## Clinical Scenario Analysis This patient has **NSAID-induced (aspirin) peptic ulcer with active bleeding (Forrest IIb)**. The key challenge is balancing hemostasis with the need to maintain antiplatelet therapy for secondary stroke prevention. ## Management Algorithm for Bleeding PUD in Antiplatelet Users ```mermaid flowchart TD A[Bleeding PUD on aspirin/NSAID]:::outcome --> B[Endoscopic hemostasis indicated]:::action B --> C{Continue antiplatelet?}:::decision C -->|High cardiovascular risk| D[Temporary cessation 5-7 days]:::action C -->|Low cardiovascular risk| E[Continue aspirin during procedure] D --> F[Restart aspirin + PPI after hemostasis]:::action E --> F F --> G[PPI 40 mg BD for 4-8 weeks]:::action G --> H[Assess for H. pylori/NSAID continuation]:::outcome ``` ## Key Point: **Endoscopic hemostasis is the standard of care for bleeding PUD**, regardless of antiplatelet therapy status [cite:Harrison 21e Ch 297]. The presence of active bleeding (Forrest IIb) mandates intervention. ## High-Yield: Forrest Classification | Grade | Appearance | Rebleeding Risk | Intervention | |-------|-----------|-----------------|---------------| | Ia | Spurting arterial bleeding | 90% | **Endoscopic** | | Ib | Oozing bleeding | 80% | **Endoscopic** | | IIa | Visible vessel (no bleeding) | 50% | **Endoscopic** | | IIb | Adherent clot | 30% | **Consider endoscopic** | | IIc | Flat pigmented spot | 10% | **Supportive care** | | III | Clean base | 5% | **Supportive care** | **This patient has Forrest IIb → endoscopic hemostasis indicated.** ## Management of Antiplatelet Therapy During Bleeding ### Temporary Cessation Strategy (Preferred for Secondary Prevention) 1. **Stop aspirin temporarily** (5–7 days) to allow hemostasis and ulcer stabilization. 2. **Perform endoscopic hemostasis** (injection of epinephrine + sclerotherapy, or thermal cautery). 3. **Start PPI 40 mg BD** immediately (high-dose for 4–8 weeks). 4. **Restart aspirin after 5–7 days** once bleeding has stopped and ulcer is stable, WITH gastroprotection (continue PPI). ### Rationale - Aspirin increases bleeding risk by 2–3 fold in PUD. - Temporary cessation (5–7 days) allows clot formation and hemostasis without significantly increasing thrombotic risk in secondary prevention (stroke risk is ~1–2% per week). - Restarting aspirin + PPI reduces rebleeding to <5%. ## Clinical Pearl: **H. pylori-negative, NSAID-induced ulcer**: This patient is H. pylori-negative, so the ulcer is aspirin-induced. Management focuses on: 1. Stopping the offending agent (aspirin temporarily). 2. Hemostasis (endoscopic). 3. PPI therapy (high-dose). 4. Restart with gastroprotection (PPI). ## Why This Approach? 1. **Endoscopic hemostasis is evidence-based**: Reduces rebleeding by 70% and mortality by 30% compared to medical management alone. 2. **Temporary aspirin cessation is safe**: 5–7 days of cessation does not significantly increase stroke risk in secondary prevention. 3. **PPI + aspirin restart reduces rebleeding**: Combination therapy reduces rebleeding to <5% vs. 20–30% with aspirin alone. 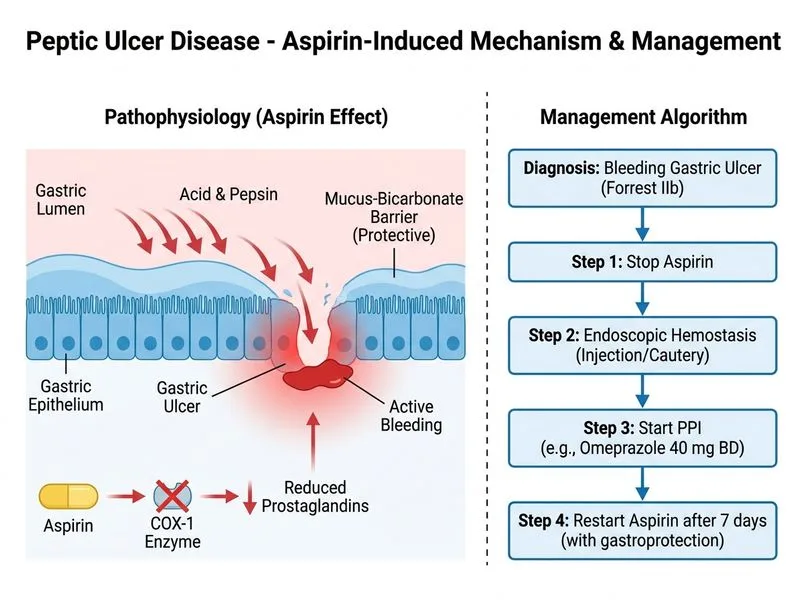
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.