## Papilloedema: Structural Confirmation ### Imaging Discriminator **Key Point:** While clinical examination can suggest papilloedema, **optic nerve sheath distension (>6 mm diameter)** on ultrasound or MRI is the structural hallmark that confirms raised intracranial pressure and papilloedema, distinguishing it from papillitis (which shows no sheath distension). ### Pathophysiology of Optic Nerve Sheath Distension **High-Yield:** Papilloedema results from **raised intracranial pressure** transmitted along the optic nerve sheath (which is continuous with the dura). This causes: 1. Compression of axoplasmic flow in the optic nerve 2. Accumulation of axoplasmic material at the disc 3. Swelling of the nerve head (true oedema) 4. **Distension of the optic nerve sheath** (pathognomonic for raised ICP) In contrast, papillitis is **local inflammation** of the optic nerve head without sheath distension. ### Comparative Imaging Findings | Modality | Papilloedema | Papillitis | |----------|--------------|------------| | **Ultrasound (A-scan)** | Optic nerve sheath >6 mm | Normal sheath diameter (<5 mm) | | **MRI Orbit** | Sheath distension, flattened posterior globe | Normal sheath, may show T2 hyperintensity of nerve | | **Fundus Photo** | Bilateral disc swelling, haemorrhages, exudates | Unilateral hyperaemia, blurred margins | | **OCT** | Elevated retinal nerve fibre layer (RNFL), buried drusen-like appearance | Elevated RNFL, but sheath normal | ### Why Imaging Matters **Clinical Pearl:** A patient with **bilateral disc swelling + normal vision + normal pupils** could have: - Papilloedema (raised ICP) - Pseudopapilloedema (optic disc drusen, tilted discs) - Bilateral papillitis (rare, e.g., neurosarcoidosis, syphilis) Imaging the **optic nerve sheath** resolves this ambiguity: - **Sheath >6 mm** → papilloedema (raised ICP) - **Normal sheath + T2 hyperintensity of nerve** → papillitis - **Drusen on imaging** → pseudopapilloedema **Mnemonic: SHEATH SIGN** - **S**welling of disc (both) - **H**yperICP (papilloedema only) - **E**xudates (both, but more in papilloedema) - **A**xonal dysfunction (papillitis only) - **T**ransaxial sheath diameter >6 mm (papilloedema only) - **H**yperICP imaging findings (MRI: empty sella, compressed ventricles) [cite:Neuro-Ophthalmology Khurana Comprehensive Ophthalmology Ch 12; Orbital Imaging Swartz & Loevner] 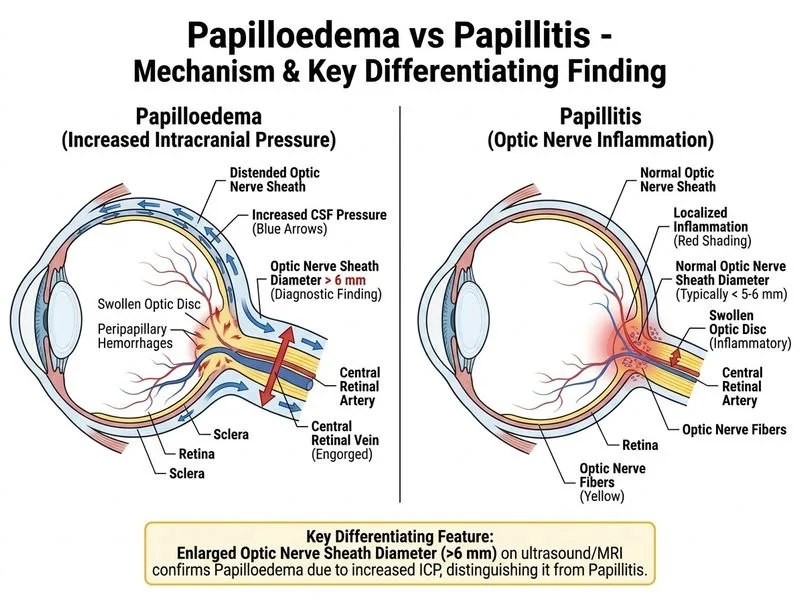
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.