## Preoperative Characterization of Borderline Epithelial Ovarian Tumors **Key Point:** MRI with contrast is the most appropriate imaging modality to characterize a suspected borderline ovarian tumor and differentiate it from invasive carcinoma or benign lesions. ### Why MRI is Superior for Borderline Tumors 1. **Soft-tissue contrast resolution** — MRI excels at depicting internal architecture, solid components, and papillary projections that characterize borderline tumors. 2. **Characterization without biopsy** — Can distinguish borderline tumors (intermediate features) from clearly benign cysts or frankly malignant masses. 3. **Staging capability** — Assesses peritoneal involvement and lymph nodes, which are critical for FIGO staging and prognostication. 4. **Reproducibility for surveillance** — Provides baseline for follow-up imaging in borderline tumors, which have a lower recurrence risk than invasive carcinomas. ### Why Other Investigations Are Suboptimal | Investigation | Limitation | |---|---| | **Serum inhibin and AMH** | Markers of ovarian reserve, not diagnostic for tumor type; not used for characterization | | **Tumor marker panel (CA-125, CEA, AFP)** | Nonspecific; elevated in benign conditions, borderline tumors, and invasive carcinomas; cannot distinguish between them | | **Fine-needle aspiration (FNA)** | Contraindicated in suspected ovarian malignancy; risk of tumor spillage and peritoneal seeding; diagnosis requires architectural assessment, not cytology alone | **Clinical Pearl:** Borderline serous tumors (BOTs) are characterized by epithelial proliferation and nuclear atypia WITHOUT stromal invasion. MRI can suggest this diagnosis by showing a predominantly cystic mass with papillary projections and minimal solid component — features that guide conservative surgical management (ovarian-sparing surgery in young women). **High-Yield:** FNA is explicitly contraindicated in suspected ovarian malignancy because of the risk of tumor seeding. Diagnosis of borderline tumors requires histopathology after surgical resection, but MRI provides the best preoperative characterization to guide the surgical approach. **Mnemonic: MRI for Ovarian Masses** — **M**orphology (cystic vs. solid), **R**isk stratification (benign vs. borderline vs. malignant), **I**nternal architecture (papillae, septations). [cite:Robbins 10e Ch 22] 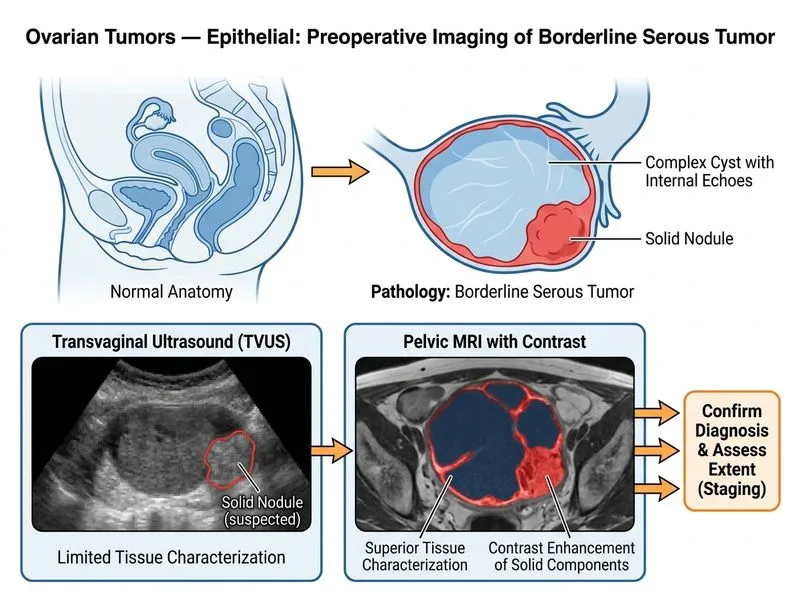
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.