## Distinguishing Septic Shock from Hypovolemic Shock ### Key Pathophysiologic Difference **Key Point:** Septic shock is characterized by **vasodilation and maldistribution of blood flow**, whereas hypovolemic shock results from **absolute loss of intravascular volume**. ### Clinical Feature Comparison | Feature | Septic Shock | Hypovolemic Shock | |---------|--------------|-------------------| | **Peripheral perfusion** | Warm, well-perfused (early/warm shock) | Cold, clammy, mottled | | **Pulse character** | Bounding, collapsing | Weak, thready | | **Pulse pressure** | Widened (due to vasodilation) | Narrowed | | **Blood pressure** | May be maintained initially | Reduced early | | **Skin turgor** | Normal | Decreased | | **Capillary refill** | Normal (< 2 sec) | Prolonged (> 2 sec) | | **Urine output** | Variable, may be maintained | Oliguria | ### Why Warm Peripheries Distinguish Septic Shock **High-Yield:** In septic shock, **peripheral vasodilation** from inflammatory mediators (TNF-α, IL-1, nitric oxide) causes **warm, well-perfused extremities** despite systemic hypotension. This is the hallmark of **distributive shock**. In contrast, hypovolemic shock triggers **sympathetic vasoconstriction** to maintain central perfusion, resulting in **cold, clammy peripheries**. **Clinical Pearl:** The presence of warm peripheries in a shocked child should immediately raise suspicion for sepsis, anaphylaxis, or other distributive causes — NOT hypovolemia. ### Why Other Features Are Non-Discriminatory Both septic and hypovolemic shock can present with: - Elevated lactate (tissue hypoperfusion in both) - Tachycardia (compensatory in both) - Metabolic acidosis (anaerobic metabolism in both) These features indicate shock severity but do NOT distinguish the **type** of shock. [cite:Nelson Textbook of Pediatrics 21e Ch 180] 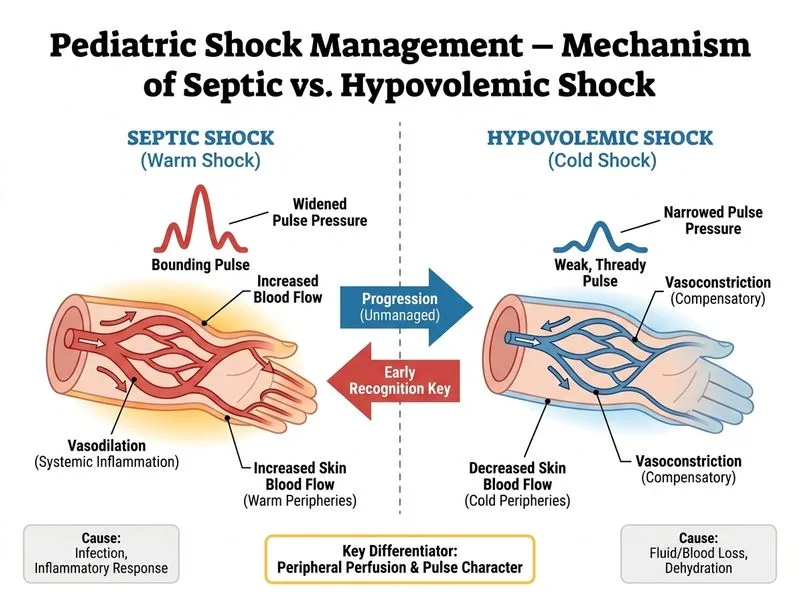
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.