## Clinical Assessment This child presents with **septic shock** (likely from severe pneumonia), evidenced by: - Fever + respiratory infection signs (cough, tachypnea, crackles) - Tachypnea (RR 52 = severe respiratory distress) - Hypoxemia (SpO₂ 88% on room air) - Signs of poor perfusion: cool extremities, prolonged CRT (2.5 sec), hypotension (95/60 is low for age 5) - Altered mental status (irritability) ## Septic Shock Management Hierarchy ```mermaid flowchart TD A[Suspected Septic Shock]:::outcome --> B[Oxygen to target SpO2 >90%]:::action B --> C[Establish IV/IO access]:::action C --> D[Fluid Bolus:<br/>20 mL/kg 0.9% NS<br/>over 15 minutes]:::action D --> E{Reassess perfusion}:::decision E -->|Improved| F[Continue resuscitation<br/>+ antibiotics<br/>+ source control]:::action E -->|No improvement| G[Repeat bolus<br/>+ inotropes/vasopressors]:::urgent G --> H{Respiratory failure?}:::decision H -->|Yes| I[Intubation & mechanical<br/>ventilation]:::action H -->|No| J[Continue medical<br/>management]:::action ``` ## Key Point: **Fluid resuscitation is the first pharmacological intervention in septic shock, even in the presence of respiratory distress.** The 2015 Surviving Sepsis Campaign guidelines mandate a **20 mL/kg bolus of crystalloid over 15 minutes** as the initial resuscitation step, *before* vasopressors or advanced airway management. ## High-Yield: - **Septic shock in children** often presents with respiratory infection as the source - Hypotension is a *late* sign in pediatric sepsis; earlier signs include tachycardia, prolonged CRT, cool extremities, and altered mental status - Do NOT delay fluid resuscitation to obtain imaging or escalate airway management - Oxygen + fluid bolus + antibiotics form the "golden hour" triad - Intubation is indicated for *respiratory failure* (inability to maintain airway/oxygenation), not merely for respiratory distress ## Clinical Pearl: This child's hypoxemia and respiratory distress may improve significantly with fluid resuscitation alone, as poor perfusion worsens tissue oxygenation. Once perfusion is restored and antibiotics are given, reassess before considering intubation. ## Warning: ~~Intubating a child in hypovolemic/septic shock without prior fluid resuscitation~~ — this risks cardiovascular collapse. Fluid first, then reassess. ~~Delaying fluid bolus to obtain a chest X-ray~~ — imaging is secondary to resuscitation in shock. 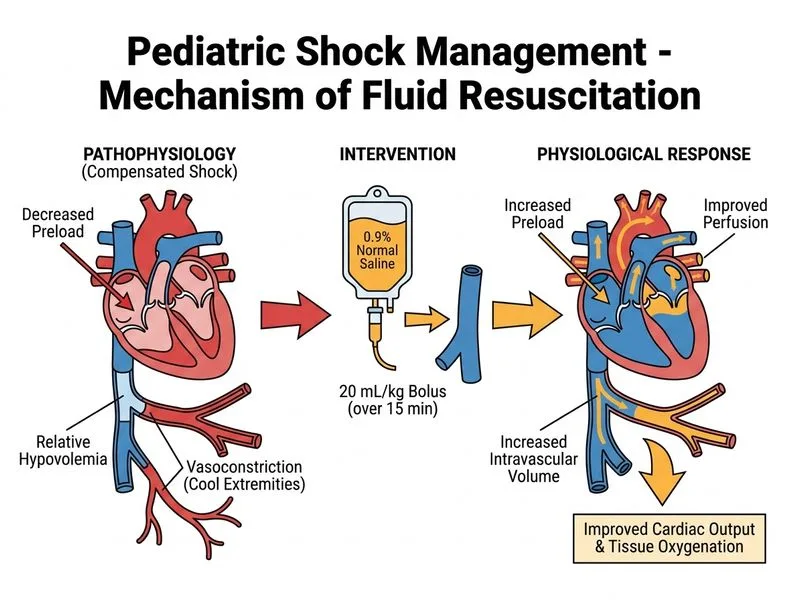
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.