## Clinical Diagnosis: Optic Neuritis (Papillitis) The clinical presentation is classic for **optic neuritis** (inflammation of the optic nerve head): - Acute unilateral vision loss with pain on eye movement (retrobulbar component) - Relative afferent pupillary defect (RAPD) indicating optic nerve dysfunction - Disc hyperaemia with peripapillary haemorrhages (papillitis = optic neuritis with visible disc involvement) - Normal intraocular pressure excludes acute glaucoma ### Differential: Papilloedema vs Papillitis | Feature | Papilloedema | Papillitis | |---------|--------------|----------| | **Onset** | Insidious (weeks–months) | Acute (hours–days) | | **Vision** | Often normal initially | Acute loss, central scotoma | | **Pain** | Absent | Present (periocular, on eye movement) | | **RAPD** | Absent (bilateral) | Present (unilateral) | | **Cause** | Raised ICP | Demyelination, infection, inflammation | | **Prognosis** | Depends on ICP cause | Often good with treatment | ## Management Algorithm for Suspected Optic Neuritis ```mermaid flowchart TD A["Acute unilateral vision loss<br/>+ disc hyperaemia + pain"]:::outcome --> B{"MRI brain & orbits<br/>already done?"}:::decision B -->|No| C["Urgent MRI brain & orbits<br/>to exclude MS, tumour, infection"]:::action C --> D{"Lesion found?"}:::decision D -->|Yes| E["Treat underlying cause<br/>+ IV methylprednisolone"]:::action D -->|No| F["Consider LP if MS risk<br/>or atypical features"]:::action B -->|Yes, normal| G["Oral corticosteroids<br/>+ VEP + MRI spine"]:::action E --> H["Neurology referral"]:::action F --> H G --> H ``` ## Next Step Rationale **Key Point:** The ONTT (Optic Neuritis Treatment Trial) and current neuro-ophthalmology guidelines recommend: 1. **MRI brain and orbits** (first-line imaging) - Excludes demyelinating lesions, intracranial mass, infection - Identifies white matter lesions (MS risk stratification) - Assesses optic nerve enhancement 2. **Lumbar puncture** (conditional) - Performed if MRI is normal AND MS is suspected - Identifies oligoclonal bands, elevated IgG index - Not routine in all cases; reserved for diagnostic uncertainty 3. **Visual Evoked Potentials (VEP)** - Confirms demyelinating conduction block - Prognostic value; delayed latency 4. **Corticosteroids** - Initiated after imaging (to avoid masking serious pathology) - Oral prednisolone 1 mg/kg/day × 2 weeks, then taper - IV methylprednisolone if severe vision loss or atypical presentation **High-Yield:** Option 3 (oral steroids + VEP) skips neuroimaging — **dangerous** because it does not exclude intracranial lesions (MS, tumour, infection). Option 1 (MRI alone) is incomplete; LP may be needed if imaging is normal. Option 2 (LP first) is not standard — imaging must precede LP to exclude mass effect. **Clinical Pearl:** Periocular pain with eye movement is the hallmark of retrobulbar optic neuritis and strongly suggests demyelination, not papilloedema (which is painless). **Warning:** Do NOT give corticosteroids before imaging — you may mask or delay diagnosis of a treatable mass or infection. [cite:Harrison 21e Ch 428] 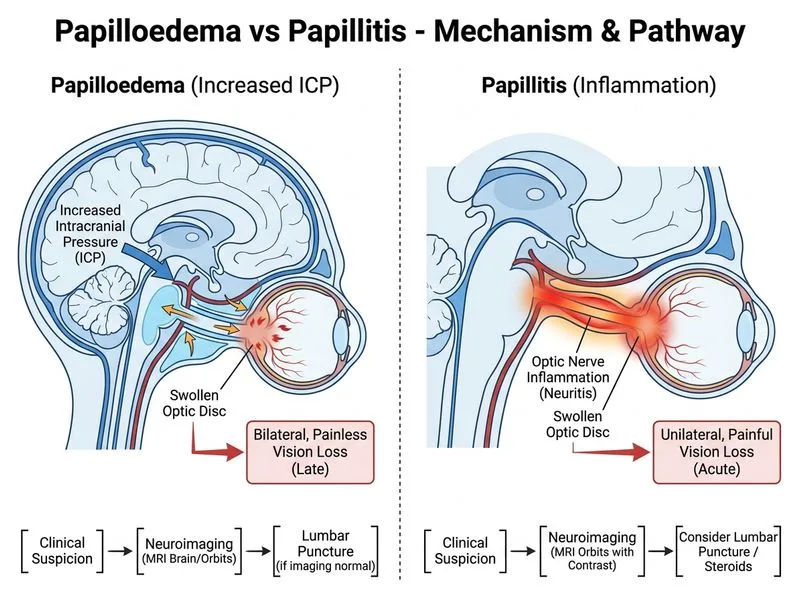
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.