## Diagnosis and Clinical Reasoning **Key Point:** Pelvic inflammatory disease (PID) is a clinical diagnosis based on empirical criteria; antibiotic therapy must begin immediately without waiting for culture confirmation, as delayed treatment increases risk of sequelae (infertility, ectopic pregnancy, chronic pelvic pain). ## Empirical Treatment Rationale This patient meets diagnostic criteria for acute PID: - Lower abdominal pain + pelvic tenderness (cervical motion tenderness, adnexal tenderness) - Fever ≥38.3°C - Purulent cervical discharge - Risk factors: multiple partners, no contraception **High-Yield:** The CDC and WHO guidelines mandate empirical broad-spectrum coverage because: 1. Gonorrhea and chlamydia are the most common causative organisms 2. Polymicrobial infection (including anaerobes) is frequent 3. Cultures have low sensitivity and results take 48–72 hours 4. Delayed treatment worsens prognosis ## Recommended Regimen **Outpatient (mild-moderate PID, no signs of sepsis):** - Ceftriaxone 250 mg IM single dose PLUS doxycycline 100 mg PO BD × 14 days ± metronidazole 400 mg PO BD × 14 days (if anaerobic coverage needed) **Inpatient (severe PID, fever >38.9°C, peritoneal signs, immunocompromised, failed outpatient therapy):** - Ceftriaxone 1–2 g IV 6-hourly PLUS doxycycline 100 mg IV/PO BD (or clindamycin 600 mg IV 6-hourly if doxycycline contraindicated) ± gentamicin This patient has fever, rebound tenderness, and bilateral adnexal involvement — consider inpatient IV therapy, but the principle is **empirical broad-spectrum coverage immediately**. ## Why Not Monotherapy? ~~Doxycycline monotherapy~~ is inadequate because it does not reliably cover gonorrhea (resistance increasing) or anaerobes, and misses polymicrobial infection in ~30% of cases. **Clinical Pearl:** Partner notification and treatment are essential; sexual partners within 60 days should receive empirical treatment for gonorrhea and chlamydia regardless of symptoms. 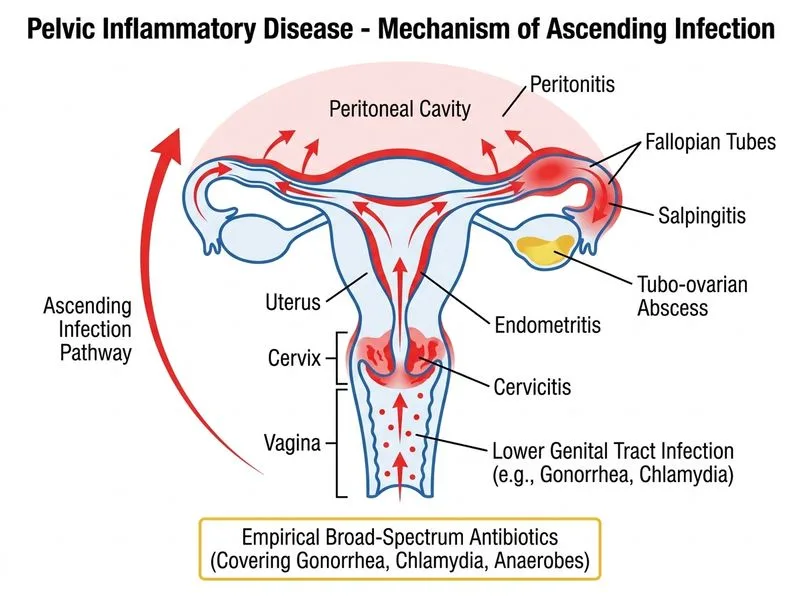
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.