## Clinical Diagnosis: Papilloedema from Raised Intracranial Pressure ### Key Distinguishing Features **Key Point:** Papilloedema is bilateral optic disc swelling due to raised intracranial pressure (ICP), presenting insidiously with progressive headache, vomiting, and blurred vision. Vision is preserved until late stages, and there is no pain on eye movement. ### Differential Diagnosis: Papilloedema vs Papillitis | Feature | Papilloedema | Papillitis | |---------|-------------|----------| | **Onset** | Insidious (weeks to months) | Acute (hours to days) | | **Vision** | Preserved until late (6/6 possible) | Markedly reduced acutely | | **Pain** | Absent | Present (pain on eye movement) | | **Laterality** | Bilateral | Unilateral | | **Disc appearance** | Swollen, blurred margins, obscured vessels, no haemorrhages initially | Hyperaemic, blurred margins, flame haemorrhages | | **Pupil response** | Normal | Relative afferent pupillary defect (RAPD) | | **Associated features** | Signs of raised ICP (headache, vomiting, CN VI palsy) | Retrobulbar inflammation, demyelinating disease | | **Cotton-wool spots** | Common | Uncommon | ### Clinical Pearl **Clinical Pearl:** The preservation of visual acuity (6/6 bilaterally) despite bilateral disc swelling is a hallmark of papilloedema and distinguishes it from papillitis, where vision is severely compromised acutely. Papilloedema is a sign of raised ICP, not a primary optic nerve disease. ### High-Yield Facts **High-Yield:** Papilloedema develops through stages: Stage 1 (hyperaemia at disc margin), Stage 2 (complete disc swelling, obscuration of vessels), Stage 3 (peripapillary haemorrhages and exudates), Stage 4 (optic atrophy with persistent disc swelling). Cotton-wool spots and retinal folds (Paton's lines) are common in advanced papilloedema. **Mnemonic:** PAPILLOEDEMA = **P**reserved vision + **A**cute headache + **P**rogressive swelling + **I**ncreased ICP + **L**ate vision loss + **L**ateral (bilateral) + **O**bscured vessels + **E**dema of disc + **D**uration weeks + **E**xudates and haemorrhages + **M**ultiple signs of raised ICP + **A**bsence of pain ### Pathophysiology of Raised ICP Common causes of papilloedema in this clinical context: 1. **Intracranial mass** (tumour, abscess, haematoma) 2. **Idiopathic intracranial hypertension (IIH)** — more common in young women 3. **Cerebral venous sinus thrombosis** 4. **Meningitis or encephalitis** 5. **Hydrocephalus** The patient's presentation (3-week progressive headache, vomiting, elevated BP) suggests a space-occupying lesion or IIH. ### Investigation Algorithm ```mermaid flowchart TD A[Bilateral disc swelling + preserved vision]:::outcome --> B{Headache + vomiting?}:::decision B -->|Yes| C[Raised ICP suspected]:::action C --> D[Neuroimaging: CT/MRI brain]:::action D --> E{Mass or hydrocephalus?}:::decision E -->|Yes| F[Neurosurgical intervention]:::action E -->|No| G[Consider IIH or CVST]:::action G --> H[LP for CSF opening pressure]:::action H --> I[Confirm papilloedema diagnosis]:::outcome ``` ### Fundoscopic Staging of Papilloedema | Stage | Features | |-------|----------| | **1** | Hyperaemia at disc margin (nasal > temporal), obscuration of nasal vessels | | **2** | Complete disc swelling, obscuration of all vessels at disc, peripapillary halo | | **3** | Peripapillary haemorrhages, exudates, Paton's lines (retinal folds) | | **4** | Optic atrophy with persistent disc swelling, gliosis | ### Key Investigations - **Neuroimaging (CT/MRI brain):** To identify cause of raised ICP - **Lumbar puncture:** If imaging normal and IIH suspected; opening pressure >25 cm H₂O confirms diagnosis - **Visual fields:** Peripheral constriction in chronic papilloedema - **OCT:** Shows optic nerve head elevation and peripapillary changes [cite:Neuro-Ophthalmology, Kanski & Bowling 8e Ch 8; Harrison 21e Ch 428] 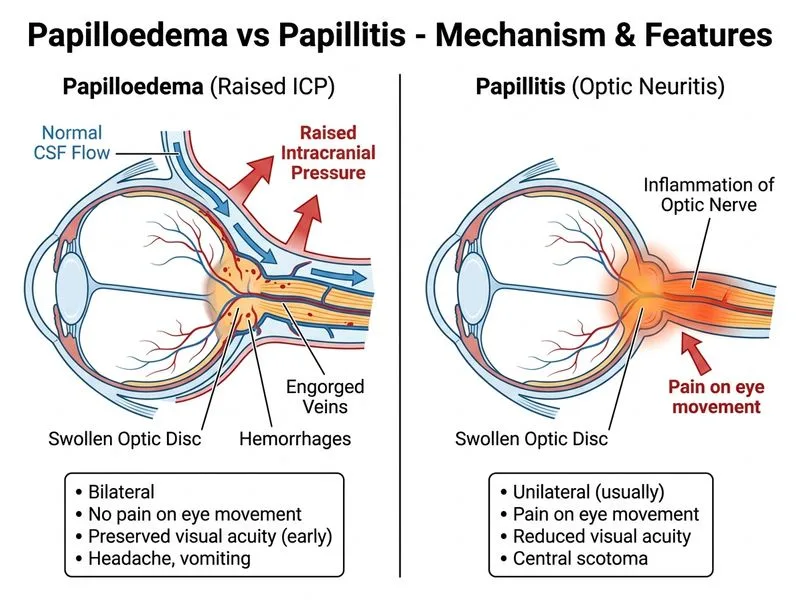
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.