## Pathogenesis of NSAID-Induced Peptic Ulcer Disease **Key Point:** NSAIDs cause peptic ulcers primarily by inhibiting COX-1 and COX-2, which reduces prostaglandin (PG) synthesis. Prostaglandins are essential for mucosal cytoprotection, and their depletion leads to ulcer formation. ### Mechanism of Mucosal Injury 1. **COX inhibition**: NSAIDs block both COX-1 and COX-2 enzymes. 2. **Prostaglandin depletion**: Reduced synthesis of PGE~2~ and PGI~2~. 3. **Loss of protective functions**: - Decreased mucus secretion - Reduced bicarbonate secretion - Impaired mucosal blood flow - Weakened epithelial cell tight junctions 4. **Net result**: Increased acid-induced mucosal damage and ulcer formation. ### Prostaglandin Functions in Mucosal Protection | Function | Effect | | --- | --- | | Mucus secretion | Creates protective barrier | | Bicarbonate secretion | Neutralizes acid at mucosal surface | | Blood flow | Maintains mucosal perfusion and healing | | Cell proliferation | Supports epithelial regeneration | | Tight junction integrity | Prevents back-diffusion of acid | **Clinical Pearl:** This is why COX-2 selective inhibitors (e.g., celecoxib) were developed — they spare COX-1 in the stomach, preserving prostaglandin-mediated cytoprotection. However, they still carry ulcer risk, albeit lower than non-selective NSAIDs. **High-Yield:** NSAID ulcers are typically **gastric** (especially antral) and **duodenal**, and are often **asymptomatic** until complications (bleeding, perforation) occur. This contrasts with H. pylori ulcers, which are usually symptomatic. **Mnemonic:** **"PG DOWN = Ulcer UP"** — Prostaglandins down → ulcer risk up. 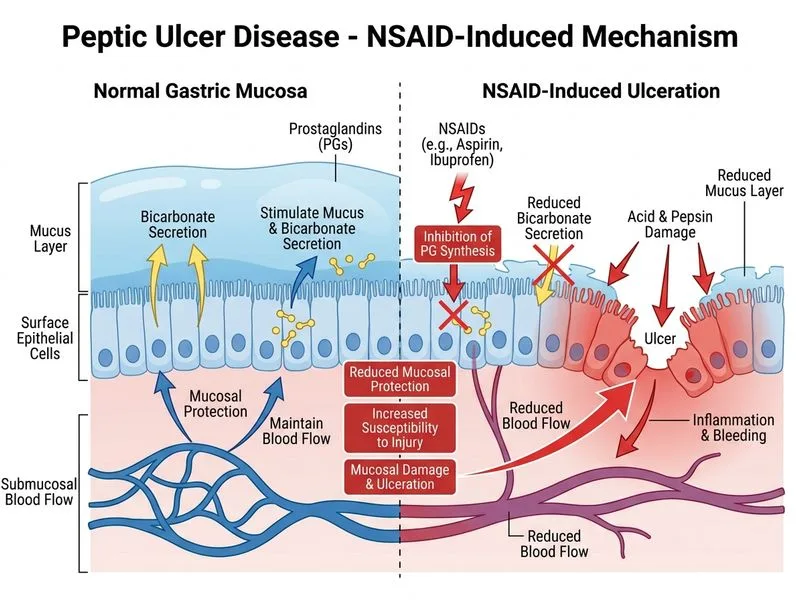
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.