## Management of Bleeding Peptic Ulcer After Endoscopic Hemostasis **Key Point:** After successful endoscopic hemostasis of a bleeding peptic ulcer, the patient requires admission for high-dose acid suppression and surveillance endoscopy to reduce rebleeding risk. ### Rationale for Correct Answer Following endoscopic treatment of a bleeding ulcer with a visible vessel: 1. **High-dose IV PPI therapy** — reduces gastric pH to < 6.0, which maintains clot stability and prevents rebleeding. Continuous infusion is superior to bolus dosing. 2. **Repeat endoscopy in 24 hours** — allows detection of early rebleeding and intervention before haemodynamic compromise. This is standard practice in high-risk ulcers (visible vessel, arterial spurting). 3. **Admission mandatory** — the patient has already bled significantly (melena) and has a high-risk stigma (visible vessel). Outpatient management is inappropriate. **High-Yield:** Rebleeding occurs in 10–30% of cases after initial hemostasis; repeat endoscopy within 24 hours reduces mortality and need for surgery. ### Why Other Options Are Incorrect | Option | Why Wrong | |--------|----------| | Discharge home with oral PPI | Oral agents achieve insufficient gastric pH in the immediate post-bleed period. Patient is at high risk for rebleeding and requires ICU-level monitoring. | | Immediate surgical intervention | Surgery is reserved for rebleeding after 2 failed endoscopic attempts, perforation, or haemodynamic instability despite resuscitation. First-line is medical + endoscopic management. | | High-dose oral H2-antagonist | H2-blockers are inferior to PPIs for acid suppression and cannot achieve target pH < 6.0. Oral route is inadequate in acute bleeding. | **Clinical Pearl:** The "visible vessel" is a predictor of rebleeding (Forrest Ib); these patients have ~50% rebleeding risk if untreated, but only ~10% after successful endoscopy + PPI. **Mnemonic: REBLEED** — Repeat endoscopy, Elevated PPI (IV), Bed rest, Liquid diet, Endoscopy surveillance, Exclude perforation, Discharge only after 48–72 hrs stable. 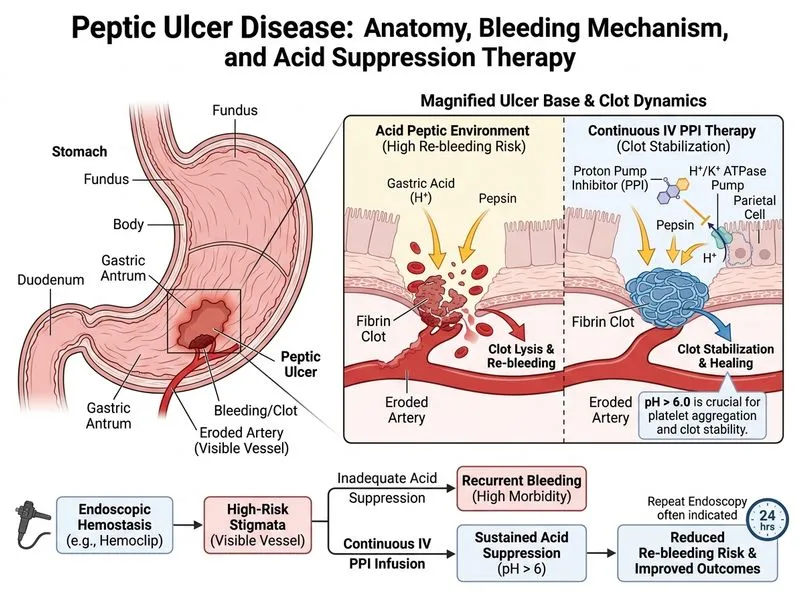
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.