## Imaging of Diverticular Perforation **Key Point:** CT abdomen and pelvis with **IV and oral contrast** is the gold-standard investigation for confirming diverticular perforation and assessing the extent of peritoneal contamination. It provides the highest sensitivity for identifying the perforation site, delineating bowel anatomy, detecting extraluminal air/fluid, and characterising abscess formation. ### Comparison of Imaging Modalities | Modality | Sensitivity for Perforation | Bowel Lumen Delineation | Shows Contamination | Peritonitis Assessment | |----------|---------------------------|------------------------|----------------------|------------------------| | **CT IV + oral contrast** | ~98% | **Excellent** | Excellent | Excellent | | **CT IV contrast alone** | 95–97% | Good | Excellent | Excellent | | **Erect X-ray** | 60–70% | No | No | No | | **MRI abdomen** | ~90% | Good | Good | Good | **High-Yield:** CT with IV and oral contrast demonstrates: 1. **Perforation site** — focal diverticular defect with extraluminal air or contrast leak 2. **Pneumoperitoneum** — free intraperitoneal air 3. **Peritoneal contamination** — extent of feculent material, free fluid, and abscess pockets 4. **Inflammation grade** — pericolic fat stranding, localised vs. generalised peritonitis (Hinchey classification) 5. **Adjacent organ involvement** — bladder, small bowel, pelvic structures ### Why IV + Oral Contrast is Preferred - **Oral contrast** (water-soluble agents such as Gastrografin) delineates the bowel lumen, helps identify the exact site of perforation, and can demonstrate contrast extravasation — all critical for surgical planning. **Barium** is contraindicated in suspected perforation (risk of barium peritonitis), but **water-soluble oral contrast is safe and widely used** per ACR guidelines and standard surgical practice. - **IV contrast** enhances bowel wall, mesentery, and inflammatory changes, enabling abscess characterisation and vascular assessment. - CT IV alone is a reasonable alternative when oral contrast administration is not feasible (e.g., vomiting, haemodynamic instability), but it is **not** the preferred first-line choice when the full study can be obtained. - **Erect X-ray** is useful as a rapid screen for pneumoperitoneum but cannot confirm the source or assess contamination extent. - **MRI** is limited by availability, prolonged scan time, and motion artefact in the acute setting. ### Why Option A (IV Contrast Alone) is Incorrect as the "Most Specific" While CT with IV contrast alone is highly sensitive (~95–97%) and widely used in emergency settings, it does **not** provide optimal bowel lumen delineation. The addition of water-soluble oral contrast improves identification of the exact perforation site and can demonstrate contrast extravasation, making CT with **both IV and oral contrast** the most specific modality for confirming diverticular perforation and assessing peritoneal contamination extent. **Clinical Pearl:** Per the **American College of Radiology (ACR) Appropriateness Criteria** for left lower quadrant pain/suspected diverticular perforation, CT abdomen/pelvis with IV contrast is "usually appropriate," and the addition of water-soluble oral contrast further improves diagnostic specificity — particularly for surgical planning and Hinchey classification. **Mnemonic: PAST (for perforation CT)** - **P** — Perforation site (diverticulum) - **A** — Abscess / free air - **S** — Stranding (pericolonic inflammation) - **T** — Tracking of contamination (Hinchey grade) *Reference: ACR Appropriateness Criteria — Left Lower Quadrant Pain; Schwartz's Principles of Surgery, 11th ed.; Emergency Radiology (Novelline), 6th ed.* 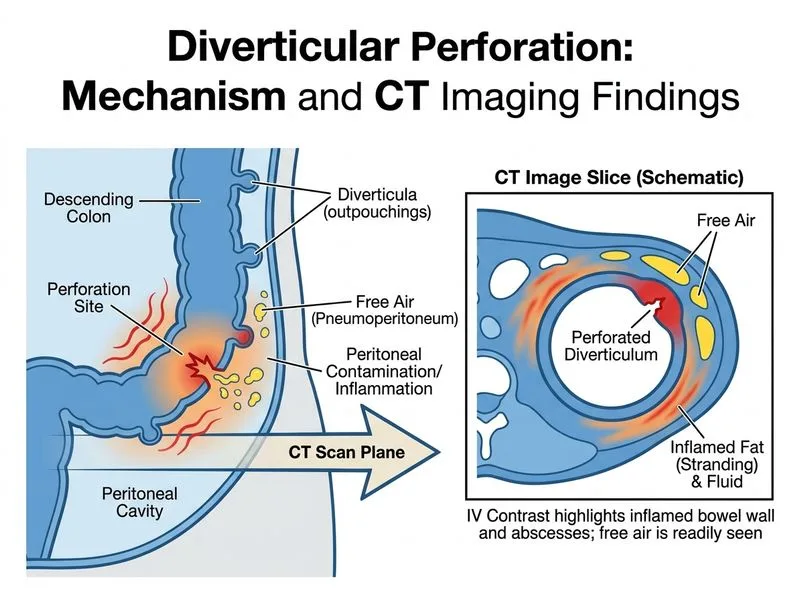
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.