## Clinical Diagnosis and Management Rationale **Key Point:** Pelvic inflammatory disease (PID) is a clinical diagnosis based on empirical criteria; culture confirmation is not required before starting treatment, and delayed antibiotics increase morbidity risk. ### Diagnostic Criteria for PID The CDC empirical criteria for PID diagnosis require: - Pelvic pain AND - One of: cervical motion tenderness, uterine tenderness, OR adnexal tenderness - No other cause identified This patient meets all criteria (pain + cervical motion tenderness + adnexal tenderness). ### Why Empirical Antibiotics Are Started Immediately **High-Yield:** PID is caused by multiple organisms (Neisseria gonorrhoeae, Chlamydia trachomatis, anaerobes, gram-negatives). Culture takes 48–72 hours; delayed treatment increases risk of: - Tubo-ovarian abscess (TOA) - Infertility (10–15% after first episode) - Ectopic pregnancy - Chronic pelvic pain ### Recommended Antibiotic Regimens (Outpatient) | Regimen | Agents | Notes | |---------|--------|-------| | **First-line** | Ceftriaxone 250 mg IM + Doxycycline 100 mg PO BD × 14 days ± Metronidazole 400 mg PO BD × 14 days | Covers gonorrhea, chlamydia, anaerobes | | **Allergy/Intolerance** | Fluoroquinolone (levofloxacin 500 mg daily) + Metronidazole | If β-lactam allergy | **Clinical Pearl:** Blood and cervical cultures should be obtained *before* antibiotics, but culture results should NOT delay treatment initiation. ### Why Other Options Are Incorrect - **Diagnostic laparoscopy** is reserved for cases where diagnosis is uncertain or TOA is suspected; it is not a first-line diagnostic tool. - **Deferring antibiotics pending cultures** risks progression to severe PID, TOA, or sepsis. - **Observation without antibiotics** is inappropriate; PID requires prompt antimicrobial therapy. **Mnemonic:** **PID = Prompt Identification & Drugs** — empirical antibiotics are the cornerstone of management. [cite:Harrison 21e Ch 137] 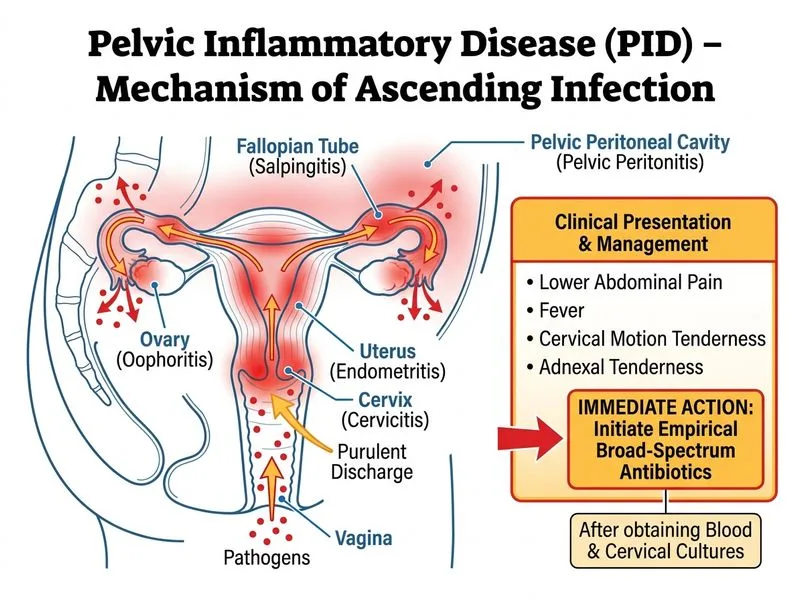
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.