## Distinguishing Optic Neuritis from Papilloedema: Investigation of Choice ### Clinical Presentation Analysis The patient presents with: - Acute unilateral vision loss with pain on eye movements (pathognomonic for optic neuritis) - Hyperaemic optic disc with blurred margins - Flame-shaped haemorrhages While the fundoscopic appearance may superficially resemble papilloedema, the **acute unilateral presentation with pain on eye movements** is diagnostic of optic neuritis, not papilloedema (which is bilateral, painless, and develops gradually). ### Why MRI Brain and Orbits with Contrast is the Investigation of Choice **Key Point:** MRI with contrast is the gold standard for confirming optic neuritis and detecting demyelinating lesions in the optic nerve and brain. 1. **Demyelinating lesion detection**: Identifies T2-weighted hyperintense lesions in the optic nerve consistent with demyelination 2. **CNS demyelination screening**: Detects asymptomatic brain lesions that predict conversion to multiple sclerosis (MS) — approximately 50% of optic neuritis patients have brain lesions on MRI 3. **Prognostic value**: Presence of brain lesions increases MS risk from ~25% to ~75% over 15 years 4. **Excludes structural causes**: Rules out compressive lesions, tumours, or other structural pathology ### Comparison with Other Investigations | Investigation | Role in Optic Neuritis | Limitation | |---|---|---| | **MRI brain/orbits + contrast** | Gold standard; detects demyelination | — | | OCT optic nerve head | Quantifies axonal loss; useful for monitoring | Cannot diagnose acute demyelination; shows structural changes only | | FFA | Shows optic nerve hyperfluorescence in papillitis | Non-specific; cannot differentiate optic neuritis from papilloedema reliably | | CT head | Rapid; excludes acute intracranial pathology | Low sensitivity for demyelination; radiation exposure | **High-Yield:** In optic neuritis, MRI is essential because: - It confirms demyelination - It stratifies MS risk - It guides long-term management and counselling ### Papilloedema vs Papillitis: Key Distinguishing Features **Key Point:** The clinical presentation (acute unilateral pain with vision loss) already excludes papilloedema, but MRI confirms the diagnosis by showing demyelination. | Feature | Papilloedema | Papillitis (Optic Neuritis) | |---|---|---| | **Onset** | Gradual (weeks to months) | Acute (hours to days) | | **Laterality** | Bilateral | Unilateral | | **Pain** | Absent | Present (pain on eye movements) | | **Vision loss** | Late, peripheral field first | Early, central scotoma | | **MRI finding** | Normal (unless underlying cause) | T2 hyperintense lesion in optic nerve | | **Prognosis** | Depends on underlying cause | ~50% convert to MS | **Clinical Pearl:** The presence of **pain on eye movements** is the single most useful clinical sign to differentiate optic neuritis from papilloedema. Papilloedema is painless; optic neuritis is painful. 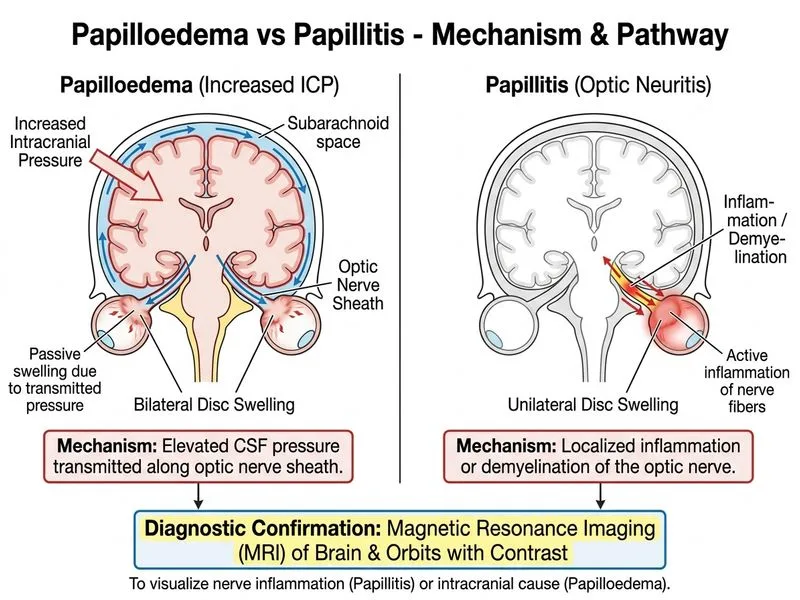
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.