## Septic Shock Recognition and Resuscitation **Key Point:** This child has meningococcal sepsis with septic shock (fever + petechial rash + hypotension + altered mental status + signs of poor perfusion + thrombocytopenia + elevated lactate). Time-sensitive intervention is critical. ### Septic Shock Diagnostic Criteria in This Child | Feature | Finding | Significance | |---------|---------|---------------| | **Fever** | 40.5°C | Systemic infection | | **Rash** | Petechial (non-blanching) | Meningococcemia (Neisseria meningitidis) | | **Hypotension** | 85/50 (< 5th percentile) | Distributive shock | | **Tachycardia** | 160/min | Compensatory response | | **Altered mental status** | Confusion, restlessness | CNS involvement ± hypoperfusion | | **CRT** | 4 seconds (> 2 sec) | Peripheral hypoperfusion | | **Mottled skin** | Cool periphery | Vasoconstriction, poor perfusion | | **Thrombocytopenia** | 45,000/μL | DIC (disseminated intravascular coagulation) | | **Elevated lactate** | 4.2 mmol/L | Tissue hypoxia/anaerobic metabolism | ### Pediatric Septic Shock Management Algorithm ```mermaid flowchart TD A[Suspected Sepsis + Shock]:::outcome --> B["Recognize: fever + hypotension<br/>+ poor perfusion + altered mental status"]:::action B --> C["Immediate actions<br/>parallel processing"]:::action C --> D["1. Establish IV/IO access<br/>2. Draw blood cultures<br/>3. Fluid bolus 20 mL/kg<br/>0.9% NS over 15 min"]:::action D --> E["4. START antibiotics<br/>WITHOUT waiting for cultures"]:::urgent E --> F["Ceftriaxone 80 mg/kg/day<br/>+ Vancomycin 15 mg/kg/dose"]:::action F --> G{Reassess perfusion<br/>after 15 min}:::decision G -->|Improved| H[Continue resuscitation<br/>+ source control]:::action G -->|Persists| I[Repeat bolus<br/>+ start vasopressor<br/>dopamine or noradrenaline]:::action C --> J["Investigations<br/>in parallel"]:::action J --> K["Blood cultures,<br/>CBC, CMP, lactate,<br/>coagulation profile"]:::action K --> L["Consider LP if<br/>no contraindications<br/>after stabilization"]:::action ``` ### Why Antibiotics BEFORE Culture Results? **High-Yield:** In septic shock, every hour of delay in antibiotic administration increases mortality by ~7–10%. The "golden hour" principle mandates: 1. **Blood cultures are drawn simultaneously with IV access** — not instead of it. 2. **Antibiotics are started immediately** — do not wait for culture results (which take 24–48 hours). 3. **Empirical broad-spectrum coverage** is used pending culture identification and sensitivities. **Clinical Pearl:** The phrase "cultures before antibiotics" applies to stable patients with suspected infection. In septic shock with hypotension and altered mental status, this is a medical emergency — antibiotics are given within the first 15 minutes of recognition, in parallel with fluid resuscitation. ### Antibiotic Selection for Meningococcal Sepsis - **Ceftriaxone** 80 mg/kg/day (max 2 g/dose) — excellent CSF penetration, covers most gram-negatives and gram-positives - **Vancomycin** 15 mg/kg/dose Q6H — covers penicillin-resistant pneumococci and meningococci - Consider **acyclovir** if HSV encephalitis is in the differential (though less likely with petechial rash) ### Fluid Resuscitation in Septic Shock - **First bolus:** 20 mL/kg 0.9% NS or Ringer's lactate over 15 minutes - **Reassess:** If improved, continue maintenance + deficit replacement - **If persists:** Repeat bolus (up to 60 mL/kg in first hour) + vasopressor initiation **Mnemonic for septic shock management: "ABCDE-FLUIDS"** - **A**irway, **B**reathing, **C**irculation - **D**iagnosis (blood cultures, lactate, CBC) - **E**arly antibiotics (within 15 minutes) - **F**luid bolus (20 mL/kg) - **L**actate clearance (reassess) - **U**se vasopressors if needed - **I**notropes for cardiogenic component - **D**eficit + maintenance calculation - **S**upport organ function (renal, hepatic, coagulation) 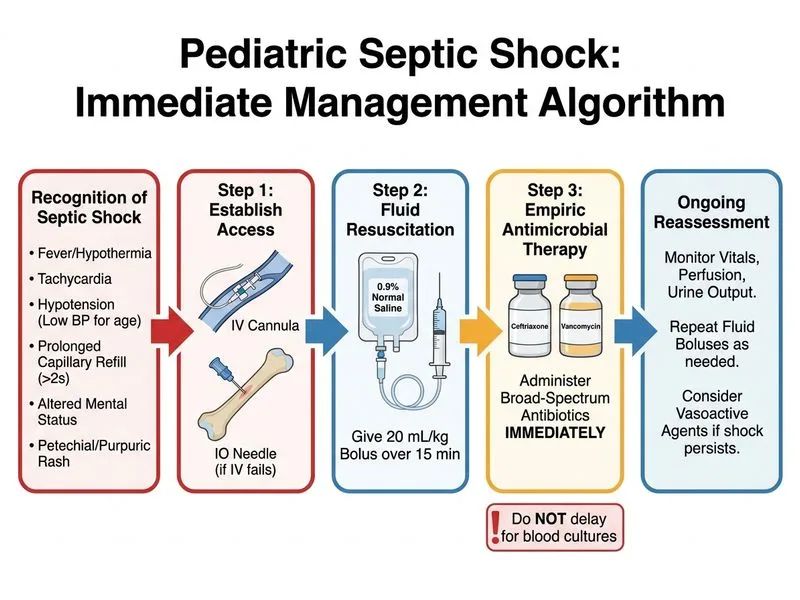
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.