## Diagnosis of Meningococcal Sepsis in Infants ### Clinical Presentation This infant presents with the classic triad of **meningococcemia with septic shock**: - **Fever + lethargy** (altered mental status) - **Petechial rash** (pathognomonic for meningococcal disease) - **Shock** (hypotension, tachycardia, prolonged capillary refill) ### Why Blood Culture Is the Investigation of Choice **Key Point:** Blood culture is the gold standard for confirming meningococcal sepsis because: 1. **Organism identification** — Neisseria meningitidis grows in aerobic blood cultures within 24–48 hours 2. **Antibiotic susceptibility testing** — determines resistance to penicillin, cephalosporins, or fluoroquinolones 3. **Timing** — can be obtained immediately without delaying antibiotics (cultures should be drawn BEFORE antibiotics, but treatment must not be delayed) 4. **High yield** — blood cultures are positive in 50–80% of meningococcal sepsis cases **High-Yield:** Gram stain of blood culture isolate shows **Gram-negative diplococci** (kidney-bean or coffee-bean shape), which is highly specific for Neisseria meningitidis. ### Diagnostic Algorithm for Suspected Meningococcal Sepsis ```mermaid flowchart TD A[Fever + petechial rash + shock]:::outcome --> B[Obtain blood cultures immediately]:::action B --> C[Start empiric antibiotics without delay]:::action C --> D{CSF accessible safely?}:::decision D -->|Yes, no contraindications| E[Lumbar puncture + CSF culture]:::action D -->|No, or contraindicated| F[Defer LP, rely on blood culture]:::action E --> G[Gram stain, culture, PCR of CSF]:::action F --> G B --> H[Gram stain of blood culture isolate]:::action H --> I{Gram-negative diplococci?}:::decision I -->|Yes| J[Presumptive N. meningitidis]:::outcome J --> K[Adjust antibiotics based on susceptibility]:::action ``` **Clinical Pearl:** In meningococcal sepsis with petechial rash, **do NOT delay antibiotics** while awaiting culture results. Blood cultures should be drawn first, but empiric ceftriaxone (or cefotaxime in infants) must be given immediately. Vancomycin is added if pneumococcal resistance is a concern. ### Why This Beats Other Options | Investigation | Role | Limitation | |---|---|---| | **Blood culture + Gram stain** | **Gold standard** — identifies organism, guides therapy | Takes 24–48 hrs; Gram stain available within hours | | CSF analysis via LP | Confirms meningitis, identifies organism | Contraindicated if shock/petechiae suggest meningococcemia; delays antibiotics; may worsen outcome | | Rapid PCR (blood) | Fast (results in 1–2 hrs) | Not widely available; does not provide susceptibility data | | Procalcitonin/CRP | Markers of inflammation | Non-specific; does not identify organism or guide antibiotic choice | **Mnemonic:** **BLOOD culture = B**est **L**aboratory **O**ption for **O**rganism **D** identification in sepsis. ### Why NOT Lumbar Puncture First? **Warning:** In a child with meningococcal sepsis and petechial rash: - Risk of **increased intracranial pressure** and herniation - Blood cultures are sufficient for diagnosis - CSF analysis is deferred until clinical stabilization (or omitted if blood culture is positive) - Empiric antibiotics are started based on clinical suspicion, not LP results **Key Point:** LP is indicated for suspected meningitis WITHOUT septic shock or petechiae; in meningococcemia, blood culture alone is diagnostic and safer. ### Antibiotic Regimen (Empiric) - **Ceftriaxone 80 mg/kg/day** (or cefotaxime) — covers meningococci and pneumococci - **Vancomycin 15 mg/kg Q6H** — added if pneumococcal resistance suspected - **Dexamethasone 0.15 mg/kg Q6H** — reduces mortality in bacterial meningitis **High-Yield:** Penicillin resistance in N. meningitidis is increasing globally; cephalosporins are now preferred over penicillin. 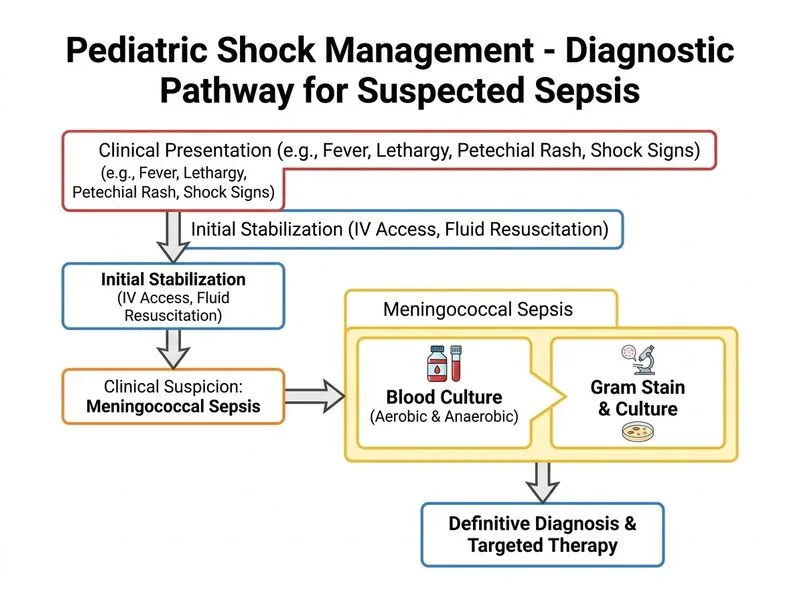
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.