## Pathophysiology of NSAID-Induced Peptic Ulcer Disease ### Mechanism of Ulcer Formation NSAIDs (non-selective cyclooxygenase inhibitors) impair the protective mechanisms of the gastric and duodenal mucosa by blocking prostaglandin (PG) synthesis. **Key Point:** Prostaglandins (particularly PGE~2~ and PGI~2~) are essential for: - Stimulating mucus secretion - Promoting bicarbonate secretion - Maintaining mucosal blood flow - Enhancing mucosal cell proliferation and repair ### Why NSAID-Induced Ulcers Occur 1. **Loss of cytoprotection** — reduced PG-mediated mucus and HCO~3~^−^ secretion 2. **Direct mucosal injury** — NSAIDs are acidic and cause direct epithelial damage 3. **Impaired healing** — reduced blood flow and cell proliferation 4. **Acid persistence** — acid secretion remains normal or elevated, unopposed by protective mechanisms ### Clinical Features in This Case - **Risk factor:** 2-year NSAID use (ibuprofen) - **Location:** Anterior duodenal wall (classic for NSAID ulcers; posterior wall is more common with H. pylori) - **Clean base:** Indicates chronic ulcer with healing response - **Iron deficiency anemia:** Chronic blood loss from ulcer **High-Yield:** NSAID-induced ulcers are the second most common cause of peptic ulcer disease (after H. pylori), accounting for ~25% of cases. They are more common in elderly patients and those on long-term therapy. **Clinical Pearl:** The anterior duodenal wall location is significant because perforation here leads to peritonitis; posterior wall ulcers erode into the gastroduodenal artery, causing hemorrhage. ### Differential Consideration - ~~H. pylori~~ — would present with antral/prepyloric ulcers; serology or CLO test would be positive - ~~Zollinger-Ellison~~ — would show multiple ulcers, severe diarrhea, and markedly elevated fasting gastrin (>1000 pg/mL) - ~~Vasculitis~~ — rare, would show systemic features and histological evidence of vessel inflammation 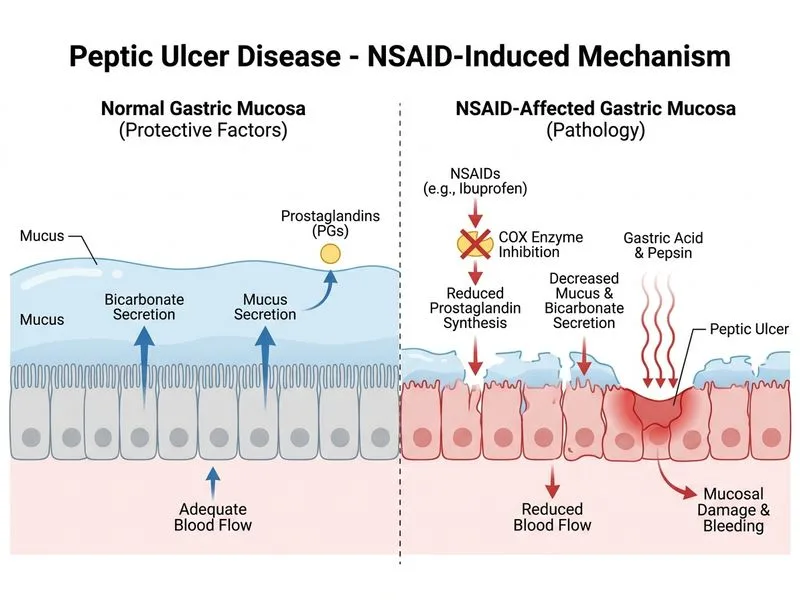
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.