## Clinical Assessment This 3-year-old child presents with **hypovolemic shock** secondary to severe dehydration from acute gastroenteritis. The clinical signs of shock are unmistakable: - Altered mental status (lethargy) - Weak pulses, cold extremities, prolonged capillary refill (>3 seconds) - Tachycardia and tachypnea - Hypotension (70/50 mmHg is critically low for a 3-year-old) - Metabolic acidosis (pH 7.28, HCO₃⁻ 12) consistent with tissue hypoperfusion ## Shock Classification & Pathophysiology This child is in **Class III–IV hypovolemic shock** (>25% circulating volume loss). The combination of severe dehydration, hypotension, and end-organ hypoperfusion (metabolic acidosis) mandates immediate fluid resuscitation. ## Management Algorithm ```mermaid flowchart TD A[Pediatric Shock Suspected]:::outcome --> B{Signs of hypoperfusion?}:::decision B -->|Yes: Cold extremities, weak pulses, altered mental status| C[Establish IV/IO access immediately]:::action C --> D[Bolus: 20 mL/kg crystalloid over 15 min]:::action D --> E{Reassess perfusion}:::decision E -->|Improved| F[Continue maintenance + deficit replacement]:::action E -->|Persistent shock| G[Repeat bolus up to 60 mL/kg total]:::action G --> H{Response?}:::decision H -->|No| I[Add inotropes + consider PICU]:::urgent H -->|Yes| F ``` ## Fluid Resuscitation Protocol (PALS/ACLS Guidelines) **Key Point:** The first-line therapy for hypovolemic shock in children is **rapid isotonic crystalloid bolus**, not slow rehydration. | Shock Class | Clinical Signs | Fluid Strategy | |---|---|---| | I–II (mild–moderate) | Tachycardia, normal BP, normal perfusion | Maintenance + deficit over 4–8 hours | | III–IV (severe) | Hypotension, weak pulses, altered mental status, acidosis | **20 mL/kg bolus over 15 min; repeat if needed** | **High-Yield:** In pediatric shock, the **first bolus of 20 mL/kg 0.9% NaCl or Ringer's lactate over 15 minutes** is standard. Reassess after each bolus. Up to 60 mL/kg total crystalloid can be given before considering inotropes. ## Why 0.9% Saline (Not Hypotonic)? **Clinical Pearl:** Although the child has hyponatremia (Na⁺ 128 mEq/L), the **acute hypovolemic shock takes priority**. Rapid isotonic saline restores circulating volume and perfusion. The hyponatremia is secondary to volume depletion and will correct as perfusion improves. Hypotonic fluids would worsen hyponatremia and delay shock reversal. ## Addressing Electrolyte Abnormalities - **Hyponatremia (128 mEq/L):** Likely dilutional; will improve with volume resuscitation. Do NOT use hypotonic fluids in shock. - **Hyperkalemia (5.8 mEq/L):** Secondary to acidosis and renal hypoperfusion. Will improve with restoration of perfusion and correction of acidosis. - **Metabolic acidosis:** Tissue hypoperfusion → lactate accumulation. Resolves with fluid resuscitation and improved oxygen delivery. **Mnemonic: SHOCK FIRST** — **S**aline bolus, **H**ypovolemia reversal, **O**xygen, **C**ontinuous monitoring, **K**eep reassessing, **F**luids before inotropes, **I**notropes only if refractory, **R**enal function, **S**odium correction (gradual), **T**ransfer to ICU if needed. ## Why Not Other Options? - **Slow IV rehydration:** Contraindicated in shock; delays restoration of perfusion and risks organ failure. - **Inotropes without fluid:** Futile in hypovolemic shock; the heart cannot generate adequate output without preload. - **Oral rehydration:** Inappropriate in shock; child is lethargic and at risk of aspiration. 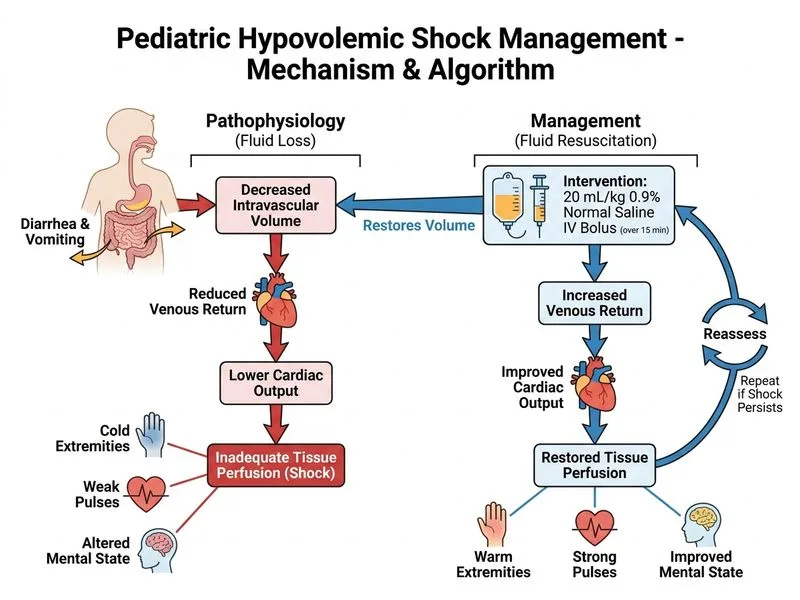
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.