## Clinical Diagnosis: Papilloedema (Raised Intracranial Pressure) This patient presents with classic papilloedema, indicating raised intracranial pressure (ICP): ### Key Distinguishing Features | Feature | Papilloedema | Papillitis | |---------|--------------|----------| | **Laterality** | Bilateral | Unilateral (usually) | | **Vision** | Preserved early; transient obscurations | Acute loss, often severe | | **Pain** | No pain on eye movement | Yes, periocular pain | | **Pupil** | Normal, no RAPD | Relative afferent defect (RAPD) | | **Disc appearance** | Pale/hyperaemic, swollen, obscured vessels | Hyperaemic, blurred margins | | **Spontaneous venous pulsations** | Lost (early sign) | Usually present | | **Aetiology** | Raised ICP (space-occupying lesion, hydrocephalus, idiopathic) | Demyelination, infection | **Key Point:** Papilloedema is optic disc swelling due to raised ICP. It is **always bilateral** and **painless**. Vision is preserved until late stages (exception: transient visual obscurations). ### Why Option D is Correct The **most appropriate next step** is to arrange **urgent neuroimaging (MRI/CT brain)** to exclude life-threatening structural causes of raised ICP — mass lesions, hydrocephalus, or venous sinus thrombosis — **combined with starting acetazolamide** as a temporizing measure to reduce CSF production. **Critical safety principle:** Lumbar puncture (Option A) is **contraindicated** in the setting of suspected raised ICP until a space-occupying lesion or obstructive hydrocephalus has been excluded by neuroimaging. Performing LP without prior imaging risks fatal transtentorial or tonsillar herniation. This is a fundamental exam-safety rule (Harrison's Principles of Internal Medicine, 21e, Ch. 379). ### Why the Other Options Are Wrong - **Option A (LP without prior imaging):** Dangerous and contraindicated. LP is appropriate *after* neuroimaging has excluded a mass lesion. The verifier's reasoning that LP is "crucial" is correct in principle but incorrect as the *first* step — imaging must precede LP. - **Option B (IV methylprednisolone):** Indicated for optic neuritis/papillitis, not papilloedema. This patient has no pain on eye movement, no RAPD, and bilateral involvement — papillitis is excluded. - **Option C (Visual fields + IOP):** Useful adjuncts in monitoring but not the urgent priority. Glaucoma causes cupping, not disc swelling with obscured vessels; IOP measurement does not address the underlying cause of papilloedema. ### Management Algorithm ``` Bilateral disc swelling + preserved vision ↓ Suspect Papilloedema (raised ICP) ↓ URGENT NEUROIMAGING (MRI/CT brain) ← FIRST STEP + Start Acetazolamide (temporizing) ↓ Mass/hydrocephalus found? → Neurosurgical referral No structural cause? → Idiopathic Intracranial Hypertension (IIH) ↓ LP (opening pressure) + Weight loss + Acetazolamide long-term ``` **High-Yield:** The sequence is: **Neuroimaging FIRST → then LP** (if no contraindication). Never reverse this order in a patient with suspected raised ICP. **Clinical Pearl:** - Loss of spontaneous venous pulsations is an **early sign** of raised ICP - Transient visual obscurations (brief, seconds-long vision loss) are pathognomonic for papilloedema - Enlarged blind spot on perimetry is characteristic - Headache + bilateral disc swelling = raised ICP until proven otherwise **Warning:** Do NOT perform LP before neuroimaging in suspected raised ICP. Do NOT assume IIH without excluding structural causes first. **Mnemonic: RAISED ICP causes of papilloedema** - **R**enal disease (hypertension) - **A**nemia (rarely) - **I**ntracranial mass / **I**diopathic intracranial hypertension - **S**inus thrombosis - **E**ncephalitis / **E**dema (cerebral) - **D**iabetes (rarely) - **I**nfection (meningitis) - **C**erebral edema - **P**ressure (raised) — hydrocephalus [cite: Harrison's Principles of Internal Medicine, 21e, Ch. 379; Kanski's Clinical Ophthalmology, 9e] 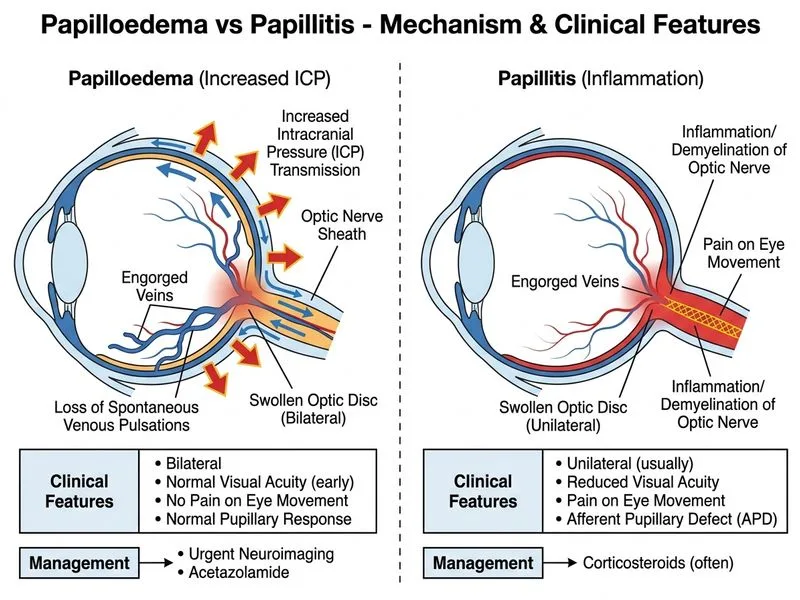
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.