## Clinical Diagnosis: Hypovolemic Shock from Severe Dehydration ### Shock Classification This child presents with **hypovolemic shock** secondary to severe dehydration from acute gastroenteritis. **Key Point:** The clinical triad of severe dehydration is: 1. **Sunken eyes** + **absent skin turgor** + **weak pulses** = ≥10% fluid loss 2. **Hypotension** (78/48 mmHg) + **prolonged capillary refill** (4 sec) = shock physiology 3. **Oliguria** (< 0.5 mL/kg/hr) = end-organ hypoperfusion ### Why NOT Septic Shock? | Feature | Septic Shock | This Case | Conclusion | |---|---|---|---| | **Fever** | Present | Absent (4-day diarrhea, no fever mentioned) | ✗ Not septic | | **WBC/Left shift** | Elevated | Not mentioned; unlikely | ✗ Not septic | | **Warm peripheries initially** | Yes | Cold extremities, weak pulses | ✗ Cold shock pattern is hypovolemic, not septic | | **Cause** | Infection | Fluid loss from GI tract | ✗ Hypovolemic | ### Acid-Base & Electrolyte Interpretation ```mermaid flowchart TD A[pH 7.18, HCO₃⁻ 12, PaCO₂ 28]:::outcome --> B{Identify primary disorder}:::decision B -->|pH low + HCO₃⁻ low| C[Metabolic Acidosis]:::outcome C --> D{PaCO₂ appropriate?}:::decision D -->|PaCO₂ 28 = appropriate respiratory compensation| E[Pure Metabolic Acidosis]:::outcome E --> F[Cause: Diarrheal loss of HCO₃⁻ + lactic acidosis from shock]:::action A --> G[Na⁺ 155 = Hypernatremia]:::outcome G --> H[Indicates: Hypotonic fluid loss > isotonic loss]:::action A --> I[K⁺ 6.2 = Hyperkalemia]:::outcome I --> J[Cause: Acidosis + acute kidney injury]:::action ``` **High-Yield:** In diarrheal dehydration: - **Metabolic acidosis** from bicarbonate loss in stool + lactic acidosis from hypovolemic shock - **Hypernatremia** (Na⁺ 155) indicates **hypotonic dehydration** (water loss > sodium loss) - **Hyperkalemia** (K⁺ 6.2) from acidosis (H⁺ shifts into cells; K⁺ shifts out) + acute kidney injury - **Elevated BUN:Cr ratio** (52:1.8 ≈ 29) indicates **prerenal azotemia** from shock ### Fluid Resuscitation Strategy **Key Point:** First-line fluid for hypovolemic shock is **0.9% normal saline (isotonic crystalloid)**. **Mnemonic: PALS Fluid Bolus = ISO** - **I**sotonic crystalloid (0.9% NS or Ringer's lactate) - **S**peed: 20 mL/kg over 15 min (or faster if severe shock) - **O**ver first bolus; reassess perfusion; repeat if needed **Why 0.9% NS (not 5% dextrose or 3% saline)?** | Fluid | Osmolality | Use Case | Why NOT here | |---|---|---|---| | **0.9% NS** | 308 mOsm/L (isotonic) | **Hypovolemic shock** | ✓ CORRECT | | **5% Dextrose** | 252 mOsm/L (hypotonic) | Maintenance; CNS edema | ✗ Hypotonic; worsens hypernatremia; no volume expansion | | **3% Saline** | 1026 mOsm/L (hypertonic) | Symptomatic hyponatremia (Na⁺ < 120) | ✗ Child has hypernatremia, not hyponatremia; hypertonic saline contraindicated | | **Ringer's Lactate** | 273 mOsm/L (isotonic) | Hypovolemic shock (alternative) | ✓ Also acceptable | **Clinical Pearl:** In hypernatremic dehydration, rapid saline correction risks **osmotic shrinkage of brain cells** → seizures. However, in **shock**, perfusion takes priority. Give isotonic saline bolus to restore perfusion first; then correct hypernatremia slowly (over 48 hr) with hypotonic fluids once shock is reversed. ### Post-Bolus Management 1. **Reassess perfusion** after 20 mL/kg bolus 2. **Repeat bolus** if shock persists (up to 60 mL/kg total in first hour) 3. **Maintenance + deficit replacement** with 0.9% NS or 0.45% NS (depending on hypernatremia severity) 4. **Monitor:** Urine output, electrolytes, acid-base status 5. **Treat hyperkalemia** (K⁺ 6.2) if ECG changes present: calcium gluconate, insulin + dextrose, sodium bicarbonate [cite:Park 26e Ch 10, PALS 2020 Guidelines] 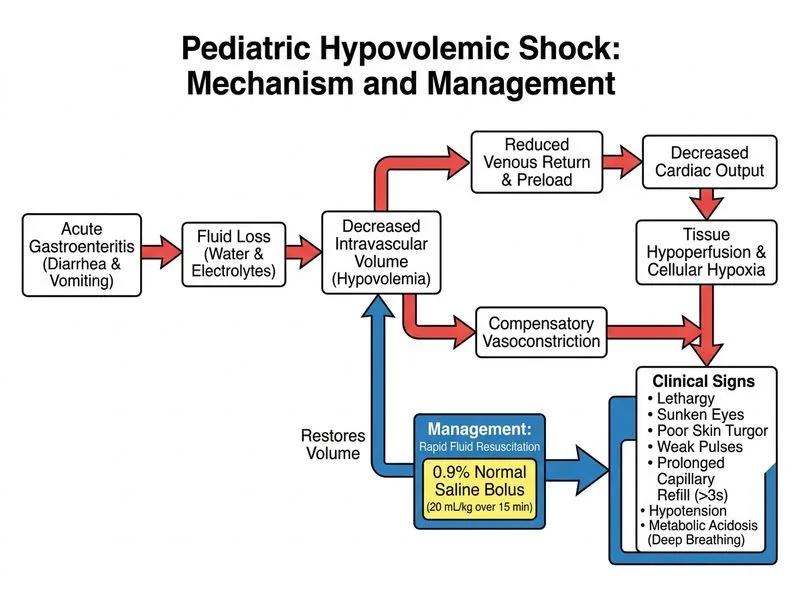
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.