## Clinical Diagnosis: Papilloedema Secondary to Hypertensive Retinopathy The presentation is consistent with **papilloedema from chronic raised intracranial pressure (ICP)** secondary to **hypertensive encephalopathy** or **malignant hypertension**: - Bilateral disc swelling (papilloedema is always bilateral) - Insidious onset over weeks (typical of chronic ICP elevation) - Retinal haemorrhages, cotton-wool spots, hard exudates (hypertensive retinopathy) - Normal IOP (excludes glaucoma) - Relatively preserved vision (6/9 — early papilloedema) - History of chronic hypertension (predisposing factor) ### Differential: Papilloedema vs Papillitis | Feature | Papilloedema | Papillitis | |---------|--------------|----------| | **Onset** | Insidious (weeks–months) | Acute (hours–days) | | **Bilateral** | Always | Unilateral | | **Pain** | Absent | Present (periocular, on eye movement) | | **RAPD** | Absent | Present (unilateral) | | **Vision** | Often normal initially | Acute loss, central scotoma | | **Cause** | Raised ICP (tumour, pseudotumour, hydrocephalus, hypertension) | Demyelination, infection, inflammation | | **Associated findings** | Obscured disc margins, Paton's lines, enlarged blind spot | Disc hyperaemia, peripapillary haemorrhages | ## Hypertensive Retinopathy Grading (Keith-Wagener-Barker) | Grade | Findings | ICP Status | |-------|----------|----------| | **I** | Arteriolar narrowing, AV nicking | Normal | | **II** | Grade I + arteriovenous nicking, copper/silver wire arterioles | Normal | | **III** | Grade II + flame haemorrhages, cotton-wool spots, hard exudates | Elevated ICP | | **IV** | Grade III + papilloedema, macular star exudates | Severely elevated ICP | **This patient has Grade IV hypertensive retinopathy with papilloedema.** ## Management Algorithm ```mermaid flowchart TD A["Bilateral disc swelling<br/>+ hypertensive retinopathy<br/>+ normal IOP"]:::outcome --> B{"Acute symptoms?<br/>Headache, confusion, seizures?"}:::decision B -->|Yes| C["Hypertensive emergency<br/>IV antihypertensives<br/>Stat imaging"]:::urgent B -->|No| D{"BP severely elevated?<br/>> 180/120 mmHg?"}:::decision D -->|Yes| E["Urgent antihypertensive therapy<br/>Target BP <140/90 in 24 hrs"]:::action D -->|No| F["Aggressive oral antihypertensives<br/>Target <140/90 mmHg"]:::action C --> G["CT/MRI head to exclude<br/>other causes of ICP elevation"]:::action E --> H["Ophthalmology follow-up<br/>in 1–2 weeks"]:::action F --> H G --> H ``` ## Why This Is Papilloedema (Not Papillitis) **Key Point:** The diagnosis is **papilloedema from hypertensive encephalopathy**, not papillitis, because: 1. **Bilateral disc swelling** — papillitis is always unilateral 2. **Insidious onset** — papillitis is acute (hours–days) 3. **No pain** — papillitis causes periocular pain on eye movement 4. **Hypertensive retinopathy** — flame haemorrhages, cotton-wool spots, hard exudates are classic for hypertension-induced ICP elevation 5. **No RAPD** — papillitis causes RAPD; papilloedema does not ## Next Step Rationale **High-Yield:** The correct management is **aggressive antihypertensive therapy** because: 1. **Papilloedema in this context is secondary to hypertension**, not a primary CNS lesion 2. **Lowering BP is both diagnostic and therapeutic** — if papilloedema resolves with BP control, the diagnosis is confirmed 3. **Imaging is NOT the first step** in uncomplicated hypertensive papilloedema (it is in acute papillitis or atypical cases) 4. **Acetazolamide is contraindicated** in hypertensive papilloedema — it does not address the underlying cause 5. **Close ophthalmology follow-up** monitors disc resolution and detects complications (optic atrophy, macular star) **Clinical Pearl:** Papilloedema from hypertension typically resolves within 4–8 weeks of adequate BP control. Disc margins become sharp again, haemorrhages resorb, and exudates fade. **Warning:** Do NOT perform lumbar puncture or neuroimaging as the first step in suspected hypertensive papilloedema. Imaging is reserved for atypical presentations, acute encephalopathy, or failure to improve with BP control. [cite:Harrison 21e Ch 428; Kanski & Bowling Clinical Ophthalmology 9e Ch 13] 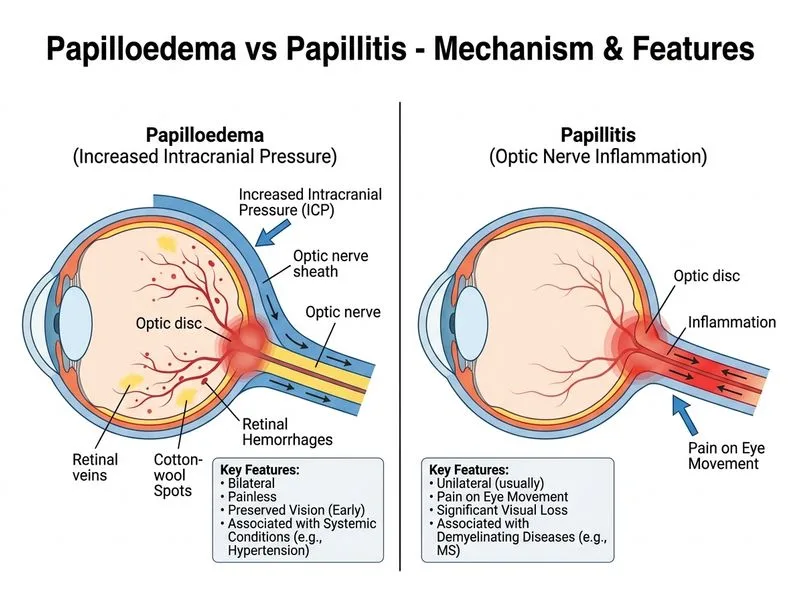
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.