## Opioid Dose Escalation in Cancer Pain **Key Point:** When a patient on chronic opioid therapy reports inadequate pain control despite good compliance and absence of side effects, the appropriate response is **opioid dose escalation** combined with breakthrough pain management, not switching agents or adding non-opioid adjuvants alone. ### Rationale for Correct Answer This patient meets criteria for opioid dose escalation: 1. **Inadequate analgesia** despite therapeutic dosing (VAS 9/10 on 120 mg morphine/day) 2. **Absence of intolerable side effects** (no nausea, constipation, or sedation) 3. **Cancer pain** (not chronic non-cancer pain) — opioid escalation is appropriate and guideline-recommended **High-Yield:** In cancer pain management, the **WHO analgesic ladder** and oncology guidelines recommend: - Step 1: Non-opioids (NSAIDs, acetaminophen) - Step 2: Weak opioids (codeine, tramadol) - Step 3: Strong opioids (morphine, fentanyl) with dose escalation as needed **Correct escalation strategy:** - Increase the **long-acting (baseline) opioid by 25–50%** (morphine 60 mg → 75–90 mg twice daily) - Provide **short-acting breakthrough opioid** (immediate-release morphine 10–20 mg every 2–4 hours as needed) - Reassess in 48–72 hours - Continue escalation until pain control achieved or intolerable side effects emerge ### Why Not Other Options? | Option | Why Incorrect | |--------|---------------| | Add adjuvant without opioid escalation | Adjuvants (gabapentin, duloxetine) are **complementary**, not alternatives to opioid escalation in cancer pain. They should be used **alongside** dose increases, not instead of them. | | Switch to fentanyl patch | Fentanyl is not more potent than morphine on a mg-for-mg basis; equianalgesic dosing applies. Switching without dose escalation would not address inadequate pain control. Fentanyl patches are appropriate for **stable** pain, not for dose titration. | | Increase morphine alone without breakthrough coverage | Escalating baseline opioid without providing short-acting breakthrough medication leaves the patient vulnerable to pain spikes and inadequate acute pain management. | **Clinical Pearl:** Cancer pain is **progressive and dynamic**. Unlike chronic non-cancer pain, opioid escalation is not only appropriate but **ethically mandated** to relieve suffering. Tolerance (requiring dose increases) is expected and does not indicate addiction in the cancer setting. **Mnemonic: ESCALATE** — Escalate opioid dose, provide Short-acting breakthrough coverage, Assess in 48–72 hours, Continue until adequate analgesia or toxicity, Adjuvants as complementary (not alternative) therapy. 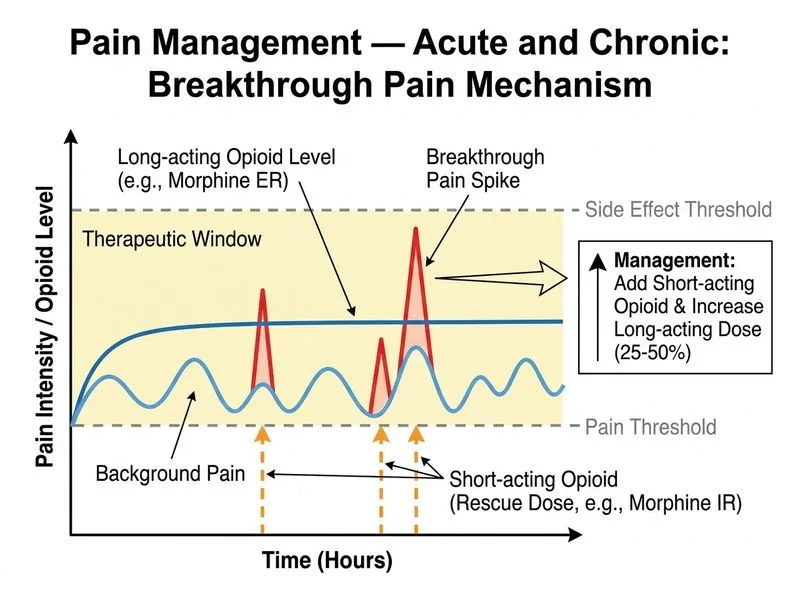
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.