## Distinguishing Papillitis from Papilloedema **Key Point:** Papillitis is inflammation of the optic nerve head (anterior optic neuritis), while papilloedema is passive swelling due to raised intracranial pressure. The clinical presentations can overlap, making imaging critical. ### Clinical Features Comparison | Feature | Papillitis | Papilloedema | |---------|-----------|---------------| | Vision loss | Early, marked (often 6/60 or worse) | Late, mild initially | | Eye pain | Present (especially on eye movement) | Absent | | Relative afferent pupillary defect (RAPD) | Present | Absent | | Disc hyperemia | Marked | Mild | | Hemorrhages | At disc margin (flame-shaped) | Peripapillary, superficial | | Exudates | Often present | Variable | | Bilateral | Usually unilateral | Usually bilateral | | VEP latency | Delayed | Normal | ### Why MRI with Contrast is Most Specific **High-Yield:** MRI with gadolinium contrast is the gold standard for confirming papillitis because it: 1. Demonstrates **optic nerve enhancement** (pathognomonic for inflammation) 2. Excludes raised intracranial pressure as the cause 3. Evaluates for demyelinating disease (MS plaques in brain white matter) 4. Assesses the entire optic pathway 5. Provides prognostic information regarding MS risk **Clinical Pearl:** Approximately 50% of patients with optic neuritis will develop MS within 15 years. Brain MRI showing demyelinating lesions increases this risk to >80%. ### Role of Other Investigations **VEP** — Confirms conduction delay but cannot distinguish papillitis from other causes of optic nerve dysfunction. **OCT** — Shows structural changes (nerve fiber layer thinning) but cannot differentiate inflammation from other pathologies. **FFA** — Shows disc leakage and vascular changes but is non-specific; cannot confirm inflammatory etiology or exclude raised ICP. **Mnemonic:** **MRI-CONFIRM** — MRI with contrast is required to confirm inflammatory optic nerve disease and rule out intracranial pathology. 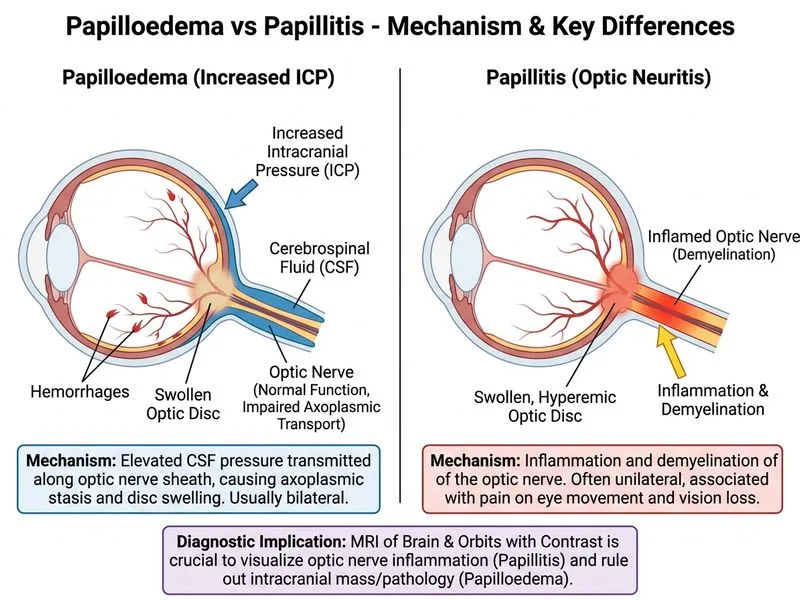
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.