## Clinical and Pathologic Integration **Key Point:** A woman of reproductive age presenting with a large, multiloculated cystic ovarian mass, ascites, elevated CA-125, and histology showing columnar mucinous epithelium with mild atypia and stratification is most consistent with mucinous cystadenocarcinoma (MCC), a low-grade epithelial ovarian malignancy. ## Mucinous Tumors of the Ovary — Spectrum | Feature | Cystadenoma | Borderline Tumor | Cystadenocarcinoma | |---------|-------------|------------------|--------------------| | **Age** | 20–50 yr | 30–50 yr | 30–50 yr | | **Size** | Variable, often large | Large (>10 cm) | Large (>10 cm) | | **CA-125** | Normal or <100 U/mL | Mildly elevated (100–300 U/mL) | Elevated (>200 U/mL) | | **Ascites** | Absent (unless rupture) | Absent or minimal | Present (pseudomyxoma peritonei if ruptured) | | **Epithelial Atypia** | Absent | Mild to moderate | Moderate to marked | | **Invasion** | None | Absent | Present (into stroma) | | **Prognosis** | Excellent (>99%) | Intermediate (~90% 5-yr OS) | Poor if ruptured (~50% 5-yr OS); better if confined (~80%) | ## Histopathologic Criteria for Mucinous Cystadenocarcinoma 1. **Epithelial lining:** Tall columnar mucinous cells (resembling intestinal epithelium) 2. **Mucin production:** Abundant intracellular and extracellular mucin (PAS+, mucicarmine+) 3. **Nuclear atypia:** Mild to moderate; nuclei enlarged, hyperchromatic, irregular membranes 4. **Stratification:** Focal to multifocal epithelial stratification (>1 layer) 5. **Stromal invasion:** Infiltration of tumor cells into ovarian stroma (key differentiator from borderline tumors) 6. **Mitotic activity:** Increased but not excessive **High-Yield:** Mucinous cystadenocarcinoma is a **low-grade malignancy**. When confined to the ovary (stage I), it has a favorable prognosis (~80–90% 5-yr OS). However, if ruptured, mucinous material spills into the peritoneum, causing pseudomyxoma peritonei (PMP) with worse outcomes. ## Why This Patient Has MCC (Not Cystadenoma or Borderline) - **Ascites + elevated CA-125 (320 U/mL)** suggests malignancy; benign cystadenoma rarely causes ascites and CA-125 is typically <100 U/mL - **Histology shows mild atypia + stratification + stromal invasion** = carcinoma (not benign cystadenoma, which has no atypia or invasion) - **Age 38 yr, reproductive age** = typical for mucinous tumors (not serous, which peaks postmenopausally) - **Large multiloculated cystic mass** = classic imaging for mucinous tumor **Clinical Pearl:** Mucinous tumors account for only ~5–10% of epithelial ovarian cancers but are the most common epithelial tumor in younger women. Always consider mucinous cystadenocarcinoma in a woman <50 yr with a large cystic ovarian mass and ascites. ## Distinction from Borderline Mucinous Tumor Borderline mucinous tumors lack stromal invasion and have better prognosis (~95% 5-yr OS if stage I). The presence of stromal invasion in this case elevates the diagnosis to cystadenocarcinoma. ## Management **Tip:** Stage I mucinous cystadenocarcinoma is treated with surgery alone (unilateral salpingo-oophorectomy ± staging). Chemotherapy is reserved for advanced or ruptured tumors. Unlike serous carcinoma, mucinous tumors are relatively chemoresistant. 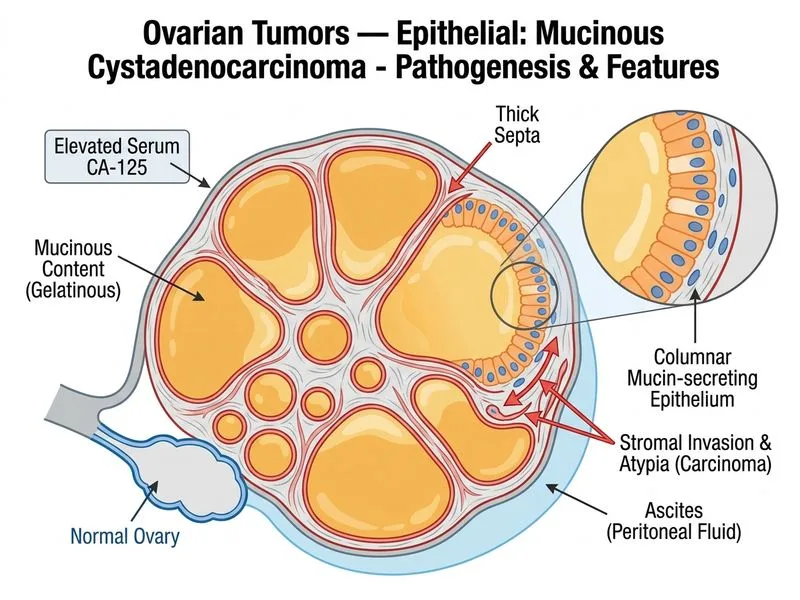
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.