## Clinical Assessment This child presents with **septic shock** (fever, hypotension, altered perfusion with cool extremities, delayed capillary refill, tachycardia, tachypnea) secondary to influenza A pneumonia with concurrent pulmonary edema (bilateral crackles, hypoxia). ## Shock Management Hierarchy in Pediatrics **Key Point:** The first-line intervention in pediatric septic shock is **rapid fluid resuscitation** with isotonic crystalloid (normal saline or Ringer's lactate), regardless of the presence of pulmonary findings. The 2020 Surviving Sepsis Campaign guidelines and pediatric PALS protocols mandate initial fluid bolus therapy before vasopressor consideration. **High-Yield:** In pediatric septic shock, give **20 mL/kg IV bolus of isotonic crystalloid over 10–15 minutes**. Reassess and repeat if needed (up to 60 mL/kg in the first hour). Vasopressors (dopamine, epinephrine) are second-line, reserved for refractory hypotension after adequate fluid resuscitation and antibiotics. ## Why Fluid First, Not Vasopressors? 1. **Hypovolemia** is the dominant mechanism in early septic shock; fluid restores preload and cardiac output. 2. **Dopamine at 5 mcg/kg/min** is inotropic but does not address the underlying fluid deficit and may worsen tissue perfusion if given before volume repletion. 3. **Pulmonary edema concern:** Although bilateral crackles are present, they are secondary to sepsis-induced capillary leak and hypoxia-driven pulmonary injury, NOT cardiogenic pulmonary edema. Fluid resuscitation improves systemic perfusion and oxygenation; overzealous fluid restriction worsens shock. ## Concurrent Management ```mermaid flowchart TD A[Pediatric Septic Shock]:::outcome --> B[Airway, Oxygen, Circulation]:::action B --> C[IV Fluid Bolus 20 mL/kg]:::action C --> D[Antibiotics within 1 hour]:::action D --> E{Reassess perfusion}:::decision E -->|Improved| F[Continue supportive care]:::action E -->|Persistent hypotension| G[Vasopressor + ICU]:::urgent B --> H[Antiviral oseltamivir]:::action ``` **Clinical Pearl:** The presence of pulmonary crackles does NOT contraindicate fluid bolus in shock; it reflects sepsis-induced capillary permeability, not fluid overload. Adequate resuscitation improves microcirculatory flow and tissue oxygenation. **Mnemonic:** **ABCDE of Pediatric Septic Shock** — **A**irway, **B**reathing (oxygen), **C**irculation (fluid first), **D**rugs (antibiotics, antivirals), **E**valuation (reassess every 15 min). [cite:Surviving Sepsis Campaign 2020, Pediatric Advanced Life Support Guidelines 2020] 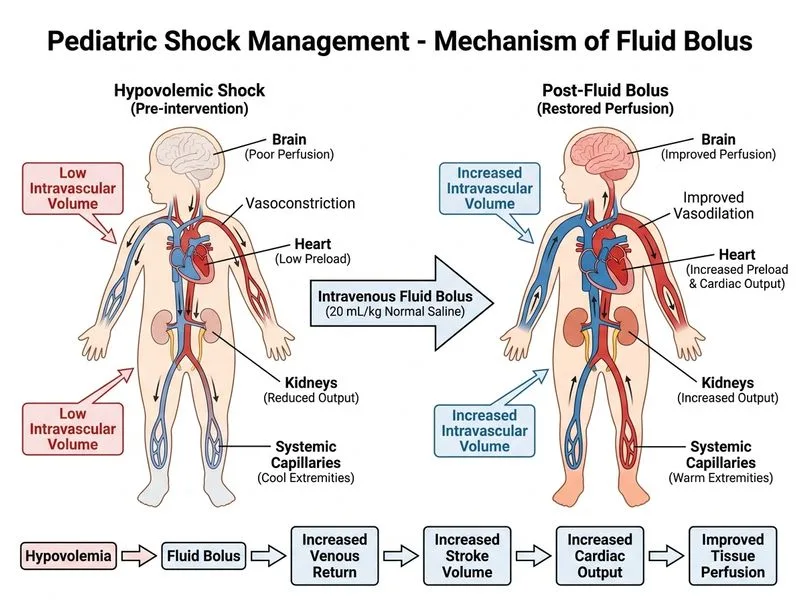
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.