## Compensatory Mechanisms in Pediatric Shock **Key Point:** The sympathetic nervous system is the FIRST and most rapid compensatory mechanism in shock, occurring within seconds. ### Timeline of Compensation | Mechanism | Onset | Duration | Effectiveness | |-----------|-------|----------|----------------| | Sympathetic activation (↑HR, ↑contractility, vasoconstriction) | Seconds | Minutes | Very rapid but unsustainable | | Fluid shift (Starling forces) | Minutes | Hours | Provides ~500 mL in children | | RAAS activation (aldosterone, ADH) | Minutes–hours | Hours–days | Longer-term compensation | | Increased renal perfusion | Hours | Days | Compensatory, not primary | **High-Yield:** In early compensatory shock, the child maintains normal blood pressure through increased heart rate and peripheral vasoconstriction. Blood pressure = Cardiac Output × Systemic Vascular Resistance. When CO drops, SVR ↑ to maintain BP. ### Mechanism 1. Baroreceptor sensing of ↓ blood pressure 2. Sympathetic discharge → catecholamine release (epinephrine, norepinephrine) 3. β~1~ receptors on heart → ↑ HR and contractility 4. α~1~ receptors on vessels → vasoconstriction (maintains central perfusion) 5. Skin becomes cool and mottled; capillary refill prolonged **Clinical Pearl:** A tachycardic child with cool extremities and normal blood pressure is in *compensated shock* — the sympathetic system is working. Once tachycardia fails to maintain BP, decompensated shock ensues. **Warning:** Do not confuse the FIRST mechanism (sympathetic) with the MOST IMPORTANT long-term mechanism (RAAS). NEET PG often tests this distinction. 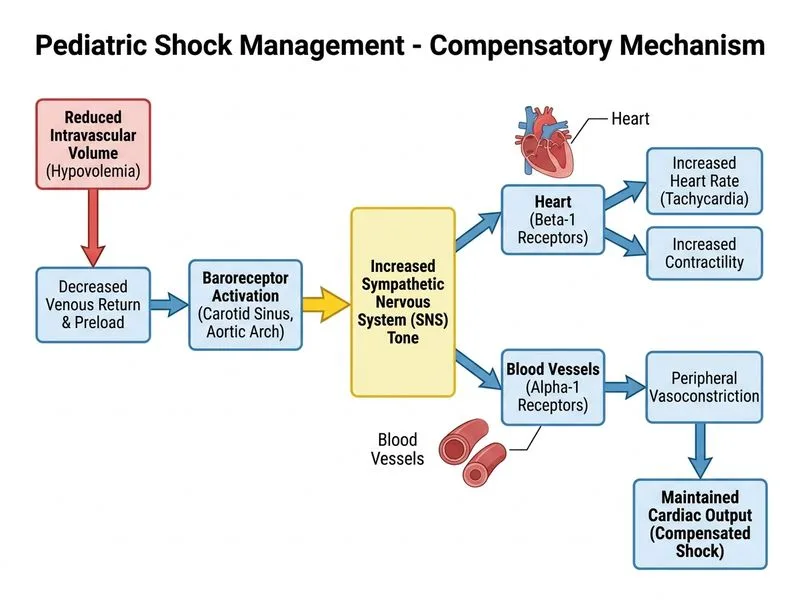
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.