## Clinical Diagnosis This child presents with **septic shock** secondary to acute gastroenteritis with severe dehydration. The constellation of fever, altered mental status, poor perfusion (cold extremities, prolonged capillary refill), hypotension, and elevated lactate confirms shock. ## Shock Classification | Feature | Septic Shock (this case) | Hypovolemic Shock | |---------|-------------------------|-------------------| | **Cause** | Infection + inflammatory cascade | Fluid loss alone | | **Lactate** | Elevated (tissue hypoxia + mitochondrial dysfunction) | Elevated (tissue hypoxia) | | **Extremities** | Cold (vasoconstriction initially) | Cold (vasoconstriction) | | **Urine output** | Oliguria (renal hypoperfusion) | Oliguria (prerenal) | ## Management Algorithm ```mermaid flowchart TD A[Child in shock<br/>Fever + poor perfusion]:::outcome --> B{Airway patent?}:::decision B -->|Yes| C[Establish IV access<br/>Draw labs]:::action B -->|No| D[Intubate]:::urgent C --> E[Bolus 20 mL/kg<br/>0.9% saline IV<br/>over 15 min]:::action E --> F[Reassess perfusion<br/>at 15 min]:::decision F -->|Improved| G[Continue maintenance<br/>+ deficit replacement]:::action F -->|Not improved| H[Second bolus 20 mL/kg<br/>+ prepare vasopressor]:::action H --> I[Start noradrenaline<br/>if hypotensive after<br/>40 mL/kg fluids]:::urgent G --> J[Antibiotics within 1 hour]:::action I --> J ``` **Key Point:** Pediatric septic shock management follows the **"Golden Hour"** protocol: rapid IV access, fluid resuscitation (20 mL/kg bolus of isotonic crystalloid), reassessment, and early antibiotics. Vasopressors are second-line if hypotension persists after 40 mL/kg fluid. **High-Yield:** The PALS/ACCM guidelines recommend **0.9% normal saline** (isotonic) for initial boluses in pediatric shock, NOT hypotonic solutions. Hypotonic fluids risk worsening hyponatremia (already present: Na+ 128) and cerebral edema. **Clinical Pearl:** Lactate >4 mmol/L indicates tissue hypoperfusion and is a marker of shock severity. This child's lactate of 5.2 confirms the need for urgent fluid resuscitation and likely vasopressor support. **Warning:** Do NOT restrict fluids or give diuretics in early septic shock — this worsens organ perfusion. Hyperkalemia (K+ 5.8) and acute kidney injury are *consequences* of shock, not reasons to withhold fluids. Treat hyperkalemia after perfusion is restored. ## Why Bolus Resuscitation? 1. Restores circulating volume and cardiac preload 2. Improves tissue perfusion and reduces lactate 3. Allows time to secure IV access and prepare vasopressors 4. Reassessment at 15 minutes guides escalation to vasopressor therapy [cite:Harrison 21e Ch 297; PALS 2020 Guidelines] 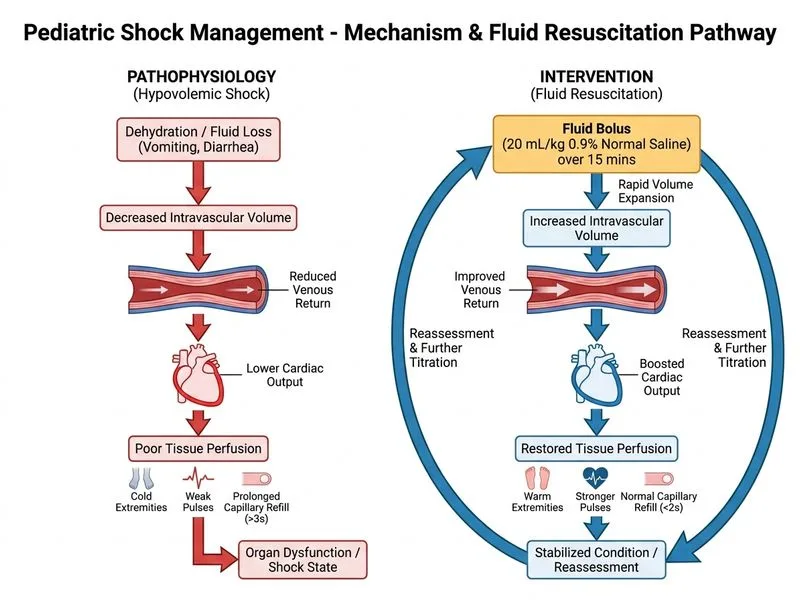
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.