## PID with Suspected Complications: IUD-Associated Tubo-Ovarian Abscess ### Clinical Red Flags in This Case **Key Point:** This patient has signs of complicated PID (possible tubo-ovarian abscess) requiring hospitalization and IV antibiotics, NOT outpatient oral therapy. Red flags present: - **Severe peritoneal signs:** Guarding (suggests peritonitis or localized abscess) - **Palpable adnexal mass:** Highly suggestive of tubo-ovarian abscess (TOA) - **Fever ≥39°C + elevated inflammatory markers:** CRP 8.5 mg/dL, WBC 14,500/μL - **IUD in situ:** Increases risk of anaerobic infection and abscess formation - **Hemoglobin 11.2 g/dL:** Mild anemia from chronic inflammation or blood loss ### Management Algorithm for Complicated PID ```mermaid flowchart TD A[PID with severe peritoneal signs<br/>or palpable adnexal mass]:::outcome --> B{IUD in situ?}:::decision B -->|Yes| C[Remove IUD immediately]:::action B -->|No| D[Proceed to IV antibiotics] C --> E[IV broad-spectrum antibiotics<br/>+ anaerobic coverage]:::action E --> F{Response at 48-72 hrs?}:::decision F -->|Yes| G[Continue IV antibiotics<br/>then switch to oral]:::action F -->|No| H[Imaging: Ultrasound/CT<br/>to assess for abscess]:::decision H -->|Abscess confirmed| I[Percutaneous drainage<br/>+ continued antibiotics]:::action H -->|No abscess| J[Laparoscopy for diagnosis]:::action I --> K[Clinical improvement]:::outcome J --> K ``` ### Why IUD Removal Is Mandatory **High-Yield:** The IUD acts as a foreign body and nidus for infection, particularly anaerobic bacteria. Removal is essential in: - Acute PID with fever and systemic toxicity - Suspected or confirmed tubo-ovarian abscess - Failure to respond to antibiotics within 48–72 hours Removal should occur **immediately upon diagnosis**, before or concurrent with antibiotic initiation. ### Recommended IV Antibiotic Regimen (Hospitalized PID with Abscess Risk) | Component | Agent | Dosing | |-----------|-------|--------| | **3rd-gen cephalosporin** | Ceftriaxone | 1–2 g IV Q12H | | **Tetracycline** | Doxycycline | 100 mg IV/PO BD | | **Anaerobic coverage** | Metronidazole | 500 mg IV Q8H | | **Alternative** | Clindamycin | 600–900 mg IV Q6–8H (covers anaerobes) | **Clinical Pearl:** Clindamycin + gentamicin is an alternative regimen and provides excellent anaerobic coverage, which is critical in IUD-associated PID. ### Why Imaging Before Antibiotics Is Wrong While ultrasound would confirm TOA, **do not delay IUD removal and IV antibiotics while awaiting imaging.** In a patient with severe peritoneal signs and a palpable mass, the clinical suspicion is high enough to warrant immediate intervention. Imaging can be obtained after stabilization if needed for drainage planning. **Tip:** Imaging (ultrasound or CT) is useful AFTER 48–72 hours of antibiotics if the patient does not improve, to guide percutaneous drainage. It is NOT a prerequisite for initiating treatment in acute, severe PID. 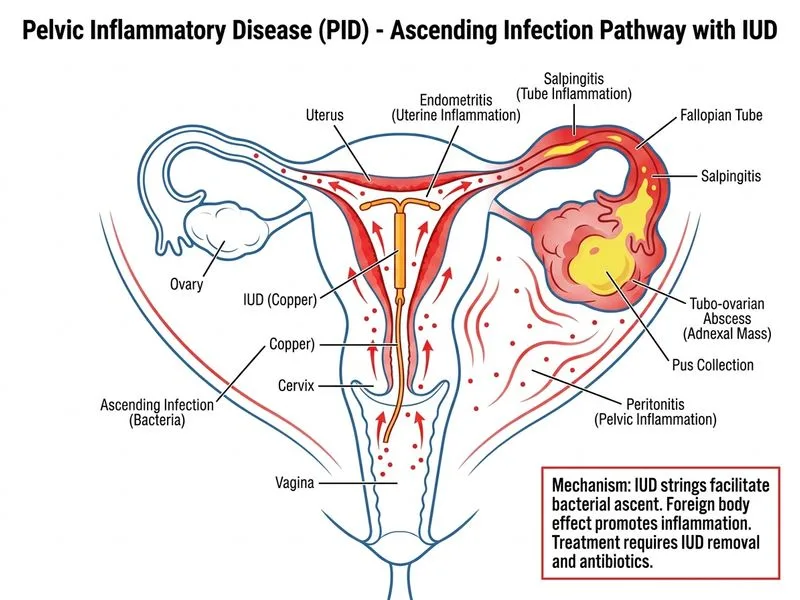
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.