## Investigation of Choice for Germ Cell Tumors ### Clinical Context The patient's presentation — young age, mixed ovarian mass, elevated β-hCG and AFP — is classic for a **mixed germ cell tumor** (dysgerminoma with yolk sac tumor elements or immature teratoma). ### Why CT Chest, Abdomen, and Pelvis? **Key Point:** Staging imaging with contrast-enhanced CT of the chest, abdomen, and pelvis is the gold standard for initial metastatic workup in ovarian germ cell tumors. 1. **Detects retroperitoneal lymph node involvement** — the most common site of metastasis in germ cell tumors 2. **Assesses lung bases** — pulmonary metastases are frequent 3. **Evaluates liver and peritoneal spread** — essential for staging (FIGO) 4. **Guides surgical planning** — determines extent of debulking and need for chemotherapy 5. **Cost-effective and widely available** — first-line staging modality ### Role of Tumor Markers | Marker | Significance in This Case | |--------|---------------------------| | β-hCG (45 mIU/mL) | Elevated → suggests trophoblastic component (yolk sac tumor or choriocarcinoma) | | AFP (120 ng/mL) | Elevated → confirms yolk sac tumor component | | Both elevated | Indicates mixed germ cell tumor; markers also used for post-treatment surveillance | **High-Yield:** Tumor markers + imaging together establish diagnosis and baseline for monitoring chemotherapy response. ### Why Not Laparoscopy or MRI? **Clinical Pearl:** Diagnostic laparoscopy risks tumor spillage and is avoided in suspected malignancy. MRI is better for local pelvic detail but does not adequately assess distant metastases. PET-CT is not first-line for germ cell tumors (better for lymphomas and epithelial cancers). [cite:Robbins 10e Ch 22] 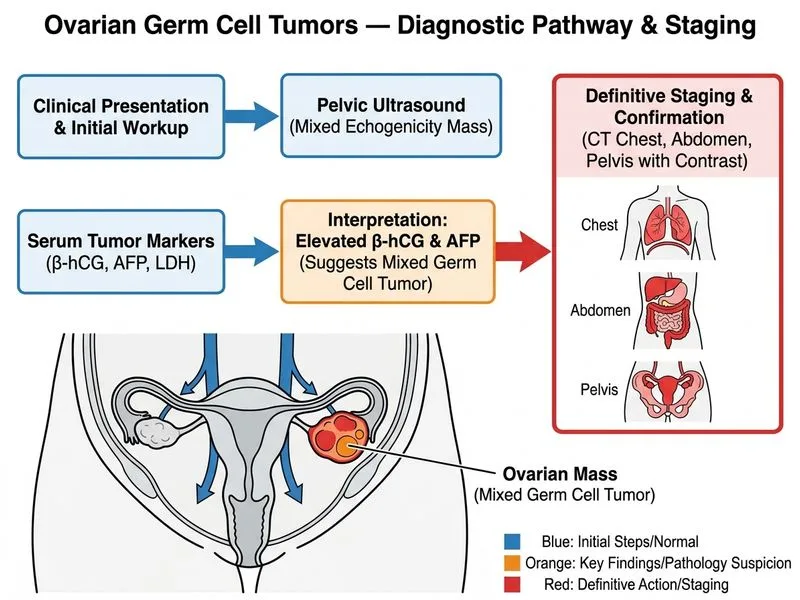
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.