## Clinical Scenario Analysis This child presents with **septic shock** secondary to influenza A with pneumonia and respiratory distress. Evidence of shock: - Tachycardia (140/min) - Hypotension (85/50 mmHg) - Prolonged capillary refill time (3 seconds) - Altered perfusion (irritability) - Hypoxemia (SpO₂ 88%) - Pulmonary involvement (bilateral crackles, retractions) ## Pediatric Septic Shock Management Sequence ```mermaid flowchart TD A[Septic Shock Suspected]:::outcome --> B[Immediate ABCs]:::action B --> C[High-flow O₂<br/>target SpO₂ ≥94%]:::action C --> D[Establish IV/IO access]:::action D --> E[Fluid bolus 20 mL/kg<br/>0.9% saline over 15-30 min]:::action E --> F{Reassess perfusion<br/>after bolus}:::decision F -->|Improved| G[Continue supportive care<br/>+ antibiotics/antivirals]:::action F -->|No improvement| H[Second bolus ±<br/>inotropes]:::action H --> I[ICU admission<br/>+ advanced support]:::action ``` ## Key Point: PALS Septic Shock Protocol **First 15 minutes (Golden Hour) priorities:** 1. **Oxygenation:** High-flow O₂ to maintain SpO₂ ≥94% 2. **Vascular access:** Peripheral IV or intraosseous line 3. **Fluid resuscitation:** 20 mL/kg bolus of 0.9% saline IV over 15–30 minutes 4. **Reassess:** Check perfusion, repeat bolus if needed 5. **Antimicrobials:** Broad-spectrum antibiotics (after cultures if possible) 6. **Antivirals:** Oseltamivir for confirmed influenza **High-Yield:** Fluid resuscitation is the **cornerstone** of septic shock management in children. Do NOT delay fluids for investigations or advanced interventions. ## Clinical Pearl: Respiratory Distress vs. Respiratory Failure - **Respiratory distress** (this case): Tachypnea, retractions, but maintaining SpO₂ and airway. Manage with O₂ and fluids. - **Respiratory failure:** Inability to maintain airway, SpO₂ <90% despite O₂, altered mental status. Requires intubation. This child has **distress, not failure** — high-flow O₂ and fluid bolus are appropriate before considering intubation. ## Why NOT the Other Options? | Option | Why Wrong | |--------|----------| | Mechanical ventilation immediately | **Premature escalation.** Child is maintaining airway and has respiratory distress, not failure. Intubation increases infection risk and should be reserved for airway compromise or refractory hypoxemia. | | Albuterol + oseltamivir, reassess in 2 hours | **Dangerous delay.** Child is in shock with hypotension and poor perfusion. Waiting 2 hours without fluid resuscitation risks cardiovascular collapse and multi-organ failure. | | Urgent intubation + surfactant | **Incorrect diagnosis.** This is **viral pneumonia with septic shock**, not ARDS or neonatal respiratory distress syndrome. Surfactant has no role; fluid resuscitation and oxygenation are priorities. | ## Mnemonic: SIRS Criteria (Systemic Inflammatory Response) **SIRS = Sepsis Inflammatory Response Syndrome** - **S** — Sepsis (infection + SIRS) - **I** — Infection source (influenza pneumonia) - **R** — Response (fever, tachycardia, tachypnea) - **S** — Shock (hypotension, poor perfusion) This child meets criteria for **septic shock** and requires immediate fluid resuscitation per PALS guidelines. ## Citation [cite:PALS 2020 Guidelines], [cite:Surviving Sepsis Campaign Pediatric Guidelines 2020] 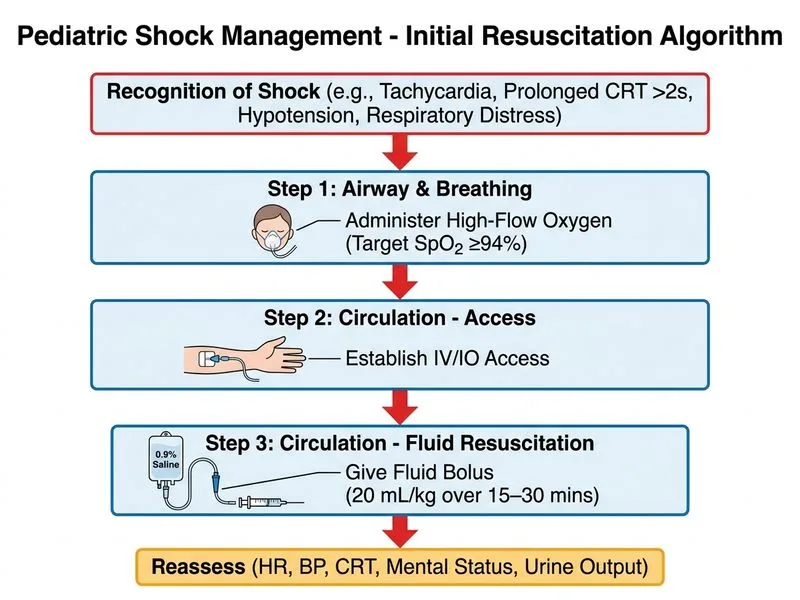
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.