## Levodopa-Induced Dyskinesia vs. Parkinson Dystonia: Clinical Discrimination ### Definition and Timing **Key Point:** Levodopa-induced dyskinesia (LID) is a **dose-dependent involuntary movement disorder** that correlates with **peak plasma levodopa levels**, whereas Parkinson dystonia occurs during **off-medication periods** (early morning or end of dose interval). ### Comparative Table: LID vs. Dystonia in Parkinson Disease | Feature | Levodopa-Induced Dyskinesia (LID) | Parkinson Dystonia | |---------|-----------------------------------|-------------------| | **Timing** | Peak-dose dyskinesia (at max drug level) | Off-medication (early morning, end of dose) | | **Morphology** | Writhing, choreoathetoid, ballistic movements | Sustained muscle contractions, twisted postures | | **Body distribution** | Generalized (limbs, trunk, face) | Focal or segmental (foot, hand, neck) | | **Dose relationship** | Increases with higher levodopa doses | Improves with levodopa dose | | **Duration of PD** | Develops after 4–5 years of levodopa therapy | Can occur early, especially in young-onset PD | | **Management** | Reduce levodopa dose, add amantadine, DBS | Increase levodopa frequency, add anticholinergics | | **Pathophysiology** | Pulsatile dopaminergic stimulation → sensitization of striatal neurons | Inadequate dopaminergic tone in off-medication state | ### High-Yield Discriminator **High-Yield:** The **temporal relationship to medication** is the single best discriminator: - **LID** = **ON-medication** (peak-dose dyskinesia) or **biphasic dyskinesia** (at dose onset/offset) - **Dystonia** = **OFF-medication** (early morning, end of dose interval) ### Clinical Pearl **Clinical Pearl:** A patient who develops **writhing movements 1–2 hours after taking levodopa** (when drug levels peak) has **LID**. A patient with **foot inversion or hand cramping in the early morning before the first dose** has **off-medication dystonia**. ### Pathophysiology Insight **Mnemonic: PULSATILE** — The mechanism of LID: - **P**ulsatile dopaminergic stimulation (not continuous, as in healthy brain) - **U**nder-regulation of postsynaptic D1 and D2 receptors - **L**oss of buffering capacity in striatum (degeneration of nigrostriatal neurons) - **S**ensitization of medium spiny neurons to dopamine surges - **A**bnormal gene expression (ΔFosB, c-fos) - **T**ransduction cascades amplify dyskinesia risk - **I**nvoluntary movements emerge after 4–5 years - **L**evodopa dose and frequency are key risk factors - **E**arly intervention with lower doses, longer intervals, or dopamine agonists reduces risk ### Management Implications 1. **For LID:** Reduce levodopa dose, extend dosing intervals, add amantadine (NMDA antagonist), or consider DBS. 2. **For Dystonia:** Increase levodopa frequency, add anticholinergics (benztropine), or optimize dopaminergic therapy. [cite:Harrison 21e Ch 430; KD Tripathi 8e Ch 12] 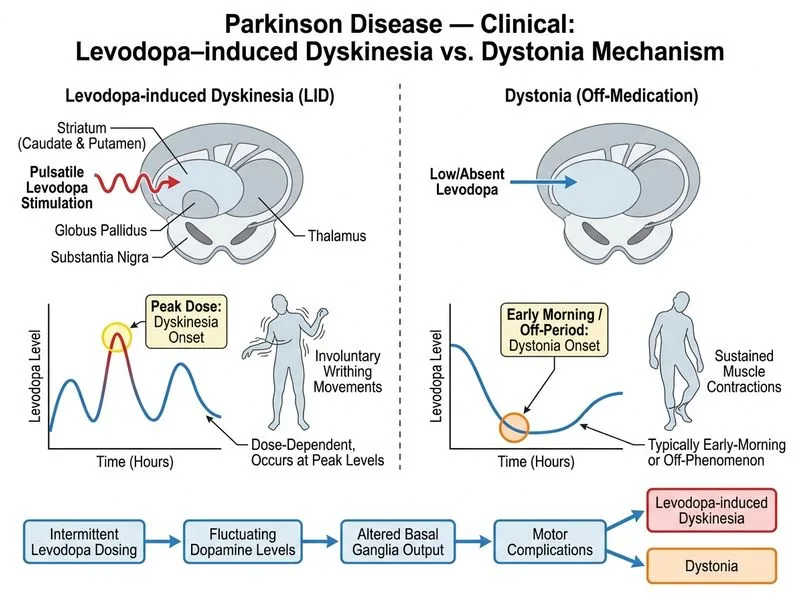
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.