## Investigation of Choice: Papilloedema vs Bilateral Papillitis ### Clinical Presentation Analysis The patient presents with: - **Bilateral optic disc swelling** with obscured margins - **Progressive course over 2 weeks** - **Preserved visual acuity** (6/6 bilaterally) - **Headaches** (suggesting raised intracranial pressure) - **No haemorrhages or exudates** (atypical for papillitis) This presentation is consistent with **papilloedema** (raised intracranial pressure) rather than bilateral papillitis, but the investigation must: 1. Confirm papilloedema 2. Identify the underlying cause of raised ICP 3. Exclude bilateral demyelinating optic neuritis ### Why MRI Brain with and without Contrast is the Investigation of Choice **Key Point:** MRI brain with and without contrast is the gold standard for investigating papilloedema because it identifies the underlying cause of raised intracranial pressure and excludes demyelinating disease. **High-Yield:** MRI brain findings in papilloedema include: - Enlarged blind spot - Flattening of the posterior globe - Optic nerve sheath distension (>6 mm) - Tonsillar herniation (if severe) - Identification of mass, hydrocephalus, venous sinus thrombosis, or idiopathic intracranial hypertension (IIH) ### Differential Diagnosis: Papilloedema vs Bilateral Papillitis | Feature | Papilloedema | Bilateral Papillitis | |---|---|---| | **Onset** | Gradual (weeks to months) | Acute to subacute (days to weeks) | | **Laterality** | Bilateral (symmetric) | Bilateral but often asymmetric | | **Pain** | Absent | Present (pain on eye movements) | | **Visual acuity** | Preserved until late | Early loss (central scotoma) | | **Headaches** | Present (due to raised ICP) | Absent | | **Haemorrhages/exudates** | Often present | Rare | | **MRI brain finding** | Structural cause of raised ICP | Normal or demyelinating lesions | | **Optic nerve sheath** | Distended (>6 mm) | Normal | **Clinical Pearl:** In this case, **preserved visual acuity with gradual bilateral disc swelling and headaches** strongly suggests papilloedema from raised ICP, not bilateral papillitis (which would present with acute vision loss and pain on eye movements). ### Why MRI is Superior to Other Investigations **Key Point:** MRI identifies the underlying cause of papilloedema, which is essential for management. ```mermaid flowchart TD A[Bilateral optic disc swelling]:::outcome --> B{Clinical features?}:::decision B -->|Gradual onset, preserved VA, headache| C[Suspect papilloedema]:::outcome B -->|Acute onset, vision loss, pain| D[Suspect papillitis]:::outcome C --> E[MRI brain with contrast]:::action E --> F{Findings?}:::decision F -->|Mass, hydrocephalus, venous thrombosis| G[Treat underlying cause]:::action F -->|Normal imaging + clinical criteria| H[Idiopathic intracranial hypertension]:::outcome D --> I[MRI brain + orbits]:::action I --> J[Detect demyelinating lesions]:::outcome ``` ### Comparison of Investigations | Investigation | Role | Limitation | |---|---|---| | **MRI brain ± contrast** | Gold standard; identifies cause of raised ICP; detects demyelination | — | | FFA | Shows optic nerve hyperfluorescence | Non-specific; does not identify underlying cause; no structural information | | OCT optic nerve head | Quantifies optic nerve swelling and axonal loss | Cannot identify cause of raised ICP; does not differentiate papilloedema from papillitis | | B-scan ultrasound | Measures optic nerve sheath diameter | Operator-dependent; does not identify underlying cause; poor soft-tissue contrast | **High-Yield:** In papilloedema, MRI must identify: - **Space-occupying lesion** (tumour, abscess) - **Hydrocephalus** (obstruction to CSF flow) - **Venous sinus thrombosis** (impaired venous drainage) - **Idiopathic intracranial hypertension** (IIH — diagnosis of exclusion) ### Clinical Pearls **Clinical Pearl:** The **absence of pain on eye movements** and **preserved visual acuity** in this patient make bilateral papillitis unlikely. Papillitis typically presents with acute vision loss and pain. **Warning:** Do not confuse papilloedema (raised ICP) with papillitis (inflammation of the optic nerve). The clinical presentation and MRI findings are distinctly different. 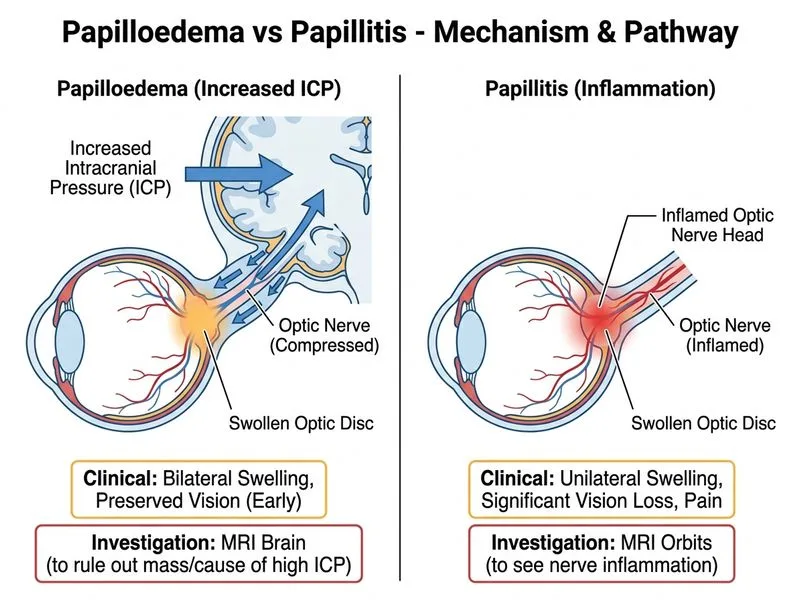
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.