## Clinical Context and Pathophysiology **Key Point:** Recurrent PID is the strongest risk factor for tubal factor infertility due to scarring, strictures, and peritubal adhesions that impair embryo transport. Even subclinical or mild inflammation causes permanent structural damage. ## Why Tubal Factor Infertility? This patient's presentation is **not acute PID** (afebrile, negative PCR, mild symptoms, no fever/peritoneal signs). Instead, she has **chronic sequelae** of recurrent PID: | Feature | Acute PID | Chronic Sequelae (This Patient) | |---------|-----------|----------------------------------| | Fever | Present (≥38.3°C) | Absent | | Cervical discharge | Purulent | Absent | | Culture/PCR | Positive | Negative | | Acute inflammation | Yes | No | | Tubal damage | Begins | Established (scarring, strictures) | **High-Yield:** Each episode of PID increases infertility risk: - 1 episode: 8% infertility risk - 2 episodes: 20% infertility risk - 3+ episodes: 40% infertility risk Mechanism: Endotoxin and inflammatory mediators (TNF-α, IL-1, IL-6) trigger fibroblast activation → collagen deposition → adhesions, strictures, and partial or complete tubal occlusion. ## Diagnostic Approach **Hysterosalpingography (HSG)** or **laparoscopy** would reveal: - Tubal strictures or partial occlusion - Peritubal adhesions - Distorted tubal anatomy **Clinical Pearl:** Mild or asymptomatic PID can still cause significant tubal damage; many women with tubal infertility have no history of symptomatic PID. ## Management - **Confirm diagnosis:** HSG or diagnostic laparoscopy - **Assisted reproduction:** IVF is the most effective treatment for tubal factor infertility (bypasses mechanical obstruction) - **Tubal surgery:** Considered only if minimal adhesions and patent tubes on imaging; success rates are low (10–30%) **Mnemonic: PID Sequelae — ASCI** - **A**dhesions (peritubal, intrauterine) - **S**trictures (tubal) - **C**hronic pelvic pain - **I**nfertility (tubal factor, ectopic pregnancy risk) 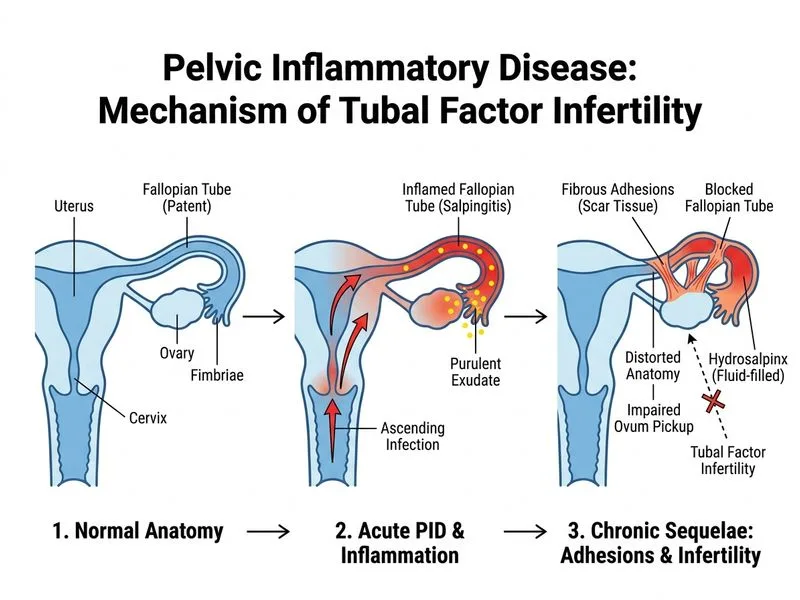
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.