## Mechanism of Capsaicin-Induced Analgesia **Key Point:** Capsaicin is a selective agonist of the transient receptor potential vanilloid 1 (TRPV1) channel, found predominantly on C-nociceptors (unmyelinated pain fibers). ### Molecular Mechanism 1. **Initial activation**: Capsaicin binds to TRPV1 receptors on C-nociceptors, causing initial depolarization and pain sensation. 2. **Sustained exposure**: Prolonged or repeated capsaicin application leads to: - Desensitization of TRPV1 receptors (reduced responsiveness) - Depletion of neuropeptide substance P from the nerve terminal - Reduced synaptic transmission in the dorsal horn of the spinal cord ### Why This Works in Diabetic Neuropathy **Clinical Pearl:** In diabetic peripheral neuropathy (DPN), C-nociceptors are preferentially affected early, making them accessible targets for capsaicin therapy. The depletion of substance P—a key neurotransmitter in pain transmission—reduces the signal reaching second-order neurons in the spinothalamic tract. ### Pathway Affected | Component | Effect | |-----------|--------| | TRPV1 receptor | Desensitized after sustained activation | | Substance P | Depleted from C-nociceptor terminals | | Dorsal horn synapse | Reduced nociceptive transmission | | Spinothalamic tract output | Decreased pain signal to brain | **High-Yield:** Capsaicin is FDA-approved as a topical analgesic patch (8%) for postherpetic neuralgia and diabetic neuropathy. Its effect is **local and peripheral**, not central. ### Why Temporary Relief? Substance P stores are gradually replenished over weeks, which is why repeated applications or patches are needed for sustained benefit. [cite:Guyton & Hall Textbook of Medical Physiology 14e Ch 48] 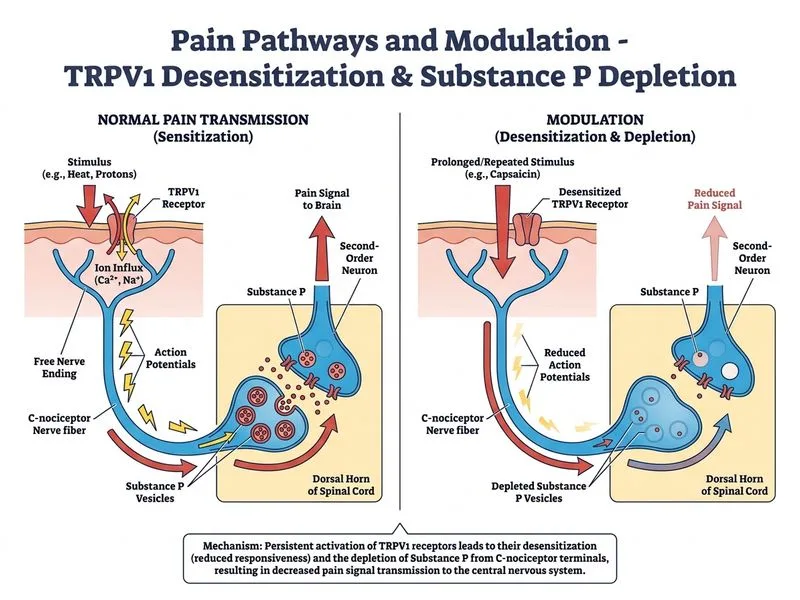
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.