## Clinical Scenario Analysis This child presents with **hypovolemic shock** secondary to acute gastroenteritis with severe dehydration. The clinical signs of shock are present: - Altered mental status (lethargy) - Poor perfusion (cold extremities, weak pulses, prolonged CRT of 4 seconds) - Hypotension (70/40 mmHg) ## Pediatric Shock Management Algorithm ```mermaid flowchart TD A[Suspected Pediatric Shock]:::outcome --> B{Assess perfusion & BP}:::decision B -->|Compensated shock| C[IV fluid bolus 20 mL/kg<br/>over 15-30 min]:::action B -->|Decompensated shock| D[Immediate IV access<br/>+ fluid bolus]:::action C --> E{Response to bolus?}:::decision D --> E E -->|Good response| F[Continue maintenance<br/>+ deficit replacement]:::action E -->|Poor response| G[Second bolus 20 mL/kg<br/>+ inotropes]:::action G --> H[Inotrope choice based<br/>on shock type]:::action H --> I[ICU monitoring]:::action ``` ## Key Point: First-Line Fluid Resuscitation **Pediatric Shock Protocol (PALS/APLS guideline):** - **First-line agent:** 0.9% Normal Saline or Ringer's Lactate - **Bolus volume:** 20 mL/kg IV over 15–30 minutes - **Route:** Peripheral IV (or intraosseous if IV access fails) - **Reassess after 15 minutes:** If no improvement, repeat bolus ± add inotropes **High-Yield:** In pediatric hypovolemic shock, the priority is **rapid restoration of circulating volume** before considering inotropes. Two boluses of crystalloid (up to 40 mL/kg) are standard before escalating to vasopressors. ## Rationale for This Case This child has: 1. **Clear hypovolemic etiology** (diarrhea + vomiting) 2. **Signs of decompensated shock** (hypotension + altered mental status) 3. **No contraindication to IV fluids** (no pulmonary edema, no hyperchloremic acidosis risk at this stage) **Clinical Pearl:** Even in decompensated shock, the first intervention in pediatric patients is **aggressive fluid resuscitation**, not immediate inotropes. Dopamine is reserved for refractory shock after 2 fluid boluses. ## Why NOT the Other Options? | Option | Why Wrong | |--------|----------| | 3% hypertonic saline | Reserved for **hyponatremic dehydration** (serum Na <130 mEq/L) or **cerebral edema**; not first-line for hypovolemic shock. Standard isotonic crystalloid is preferred. | | Dopamine at 5 mcg/kg/min | Inotropes are **second-line** after 2 boluses of crystalloid fail. Starting dopamine without adequate fluid resuscitation is ineffective and delays definitive treatment. | | Diagnostic peritoneal lavage | No clinical indication for abdominal bleeding; presentation is consistent with **gastroenteritis**, not trauma or intra-abdominal hemorrhage. | ## Citation [cite:Pediatric Advanced Life Support (PALS) 2020 Guidelines], [cite:Harrison 21e Ch 297] 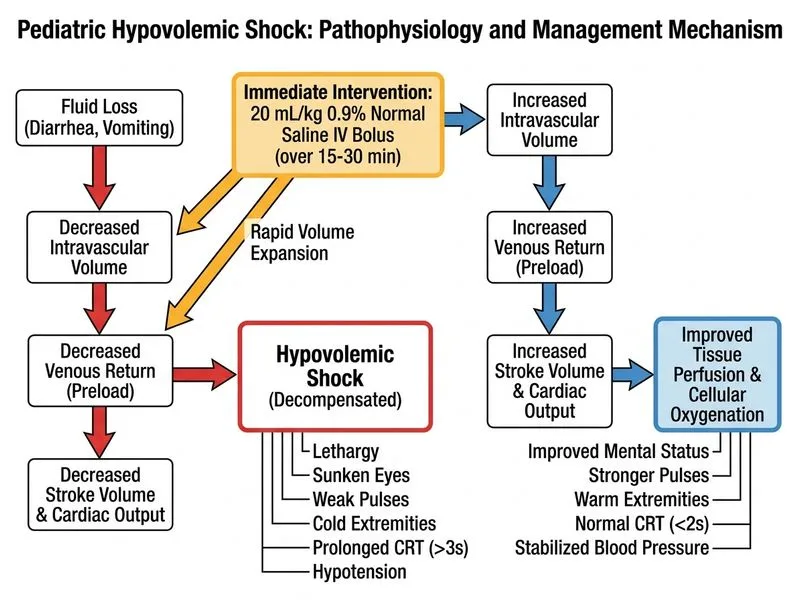
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.