## Clinical Context This 3-year-old presents with **septic shock** (fever, altered mental status, hypotension, prolonged capillary refill time of 3 seconds, cold extremities, and elevated WBC with left shift). The initial fluid bolus of 500 mL (~10 mL/kg for a ~50 kg child — but more precisely, for a typical 15 kg 3-year-old, 500 mL ≈ **33 mL/kg**, which exceeds the standard 20 mL/kg first bolus) has failed to restore perfusion, indicating **fluid-refractory septic shock**. > **Note on bolus volume:** A 3-year-old typically weighs ~14–16 kg. 500 mL ÷ 15 kg ≈ 33 mL/kg — this is actually more than one standard 20 mL/kg bolus. Regardless of exact weight, the clinical picture of **persistent shock after fluid resuscitation** defines fluid-refractory shock and mandates inotropic support. ## Shock Classification & Pathophysiology | Shock Type | Mechanism | Key Features | First-Line Therapy | |---|---|---|---| | **Hypovolemic** | ↓ Circulating volume | Dry mucosa, poor turgor, weak pulses | Fluid bolus (20 mL/kg) | | **Septic (cold)** | Vasodilation + capillary leak + myocardial depression | Fever, cold peripheries, weak pulses, elevated WBC | Fluid + antibiotics + **inotropes** | | **Cardiogenic** | ↓ Cardiac output | Hepatomegaly, JVD, pulmonary crackles | Inotropes, diuretics | | **Distributive (warm)** | Vasodilation | Warm skin, bounding pulses | Fluid + vasopressors | ## Why Option A is Correct: Inotropic Support After Fluid-Refractory Shock Per the **2020 Surviving Sepsis Campaign (SSC) Pediatric Guidelines** and **PALS (Pediatric Advanced Life Support)**: 1. **First bolus:** 20 mL/kg isotonic crystalloid over 15–30 minutes 2. **If shock persists → initiate vasoactive agents immediately** — do NOT continue repeated fluid boluses without inotropic support 3. **Empiric broad-spectrum antibiotics** should be given within 1 hour (concurrent with resuscitation) This child has received adequate (or more than adequate) initial fluid resuscitation with **minimal improvement** — the hallmark of **fluid-refractory shock**. Continuing fluids alone (Option B) risks: - Pulmonary edema - Worsening hyponatremia (Na⁺ 128 mEq/L, likely from SIADH secondary to sepsis) - Dilutional coagulopathy - Abdominal compartment syndrome **High-Yield:** Cold shock (cold extremities, weak pulses, prolonged CRT) in sepsis reflects **peripheral vasoconstriction and myocardial depression** — the correct intervention is **inotropes (adrenaline/dopamine)**, not more fluid. ## Why Other Options Are Wrong - **Option B (Continue NS boluses):** Incorrect. The child has already received ≥20 mL/kg with minimal improvement. Continuing fluids without inotropes in fluid-refractory shock delays definitive treatment and risks fluid overload. SSC 2020 explicitly recommends vasoactive agents after failed initial resuscitation. - **Option C (Hypertonic saline 3%):** Incorrect. Hypertonic saline is used for symptomatic hyponatremia with neurological compromise (seizures, coma), not for septic shock resuscitation. Na⁺ of 128 mEq/L here is likely SIADH from sepsis and does not require hypertonic saline. - **Option D (Antibiotics + observe):** Incorrect and dangerous. Septic shock requires active hemodynamic resuscitation. Observation alone in a child with hypotension and poor perfusion is inappropriate and potentially fatal. ## Inotrope Dosing Reference (PALS) - **Dopamine**: 5–10 mcg/kg/min (inotropic); 10–20 mcg/kg/min (vasopressor) - **Adrenaline (Epinephrine)**: 0.05–0.1 mcg/kg/min — **preferred in cold shock** with hypotension - **Noradrenaline**: 0.05–0.1 mcg/kg/min — preferred in warm shock (vasodilatory) **Clinical Pearl:** In pediatric cold septic shock, **adrenaline** is the preferred first-line vasoactive agent per SSC 2020, as it provides both inotropic and vasopressor effects. Dopamine is an acceptable alternative. **Key Point:** The MNEMONIC **FISH** for inotrope indications in pediatric septic shock: - **F**luid-refractory (failed adequate bolus) - **I**ncreasing lactate or worsening perfusion - **S**igns of shock persist - **H**ypotension despite fluids [cite: Surviving Sepsis Campaign 2020 Pediatric Guidelines; PALS Provider Manual 2020; Harrison's Principles of Internal Medicine 21e, Ch. 297] 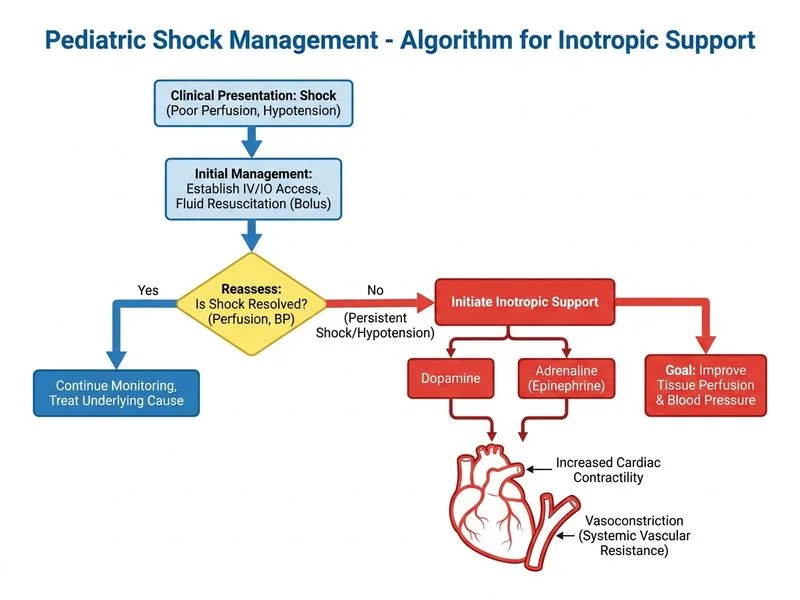
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.