## Opioid Escalation in Cancer Pain — Breakthrough and Refractory Pain **Key Point:** Severe, uncontrolled cancer pain despite adequate opioid dosing requires: 1. **Opioid rotation or escalation** (not just dose increase) 2. **Interventional pain management** (nerve blocks, infusions) 3. **Multimodal adjuvant therapy** 4. **Early palliative care involvement** ### Why IV Morphine Infusion + Celiac Plexus Block? **High-Yield:** This patient has: - **Visceral pain** (liver metastases, RUQ pain radiating to back) — classic for celiac plexus involvement - **Inadequate analgesia** on oral morphine 30 mg BD (60 mg/day total) - **Good renal function** — no contraindication to opioid escalation - **No bowel obstruction** — safe for further opioid use **Clinical Pearl:** Celiac plexus block is indicated for upper abdominal visceral pain (pancreatic, hepatic, gastric malignancy) and provides: - Rapid onset (minutes to hours) - Duration of weeks to months - Reduced opioid requirement - Improved quality of life in advanced cancer ### Opioid Escalation Strategy When oral opioids fail: 1. **IV/SC infusion** allows titration to effect without GI absorption variability 2. **Opioid rotation** (morphine → fentanyl or hydromorphone) may improve tolerability 3. **Concurrent interventional block** addresses the underlying pain mechanism **Mnemonic: SOAR** — **S**witch route (IV/SC), **O**pioid rotation, **A**djuvant therapy (gabapentin, NSAIDs), **R**egional block (celiac plexus, epidural). ### Why NOT Transdermal Fentanyl Alone? **Warning:** Fentanyl patches are: - Slow-onset (12–24 hours) - Inappropriate for acute escalation of severe, uncontrolled pain - Used for **stable, chronic** pain, not breakthrough pain - Naloxone is not standard with fentanyl patches (and addresses only constipation, not pain) ### Why NOT Simple Dose Escalation? Increasing oral morphine from 30 to 60 mg BD without addressing the underlying visceral pain mechanism is suboptimal. Visceral pain often responds better to regional blocks than to opioid escalation alone. ### Why NOT Paracetamol + Palliative Care Referral Alone? **Clinical Pearl:** While palliative care involvement is appropriate, paracetamol 4 g/day is adjunctive and insufficient for severe cancer pain. The immediate next step is **opioid escalation + interventional block**, with concurrent palliative care consultation. ## Cancer Pain Management Algorithm ```mermaid flowchart TD A[Cancer pain on opioids]:::outcome --> B{Pain controlled?}:::decision B -->|Yes| C[Maintain current regimen<br/>+ adjuvants as needed]:::action B -->|No| D{Type of pain?}:::decision D -->|Visceral<br/>RUQ/epigastric| E[Celiac plexus block<br/>+ IV opioid infusion]:::action D -->|Somatic/bone| F[Escalate opioid dose<br/>+ NSAIDs + radiotherapy]:::action D -->|Neuropathic| G[Add gabapentin/pregabalin<br/>+ opioid escalation]:::action E --> H[Reassess in 24–48 hrs]:::decision F --> H G --> H H -->|Improved| I[Continue + palliative care]:::outcome H -->|Inadequate| J[Consider opioid rotation<br/>or repeat block]:::action ``` **Adjuvant Medications for Visceral Cancer Pain:** | Agent | Indication | Mechanism | |-------|-----------|----------| | NSAIDs | Bone, soft tissue | Reduce inflammation | | Gabapentin/Pregabalin | Neuropathic component | Stabilize neuronal membrane | | Corticosteroids | Visceral inflammation | Anti-inflammatory | | Anticholinergics | Bowel colic | Reduce smooth muscle spasm | [cite:Harrison 21e Ch 385; Palliative Care Guidelines ASCO/NCCN] 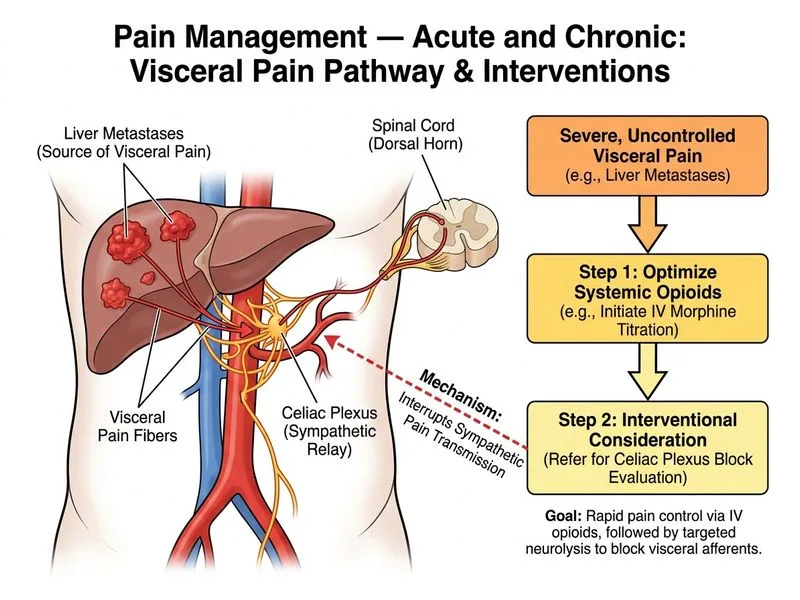
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.