## Multimodal Approach to Refractory Cancer Pain **Key Point:** Refractory cancer pain (pain uncontrolled despite adequate opioid dosing) requires a multimodal approach combining opioid escalation with non-opioid and interventional techniques, particularly regional anesthesia for localized pain. ### Assessment of This Patient's Pain The patient is on a moderate opioid dose (morphine 120 mg/day total) with: - Severe pain (9/10) despite adequate dosing - No signs of opioid toxicity or underdosing - **Localized pain** (chest wall) — a key feature suggesting regional technique benefit - Normal renal function — safe for opioid escalation **High-Yield:** Localized, somatic pain (especially chest wall, abdominal wall, or limb) is an ideal indication for regional anesthesia because it provides superior analgesia, reduces systemic opioid requirements, and improves quality of life. ### Multimodal Pain Management Strategy ```mermaid flowchart TD A[Cancer pain uncontrolled on current opioid]:::outcome A --> B{Assess pain characteristics}:::decision B -->|Localized somatic pain| C[Regional anesthetic technique]:::action B -->|Visceral/neuropathic| D[Opioid escalation + adjuvants]:::action C --> E[Intercostal nerve block / epidural]:::action E --> F[Continue opioid + PCA for breakthrough]:::action D --> G[Increase opioid dose by 25-50%]:::action G --> H[Add adjuvant: NSAID, TCA, gabapentin]:::action F --> I[Reassess in 48-72 hours]:::decision H --> I I -->|Pain controlled| J[Maintain regimen]:::outcome I -->|Pain uncontrolled| K[Escalate further or add second technique]:::action ``` ### Regional Anesthetic Techniques for Localized Cancer Pain | Technique | Indication | Duration | Benefit | |-----------|-----------|----------|----------| | **Intercostal nerve block** | Chest wall pain, rib metastases | 2–4 weeks (single shot); continuous catheter 2–4 weeks | Excellent analgesia, reduces opioid requirement | | **Epidural analgesia** | Chest, abdominal, pelvic pain | Days to weeks (continuous catheter) | Superior analgesia, allows opioid reduction | | **Paravertebral block** | Unilateral chest/abdominal pain | 2–4 weeks (single shot); continuous catheter | Localized effect, fewer systemic effects | | **Plexus block** | Limb metastases | 2–4 weeks (single shot); continuous catheter | Excellent for limb pain | **Clinical Pearl:** Regional anesthesia in palliative care is underutilized but highly effective. A single intercostal nerve block can provide 2–4 weeks of relief and allow opioid reduction, improving cognition and reducing constipation. ### Why This Approach Is Superior 1. **Localized pain** → Regional technique provides superior analgesia with lower systemic opioid exposure 2. **Opioid-sparing effect** → Reduces side effects (constipation, sedation, cognitive impairment) 3. **Multimodal principle** → Combines regional, systemic, and breakthrough analgesia 4. **Maintains current opioid dose** → Avoids unnecessary escalation while addressing root cause **Warning:** Do NOT simply escalate opioids without addressing the underlying pain mechanism. Escalating to 240 mg/day without regional technique risks opioid toxicity and poor pain control. 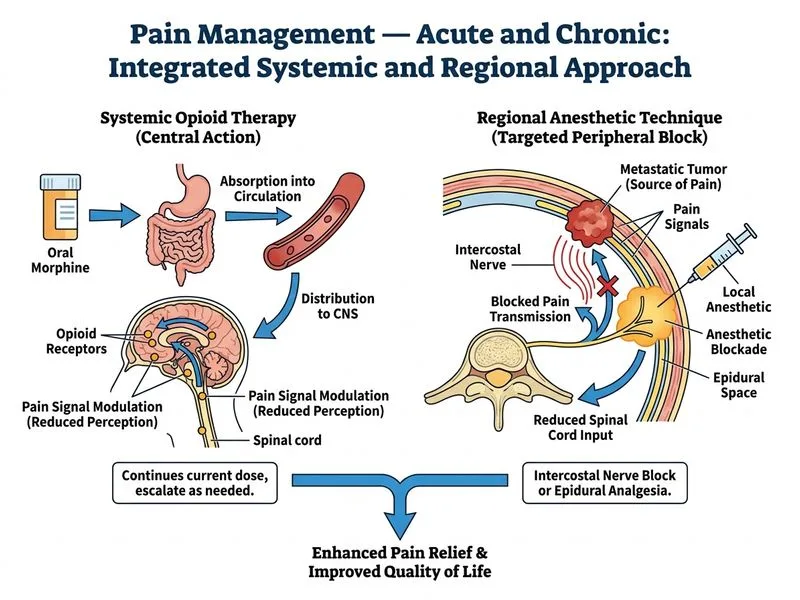
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.