## Management of Refractory Neuropathic Pain **Key Point:** When a first-line agent (gabapentin) at therapeutic doses fails to provide adequate pain relief, the evidence-based approach is either to switch to an alternative first-line agent or combine two complementary agents from different drug classes. ### Rationale for Correct Answer This patient has inadequate response to gabapentin at a reasonable dose (1800 mg/day). The next step is **combination therapy or switch to pregabalin**: - **Pregabalin** is structurally similar to gabapentin but has superior bioavailability and more predictable pharmacokinetics; switching may yield better efficacy - **Duloxetine** (an SNRI) is a first-line agent for diabetic peripheral neuropathy with a different mechanism (norepinephrine and serotonin reuptake inhibition vs. GABA modulation) - Combining gabapentin + duloxetine targets complementary pathways and is supported by clinical evidence for synergistic pain reduction **High-Yield:** First-line agents for neuropathic pain are gabapentin, pregabalin, and duloxetine. When monotherapy fails, combination therapy of agents from different classes is preferred over dose escalation alone. ### Why Not Other Options? | Approach | Limitation | |----------|------------| | Further gabapentin escalation | Diminishing returns; patient already at 1800 mg/day; side effects (sedation, ataxia) increase without proportional benefit | | Topical capsaicin alone | Appropriate as **adjunctive** therapy for localized pain, but insufficient as monotherapy for widespread bilateral neuropathy with VAS 8/10 | | Tramadol monotherapy | Opioids are not first-line for neuropathic pain; tramadol has additional SNRI activity but is reserved for refractory cases after non-opioid combination trials | **Clinical Pearl:** Diabetic peripheral neuropathy management follows a stepwise approach: optimize glycemic control → first-line pharmacotherapy (gabapentin/pregabalin/duloxetine) → combination therapy → consider tramadol or other adjuncts only if combination fails. **Mnemonic: GABA-D** — Gabapentin, pregabalin (GABA modulators) + Duloxetine (SNRI) = dual mechanism for neuropathic pain. 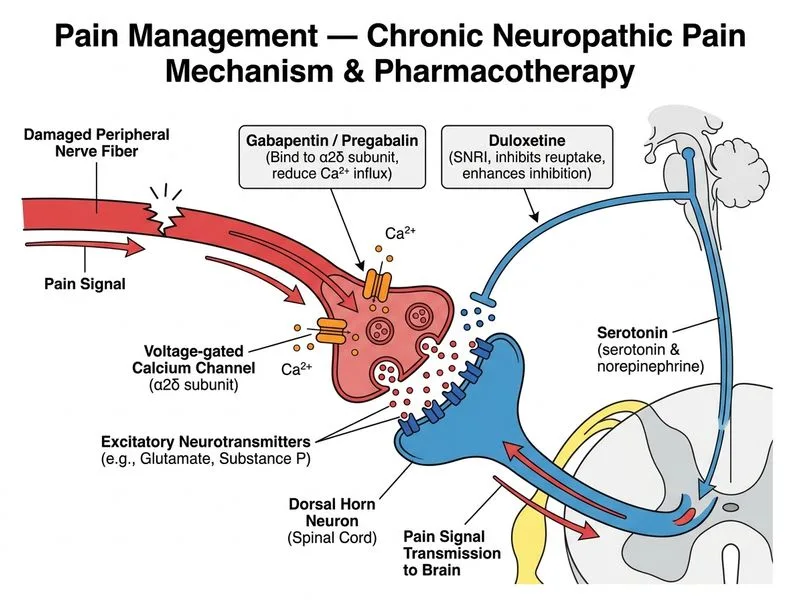
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.