## Discriminating Neuropathic from Nociceptive Pain ### Key Pathophysiology **Key Point:** Neuropathic pain arises from direct injury to or dysfunction of the somatosensory nervous system, whereas nociceptive pain results from activation of nociceptors by tissue damage or inflammation. ### Distinguishing Clinical Features | Feature | Nociceptive Pain | Neuropathic Pain | |---------|------------------|------------------| | **Allodynia & Hyperalgesia** | Absent | **Present** | | **Quality** | Dull, aching, throbbing | Burning, shooting, electric | | **Temporal Pattern** | Often intermittent | Constant, paroxysmal | | **Opioid Response** | Good | Poor to moderate | | **Inflammation Marker** | Present | Absent | | **Examination Finding** | Tenderness, swelling | Sensory loss, abnormal reflexes | ### Why Allodynia/Hyperalgesia is the Best Discriminator **High-Yield:** Allodynia (pain from normally non-painful stimuli, e.g., light touch) and hyperalgesia (exaggerated pain response to painful stimuli) are **pathognomonic** for neuropathic pain. They reflect central and peripheral sensitization—a hallmark of nerve injury or dysfunction. - In nociceptive pain, stimuli that do not activate nociceptors (e.g., gentle touch) do not cause pain. - In neuropathic pain, ectopic firing and wind-up phenomena cause pain with minimal stimulus. **Clinical Pearl:** The patient's burning quality and poor opioid response hint at neuropathic involvement (possibly from chronic pancreatitis-induced visceral neuropathy), but allodynia/hyperalgesia on examination would clinch the diagnosis and guide adjunctive therapy (gabapentin, pregabalin, duloxetine). **Mnemonic:** **ANHE** — Allodynia and Neuropathic pain go together; Hyperalgesia and Exaggerated response in neuropathy. 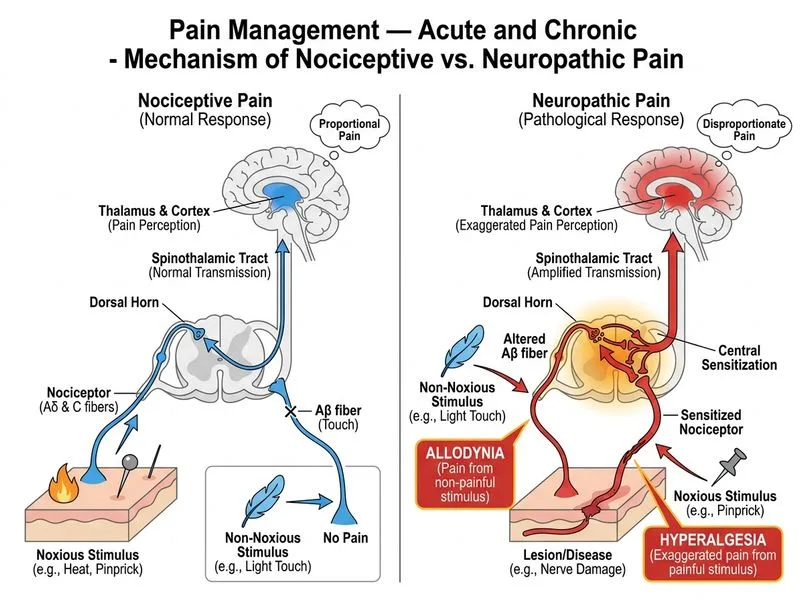
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.