## Neuropathic Pain Management in Diabetic Peripheral Neuropathy **Key Point:** Gabapentin, pregabalin, TCAs (amitriptyline), and SNRIs (duloxetine) are all recognized first-line agents for diabetic peripheral neuropathy (DPN). In this clinical scenario, gabapentin is the most appropriate choice given the patient's specific profile — but amitriptyline remains a valid co-first-line option when no contraindications exist. ### Rationale for Gabapentin (Option A) Gabapentin is an alpha-2-delta calcium channel ligand that reduces presynaptic neurotransmitter release (glutamate, substance P, norepinephrine) in pain pathways. It is: - Established as first-line for DPN (ADA Standards of Care, NICE NG173, NeuPSIG guidelines) - Well-tolerated with minimal drug–drug interactions — important in a diabetic patient on multiple medications - Safe at eGFR 78 mL/min/1.73m² (dose adjustment required only if eGFR <60) - Starting dose 300 mg once daily, titrated by 300 mg every 3 days to 1800 mg/day in divided doses (maximum 3600 mg/day) **High-Yield:** Per NeuPSIG 2015 guidelines (Finnerup et al., *Lancet Neurology*), gabapentinoids and TCAs share Grade A evidence for neuropathic pain. The choice between them is individualized based on comorbidities, tolerability, and patient factors. ### Why Gabapentin Is Preferred Over Amitriptyline in This Patient Amitriptyline (Option D) is equally first-line by guideline evidence. However, in this 58-year-old diabetic patient, gabapentin is preferred because: - **Autonomic neuropathy risk:** Diabetic patients are prone to autonomic dysfunction; amitriptyline's anticholinergic effects (urinary retention, constipation, orthostatic hypotension) can worsen this - **Cardiac safety:** TCAs carry QTc prolongation and arrhythmia risk; a baseline ECG would be required before initiating amitriptyline - **Anticholinergic burden:** Even at low doses (10–75 mg), amitriptyline contributes to anticholinergic burden, which increases with age - The distinction is **not age alone** but the combination of diabetes-related autonomic vulnerability and cardiac risk profile | Agent | Mechanism | Dose | Advantages | Cautions | |-------|-----------|------|-----------|----------| | **Gabapentin** | α2δ Ca²⁺ channel ligand | 300–3600 mg/day | Minimal interactions, renal dosing | Somnolence, dizziness | | **Pregabalin** | α2δ Ca²⁺ channel ligand | 150–600 mg/day | Faster titration | Somnolence, weight gain | | **Amitriptyline** | TCA — NE/5-HT reuptake inhibition | 10–75 mg/day | Low cost, analgesic at sub-antidepressant doses | Anticholinergic, QTc risk, autonomic effects | | **Duloxetine** | SNRI | 30–120 mg/day | FDA-approved for DPN, mood benefit | Nausea, BP elevation | ### Why Other Options Are Incorrect - **Morphine SR (Option B):** Opioids are NOT first-line for neuropathic pain. They are reserved for refractory cases after failure of multiple first-line agents, due to addiction risk, poor long-term efficacy in neuropathic conditions, and opioid-induced hyperalgesia (Harrison's Principles, 21st ed.). - **Indomethacin (Option C):** NSAIDs act on COX enzymes and are effective for nociceptive/inflammatory pain, NOT neuropathic pain. They carry additional renal and GI risks in diabetic patients and are contraindicated as a treatment strategy here. - **Amitriptyline (Option D):** Remains a valid first-line agent per guidelines. It is less preferred in *this specific patient* due to diabetic autonomic neuropathy risk and cardiac considerations — not solely because of age. **Clinical Pearl (KD Tripathi, Essentials of Medical Pharmacology, 8th ed.):** For neuropathic pain, the analgesic effect of TCAs is independent of their antidepressant effect and occurs at lower doses (10–75 mg). However, gabapentinoids are preferred when anticholinergic or cardiac risks are present. **Mnemonic:** **GPAD** = **G**abapentin / **P**regabalin / **A**mitriptyline / **D**uloxetine — the four first-line agents for neuropathic pain; individualize based on comorbidities. 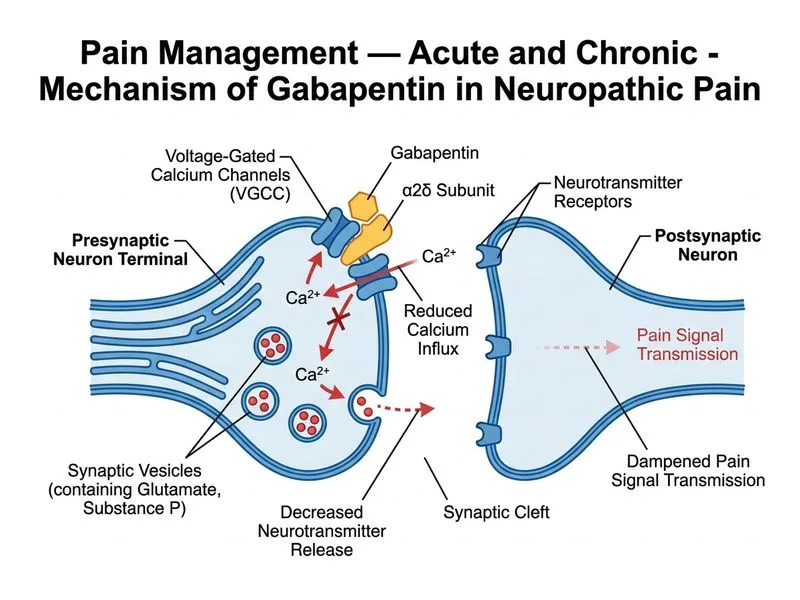
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.