## Management of Breakthrough Pain in Chronic Opioid Therapy **Key Point:** Breakthrough pain in a patient already on stable chronic opioid therapy requires a two-pronged approach: optimize the baseline analgesia AND provide rapid-onset rescue medication. ### Rationale for Correct Answer The patient is on a moderate-to-high opioid dose (60 mg morphine daily) with previously good control. Breakthrough pain suggests either: 1. Disease progression or tolerance development 2. Inadequate baseline coverage The WHO analgesic ladder and international pain guidelines recommend: - **Optimize baseline analgesia** using a long-acting formulation (transdermal fentanyl, extended-release morphine, or methadone) - **Add short-acting opioid** (immediate-release morphine or oxycodone) for breakthrough episodes Transdermal fentanyl offers: - Steady-state plasma levels (reduced fluctuations) - Better compliance (patch change every 72 hours) - Conversion: 60 mg morphine daily ≈ 25 mcg/hr fentanyl patch **Clinical Pearl:** Breakthrough pain typically requires 10–20% of the total daily opioid dose as a rescue dose, given every 2–4 hours as needed. ### Why Other Options Are Suboptimal | Option | Limitation | |--------|------------| | Increase morphine dose alone | Does not address breakthrough episodes; increases toxicity risk without rescue coverage | | Gabapentin monotherapy | Inappropriate for opioid-responsive nociceptive pain; abandons effective analgesia | | Spinal cord stimulation | Premature; reserved for refractory pain after optimized pharmacotherapy | **High-Yield:** The WHO three-step ladder emphasizes appropriate dose escalation and adjuvant use before invasive procedures. Multimodal analgesia (opioid + adjuvant) is preferred over monotherapy escalation. [cite:WHO Cancer Pain Relief Guidelines; Harrison 21e Ch 73] 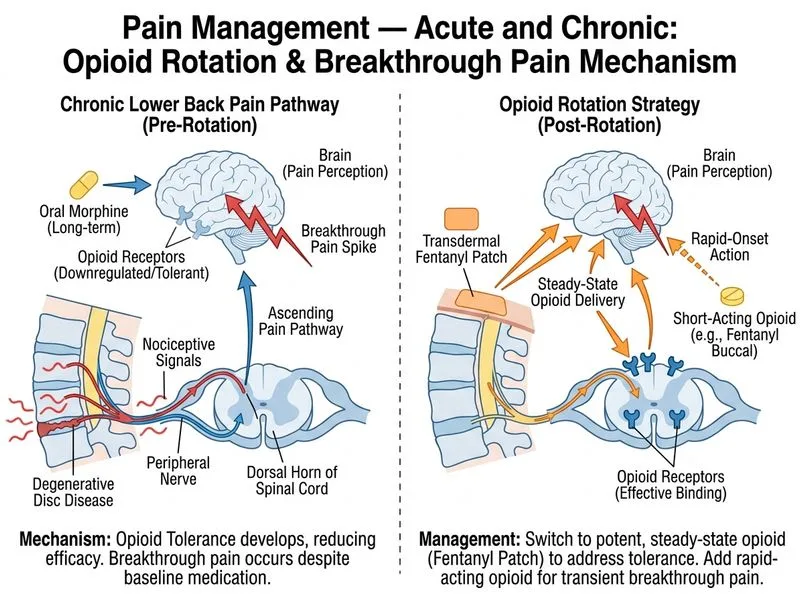
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.