## Management of Neuropathic Pain in Spinal Cord Injury ### Clinical Context This patient has central neuropathic pain (CNP) secondary to spinal cord injury—a condition where conventional analgesics are ineffective because the pain mechanism involves sensitization of dorsal horn neurons and altered inhibitory control, not peripheral nociception. ### Pathophysiology of Neuropathic Pain **Key Point:** Neuropathic pain arises from abnormal processing in the CNS due to loss of descending inhibitory control (via serotonin and norepinephrine pathways) and increased excitatory glutamatergic transmission. **High-Yield:** The gate control theory and central sensitization explain why: - NSAIDs and paracetamol are ineffective (they target peripheral inflammation, not central processing) - Gabapentinoids (pregabalin, gabapentin) reduce calcium influx and glutamate release at dorsal horn synapses - Tricyclic antidepressants (amitriptyline) enhance descending monoaminergic inhibition ### Pharmacological Approach | Drug Class | Mechanism | Evidence in CNP | Typical Dose | |---|---|---|---| | Gabapentinoids | ↓ Ca²⁺ influx, ↓ glutamate release | First-line | Pregabalin 150–600 mg/day | | Tricyclic antidepressants | ↑ Serotonin/NE reuptake inhibition | First-line | Amitriptyline 25–75 mg/day | | SNRIs | ↑ Serotonin/NE reuptake inhibition | Second-line | Venlafaxine 75–225 mg/day | | Opioids | μ-receptor agonism | Last resort (poor efficacy in CNP) | Reserved for refractory cases | | NSAIDs/Paracetamol | Peripheral COX inhibition | Ineffective | Not recommended | **Clinical Pearl:** Combination therapy (gabapentinoid + tricyclic antidepressant) targets two complementary pathways: reducing excitatory input and enhancing inhibitory output. This is superior to monotherapy in spinal cord injury pain. ### Algorithm for Neuropathic Pain Management ```mermaid flowchart TD A[Neuropathic pain diagnosis confirmed]:::outcome --> B{First-line pharmacotherapy trial}:::decision B -->|Gabapentinoid + TCA| C[Optimize doses over 4-6 weeks]:::action C --> D{Adequate response?}:::decision D -->|Yes| E[Continue maintenance therapy]:::action D -->|No| F[Add SNRI or topical agents]:::action F --> G{Refractory pain?}:::decision G -->|Yes| H[Consider SCS or intrathecal therapy]:::action G -->|No| I[Continue optimized regimen]:::action ``` **Key Point:** Spinal cord stimulation (SCS) is reserved for patients who have failed optimized pharmacotherapy (typically 6–12 weeks of combination therapy), not as an initial step. ### Why This Patient Needs Gabapentinoid + TCA 1. **Allodynia** (pain from non-noxious stimulus) indicates central sensitization—hallmark of neuropathic pain 2. **Failure of conventional analgesics** confirms non-inflammatory mechanism 3. **Evidence-based guideline:** International Spinal Cord Injury Pain guidelines recommend first-line use of gabapentinoids and antidepressants 4. **Mechanism alignment:** Both drugs restore balance between excitation and inhibition in the dorsal horn [cite:Harrison 21e Ch 394] 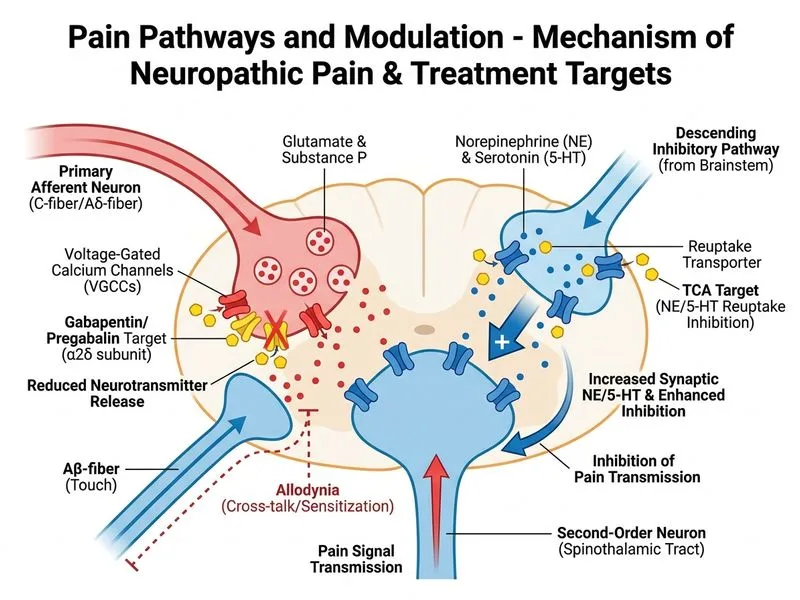
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.