## Clinical Diagnosis This child is in **Class II–III hemorrhagic shock** from blunt abdominal trauma with suspected solid organ injury (left flank bruising, abdominal distension, tenderness). She meets criteria for shock: tachycardia (140/min), tachypnea (32/min), borderline hypotension (95/60), prolonged capillary refill (3 sec), and a 2 g/dL drop in hemoglobin. ## Hemorrhagic Shock Classification in Children | Class | Blood Loss | HR | BP | Cap Refill | Urine Output | Mental Status | |-------|------------|----|----|------------|--------------|---------------| | **I** | <15% | Normal | Normal | <2 sec | Normal | Alert | | **II** | 15–30% | ↑↑ | Normal/↓ | 2–3 sec | ↓ | Anxious | | **III** | 30–40% | ↑↑↑ | ↓↓ | >3 sec | ↓↓ | Lethargic | | **IV** | >40% | ↑↑↑↑ | ↓↓↓ | Absent | Minimal | Unresponsive | **This child is Class II–III.** ## Trauma Resuscitation Algorithm ```mermaid flowchart TD A[Blunt abdominal trauma<br/>Signs of shock]:::outcome --> B[ABCs: Airway, Breathing]:::action B --> C{Breathing adequate?}:::decision C -->|Yes| D[Establish 2 large-bore IVs]:::action C -->|No| E[Supplemental O₂/<br/>Consider intubation]:::urgent D --> F[Start 20 mL/kg 0.9% saline<br/>bolus IV over 15 min]:::action F --> G[Reassess perfusion<br/>at 15 min]:::decision G -->|Improved| H[Continue maintenance<br/>+ deficit replacement]:::action G -->|Not improved| I[Prepare for second bolus<br/>+ blood products]:::action F --> J[Simultaneous: FAST exam<br/>or CT abdomen/pelvis]:::action J --> K{Free fluid/<br/>solid organ injury?}:::decision K -->|Yes, unstable| L[Surgical consultation<br/>Prepare OR]:::urgent K -->|Yes, stable| M[Admit ICU/HDU<br/>Serial exams]:::action K -->|No| N[Observe, serial labs]:::action ``` **Key Point:** The **"Permissive Hypotension"** concept applies to adults with penetrating trauma, NOT to children. Pediatric trauma resuscitation prioritizes **early, aggressive fluid boluses** to restore perfusion before irreversible shock develops. **High-Yield:** The **ATLS/PALS approach** for pediatric hemorrhagic shock: 1. **Two large-bore IVs** (18G or larger) 2. **First bolus: 20 mL/kg 0.9% saline** over 15 minutes 3. **Reassess at 15 minutes** 4. **Second bolus: 20 mL/kg** if still hypotensive 5. **Blood products (1:1:1 PRBC:FFP:platelets)** if no response to 40 mL/kg crystalloid 6. **Concurrent imaging (FAST or CT)** and surgical consultation **Clinical Pearl:** FAST (Focused Assessment with Sonography for Trauma) is rapid, bedside, and does not delay resuscitation. It detects free fluid in the peritoneum, pericardium, and pleura. CT is more sensitive but requires transport away from resuscitation. **Warning:** Do NOT delay fluid resuscitation while waiting for imaging or blood products. Do NOT perform DPL in the modern era — FAST and CT have replaced it. Do NOT transfuse without documented need (ongoing shock despite fluids). ## Why Not the Other Options? - **Immediate transfusion without fluids:** Crystalloid is first-line; blood is reserved for ongoing shock after 40 mL/kg fluids. - **Urinary catheter before fluids:** Urine output is a *marker* of perfusion, not a prerequisite for resuscitation. Delay in fluids worsens shock. - **DPL before fluids:** Outdated technique; FAST and CT are faster and non-invasive. [cite:ATLS 10th Edition; Harrison 21e Ch 297; Pediatric Trauma Handbook] 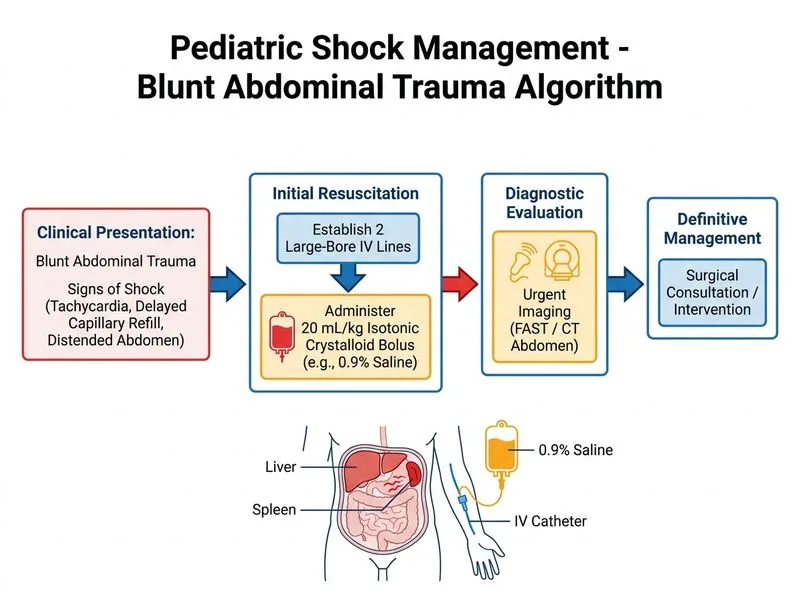
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.