## Distinguishing PHN (Neuropathic) from Post-operative Pain (Nociceptive) ### Clinical Context and Pathophysiology **Key Point:** Post-herpetic neuralgia (PHN) is a neuropathic pain condition arising from varicella zoster virus-induced nerve damage, characterized by central sensitization. Post-operative pain is acute nociceptive pain from surgical tissue trauma and inflammation. ### Comparative Analysis Table | Characteristic | Post-Herpetic Neuralgia (PHN) | Post-operative Pain | | --- | --- | --- | | **Pain Mechanism** | Neuropathic (nerve injury, central sensitization) | Nociceptive (tissue damage, inflammation) | | **Onset** | Weeks to months after herpes zoster rash | Immediate post-operatively | | **Quality** | Burning, tingling, electric, stabbing | Sharp, aching, throbbing | | **Distribution** | Dermatomal (follows nerve distribution) | Localized to surgical site | | **Allodynia/Hyperalgesia** | Present (hallmark feature) | May be present acutely | | **NSAID Response** | Poor to absent | Excellent | | **Opioid Response** | Moderate to poor | Excellent | | **Gabapentin/Pregabalin** | First-line, excellent response | Adjunctive only | | **Duloxetine (SNRI)** | Effective | Not indicated | | **Duration** | Chronic (months to years) | Acute (days to weeks) | | **Inflammatory Markers** | Minimal or absent | Elevated (CRP, IL-6) | ### Mechanism-Based Treatment Algorithm ```mermaid flowchart TD A[Chronic Pain Presentation]:::outcome --> B{Dermatomal distribution<br/>+ burning quality?}:::decision B -->|Yes| C{History of varicella<br/>zoster rash?}:::decision B -->|No| D[Nociceptive Pain]:::outcome C -->|Yes| E[Post-Herpetic Neuralgia<br/>Neuropathic]:::outcome C -->|No| F[Other Neuropathy]:::outcome E --> G[First-Line:<br/>Gabapentin/Pregabalin]:::action E --> H[Second-Line:<br/>Duloxetine, Topical Lidocaine]:::action D --> I{Acute or Chronic?}:::decision I -->|Acute| J[NSAIDs + Opioids<br/>+ Regional Blocks]:::action I -->|Chronic| K[NSAIDs + Acetaminophen<br/>+ Adjuvants]:::action ``` ### Why the Correct Answer Distinguishes These Conditions **High-Yield:** Central sensitization in PHN means: - Expanded receptive fields - Lowered pain threshold - Spontaneous ectopic discharge from damaged nerves - Poor response to peripheral-acting drugs (NSAIDs, opioids alone) - Excellent response to neuromodulators (gabapentinoids, SNRIs) **Clinical Pearl:** A patient with PHN who is given only NSAIDs and opioids will have inadequate pain control. Conversely, a post-operative patient given gabapentin alone without opioids will have inadequate acute pain relief. **Mnemonic:** **PHN = Post-herpetic Neuralgia = Poor NSAID response, Hyperalgesia/Allodynia, Neuropathic mechanism, Needs gabapentin/pregabalin** ### Pharmacological Rationale 1. **PHN (Neuropathic):** - Gabapentin 300–3600 mg/day (first-line) — modulates Ca²⁺ channels - Pregabalin 150–600 mg/day (first-line) — higher potency, faster onset - Duloxetine 60 mg/day (SNRI) — increases norepinephrine and serotonin - Topical lidocaine patch — blocks ectopic discharge locally - Opioids: only if above fail; limited efficacy 2. **Post-operative Pain (Nociceptive):** - NSAIDs (ketorolac, ibuprofen) — block COX and prostaglandins - Opioids (morphine, fentanyl) — mu-receptor agonism - Acetaminophen — central COX inhibition - Regional anesthesia (epidural, peripheral nerve blocks) — gold standard - Gabapentin: adjunctive for opioid-sparing effect [cite:Harrison 21e Ch 5; Rang & Dale's Pharmacology Ch 42; Stoelting's Pharmacology in Anesthesia Ch 15] 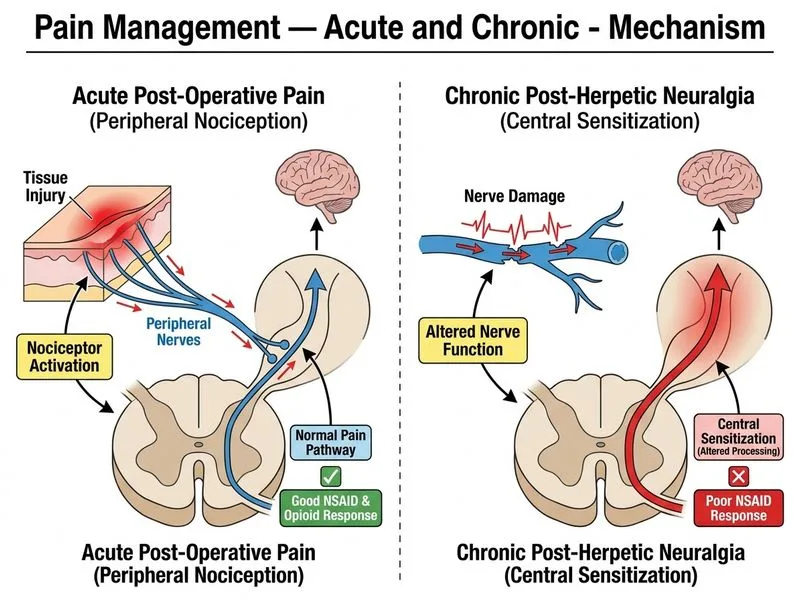
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.