## Clinical Assessment This child presents with **hypovolemic shock** secondary to acute gastroenteritis with severe dehydration: - **Signs of severe dehydration:** sunken eyes, loss of skin turgor, lethargy - **Shock indicators:** hypotension (65/40 mmHg), tachycardia (160/min), weak pulses, delayed capillary refill (3 sec) - **Oliguria:** no urine for 8 hours ## Fluid Resuscitation Protocol for Hypovolemic Shock **Key Point:** The gold standard for pediatric hypovolemic shock is **rapid isotonic crystalloid bolus: 20 mL/kg IV over 10–15 minutes**. Repeat once if perfusion does not improve, then reassess. Do NOT use hypotonic fluids or dextrose solutions for shock resuscitation. **High-Yield:** - **First-line fluid:** 0.9% normal saline or Ringer's lactate (isotonic, balanced) - **Bolus dose:** 20 mL/kg IV over 10–15 minutes - **Reassessment:** After each bolus, check for improvement in perfusion (capillary refill, pulse quality, mental status, blood pressure) - **Maximum initial bolus:** Up to 60 mL/kg in the first hour if shock persists ## Why Isotonic Crystalloid? ```mermaid flowchart TD A[Hypovolemic Shock]:::outcome --> B[Restore Intravascular Volume]:::action B --> C[Isotonic Crystalloid?]:::decision C -->|Yes: 0.9% NS or RL| D[Maintains osmotic balance]:::action C -->|No: Hypotonic or Dextrose| E[Worsens cellular edema]:::urgent D --> F[Improves cardiac preload]:::action D --> G[Restores perfusion pressure]:::action F --> H{Reassess in 15 min}:::decision H -->|Improved| I[Continue supportive care]:::action H -->|Persistent shock| J[Repeat bolus or vasopressor]:::urgent ``` **Clinical Pearl:** Hypotonic fluids (0.45% NaCl) cause water shift into intracellular space, worsening interstitial and cerebral edema. Dextrose solutions are metabolized rapidly, leaving only free water, which is inappropriate for shock resuscitation. Isotonic fluids expand intravascular volume without osmotic penalties. **Mnemonic:** **SHOCK Fluids** — **S**aline (0.9%), **H**artmann's (Ringer's lactate), **O**smotically **C**orrect, **K**eep isotonic. ## Reassessment After Bolus | Finding | Improved | Persistent | | --- | --- | --- | | Capillary refill | < 2 sec | ≥ 3 sec | | Pulse quality | Strong, regular | Weak, thready | | Mental status | Alert, interactive | Lethargic, confused | | Urine output | Present | Oliguria | | **Next step** | Continue supportive care | Repeat bolus or add vasopressor | [cite:Pediatric Advanced Life Support 2020, WHO Guidelines on Pediatric Shock Management] 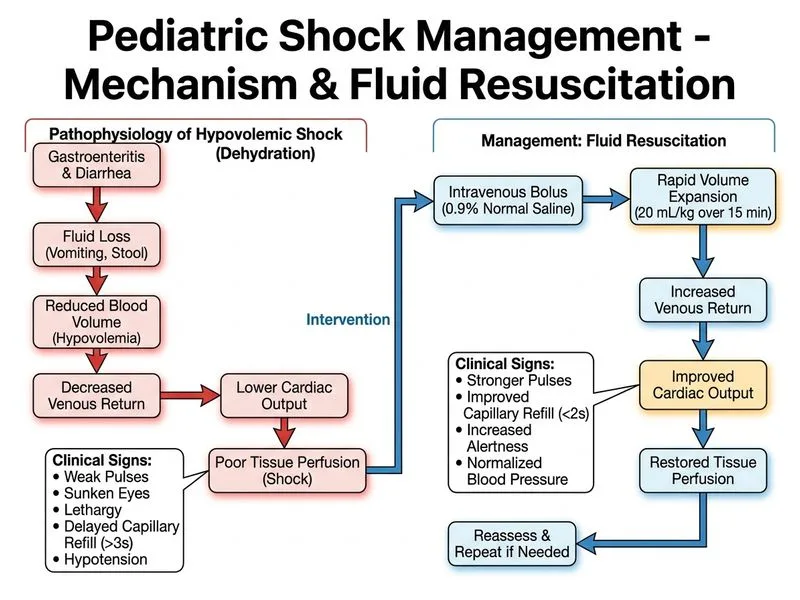
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.