## Diagnostic Approach to Papilloedema **Key Point:** Papilloedema is a sign of raised intracranial pressure (ICP), not a disease itself. The investigation of choice must identify the underlying cause of elevated ICP. ### Clinical Features of Papilloedema | Feature | Papilloedema | Papillitis | |---------|--------------|----------| | Bilateral | Yes (almost always) | No (usually unilateral) | | Vision loss | Late and mild | Early and marked | | Eye pain | Absent | Present | | RAPD | Absent | Present | | Disc appearance | Blurred margins, hyperemia, peripapillary hemorrhages | Hyperemia, flame hemorrhages at disc margin | | Symptoms | Often headache, diplopia, transient visual obscurations | Eye pain, vision loss | ### Why Neuroimaging is the Investigation of Choice **High-Yield:** Neuroimaging (MRI brain ± contrast or CT head) is essential because: 1. **Confirms papilloedema** — Shows obliteration of subarachnoid spaces, flattening of posterior globe, distension of optic nerve sheath 2. **Identifies the cause** — Brain tumors, hydrocephalus, venous sinus thrombosis, pseudotumor cerebri, infection, hemorrhage 3. **Guides management** — Treatment depends on the underlying etiology 4. **Assesses urgency** — Differentiates benign from life-threatening causes **Clinical Pearl:** **Idiopathic intracranial hypertension (IIH)** is the most common cause of papilloedema in young women. Neuroimaging must exclude secondary causes before diagnosing IIH. ### Diagnostic Algorithm for Papilloedema ```mermaid flowchart TD A[Bilateral disc swelling + blurred margins]:::outcome --> B{Asymptomatic or symptomatic?}:::decision B -->|Asymptomatic, normal VA, no pain| C[Likely papilloedema]:::outcome B -->|Eye pain, vision loss, RAPD| D[Likely papillitis]:::outcome C --> E[MRI brain ± contrast or CT head]:::action E --> F{Structural lesion found?}:::decision F -->|Yes: tumor, hydrocephalus, etc.| G[Treat underlying cause]:::action F -->|No: normal imaging| H[Suspect IIH]:::outcome H --> I[Lumbar puncture for opening pressure]:::action D --> J[MRI optic nerves with contrast]:::action J --> K[Confirm optic nerve enhancement]:::outcome ``` ### Why Other Options Are Incorrect **Perimetry** — Useful for monitoring visual field loss in chronic papilloedema but does not identify the cause of raised ICP. **OCTA** — Shows structural vascular changes but cannot assess intracranial pathology or confirm the etiology of papilloedema. **Carotid Doppler** — Relevant only if venous sinus thrombosis is suspected; not a first-line investigation for papilloedema. **Mnemonic:** **BRAIN-FIRST** — When papilloedema is suspected, image the BRAIN first to identify the cause of raised intracranial pressure. 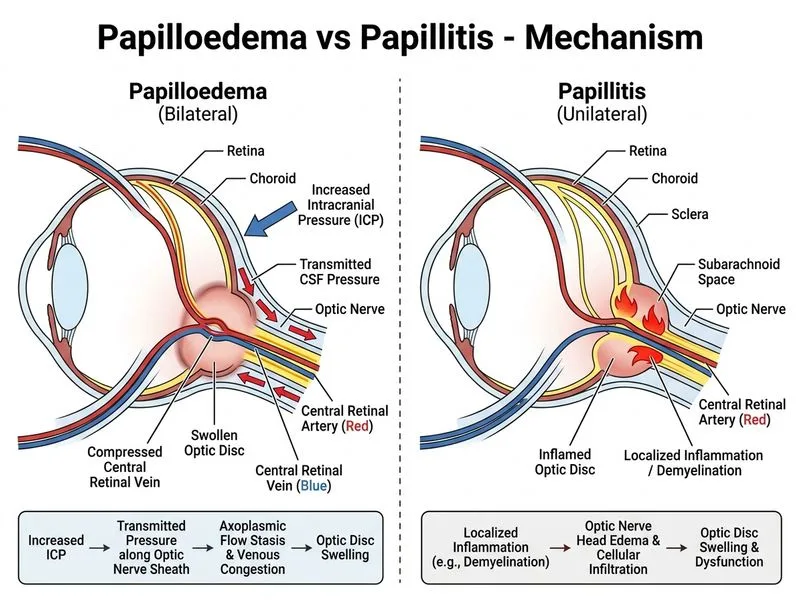
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.