## Postoperative Facial Nerve Paralysis: Immediate Next Step **Key Point:** Complete facial paralysis occurring within 24 hours of parotidectomy — especially when the nerve was identified and traced intraoperatively — demands urgent imaging (MRI or CT) to rule out a surgically correctable cause such as hematoma or edema compressing the nerve before any other intervention. ## Why Urgent MRI is the Most Appropriate Immediate Next Step **High-Yield:** The differential for immediate post-parotidectomy facial paralysis includes: - **Hematoma** compressing the facial nerve — surgically reversible if identified early - **Edema** around the nerve — managed conservatively - **Neurapraxia** — conduction block from traction/manipulation, fully reversible - **Axonotmesis or Neurotmesis** — more severe injury requiring longer-term planning Urgent MRI of the parotid region is the **most appropriate immediate next step** because: 1. It identifies a compressive hematoma — a time-sensitive, surgically correctable emergency 2. It guides whether urgent re-exploration is warranted (hematoma present) vs. conservative management (edema/neurapraxia) 3. It is non-invasive and rapidly available **Clinical Pearl (Bailey & Love / Scott-Brown):** Immediate surgical re-exploration is indicated if there is evidence of nerve transection witnessed intraoperatively OR if imaging reveals a compressive hematoma. Without imaging confirmation, blind re-exploration risks additional nerve injury. ## Why the Other Options Are Incorrect | Option | Reason Incorrect | |--------|-----------------| | A — Reassure + eye care only | Premature; does not rule out compressive hematoma requiring urgent decompression | | C — Immediate surgical re-exploration | Not indicated without imaging evidence of transection or compression; risks unnecessary morbidity | | D — EMG/NCS immediately | EMG/NCS is unreliable in the first 72 hours (Wallerian degeneration not yet complete); standard timing is Day 3–5 post-injury | ## Management Algorithm ``` Complete facial paralysis post-parotidectomy (within 24 hrs) ↓ Urgent MRI parotid region ↓ Hematoma/compression? → YES → Surgical decompression ↓ NO Edema/neurapraxia suspected → Eye care + conservative management ↓ Day 3–5: EMG/NCS to assess degree of nerve injury ↓ Guide further management (conservative vs. delayed exploration) ``` **Reference:** Bailey & Love's Short Practice of Surgery (27th ed.); Scott-Brown's Otorhinolaryngology — imaging is the critical first step to differentiate compressive from non-compressive causes of immediate post-parotidectomy facial palsy. 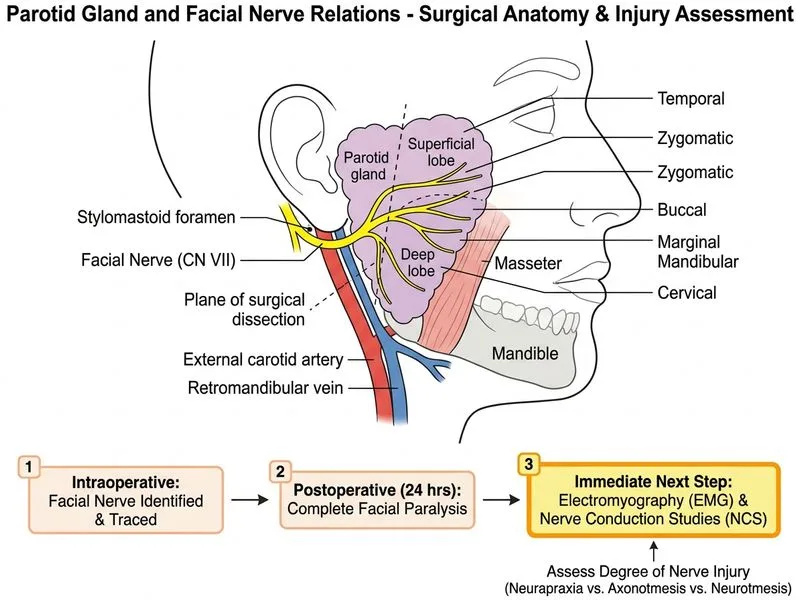
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.