## Levodopa-Induced Dyskinesia: Recognition and Management **Key Point:** Levodopa-induced dyskinesia (LID) is a predictable motor complication that emerges after 4–6 years of levodopa therapy in ~40% of patients. **Peak-dose dyskinesia** (choreiform movements at maximum drug levels) is the most common type and is managed by dose reduction and adjunctive dopaminergic agents — NOT anticholinergics or immediate surgery. ### Classification of Levodopa-Induced Dyskinesia | Type | Timing | Mechanism | Management | |------|--------|-----------|-------------| | **Peak-dose dyskinesia** | 2–3 hrs after dose (at Cmax) | Excessive dopamine stimulation | ↓ Dose, add DA agonist, MAO-B inhibitor, COMT inhibitor | | **Diphasic dyskinesia** | Early and late phases of dose cycle | Nonlinear dopamine dynamics | Smaller, more frequent doses | | **Off-period dyskinesia** | When drug levels are low | Sensitization to dopamine | Add longer-acting agents (DA agonist, patch) | **High-Yield:** In this patient, the **choreiform movements synchronous with peak drug levels** (2–3 hours post-dose) confirm **peak-dose dyskinesia**. The standard approach is: 1. **Reduce levodopa dose** (e.g., from 500 mg to 375–400 mg per dose) 2. **Add a dopamine agonist** (pramipexole, ropinirole) or **MAO-B inhibitor** (rasagiline, selegiline) to extend dopaminergic effect and reduce levodopa requirement 3. **Consider COMT inhibitor** (entacapone, tolcapone) if further optimization needed ### Pathophysiology of LID After prolonged levodopa exposure, dopamine neurons develop **pulsatile dopamine receptor stimulation** (loss of buffering capacity) → abnormal striatal plasticity → dyskinesia. This is NOT reversible by stopping levodopa; it requires **dose optimization** and **adjunctive agents** to smooth dopaminergic delivery. **Clinical Pearl:** Dyskinesia severity correlates with cumulative levodopa dose and disease duration, not with current dose alone. Reducing dose while adding a dopamine agonist or MAO-B inhibitor maintains motor control while reducing dyskinesia risk. ### Why Each Distractor Fails - **Benztropine (anticholinergic):** Worsens dyskinesia and is contraindicated in LID. Anticholinergics may help tremor but exacerbate choreiform movements. - **Entacapone monotherapy:** COMT inhibitors prolong levodopa half-life but do NOT eliminate dyskinesia if levodopa dose is not reduced. Monotherapy is ineffective. - **Immediate DBS:** Reserved for motor fluctuations and dyskinesia refractory to medical optimization (typically after 5–10 years of failed pharmacotherapy). This patient is only 5 years into PD and has not yet tried dose reduction + adjunctive agents. **Mnemonic:** **"DAME"** for LID management: - **D**ose reduction - **A**gonist addition (DA agonist) - **M**AO-B inhibitor - **E**ntacapone (COMT inhibitor) ## Algorithm for Managing Motor Complications ```mermaid flowchart TD A["Levodopa-induced dyskinesia"]:::outcome --> B{"Type of dyskinesia?"}:::decision B -->|"Peak-dose"|C["Reduce levodopa dose"]:::action B -->|"Diphasic"|D["Smaller, frequent doses"]:::action B -->|"Off-period"|E["Add longer-acting agent"]:::action C --> F["Add DA agonist or MAO-B inhibitor"]:::action D --> F E --> F F --> G{"Controlled?"}:::decision G -->|"Yes"|H["Continue medical management"]:::outcome G -->|"No after 6 months"|I["Consider DBS evaluation"]:::action I --> J["DBS if refractory"]:::action ``` [cite:Harrison 21e Ch 427; Movement Disorders Society Guidelines on Levodopa-Induced Dyskinesia] 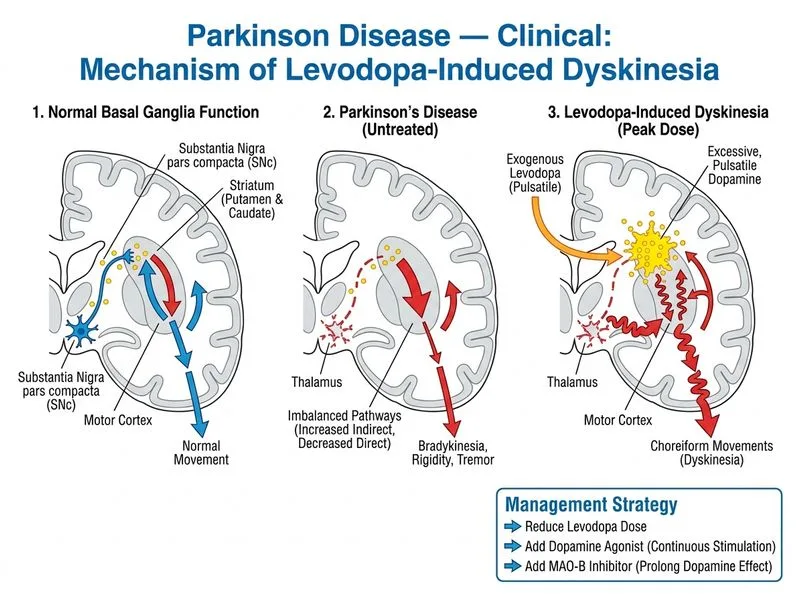
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.