## Clinical Scenario Analysis This patient presents with **acute perforation of a peptic ulcer** — evidenced by: - Acute onset severe epigastric pain - Abdominal rigidity (peritoneal signs) - Pneumoperitoneum on plain film - Hemodynamic compromise (hypotension, tachycardia) ## Management Algorithm for Perforated Peptic Ulcer ```mermaid flowchart TD A[Perforated peptic ulcer diagnosed]:::outcome --> B{Hemodynamically stable?}:::decision B -->|No/Unstable| C[Resuscitate: IV fluids, O2]:::action B -->|Yes| D[Proceed to definitive management]:::action C --> E[Broad-spectrum antibiotics]:::action D --> E E --> F[Emergency laparotomy]:::action F --> G[Repair/Graham patch]:::outcome ``` ## Key Point: **Perforated peptic ulcer is a surgical emergency.** Once diagnosis is confirmed (pneumoperitoneum + clinical signs), immediate surgical repair is indicated — there is no role for conservative management in acute perforation with peritonitis. ## Why Immediate Surgery? | Aspect | Rationale | |--------|----------| | **Peritonitis** | Established peritoneal contamination; risk of sepsis/shock | | **Hemodynamic instability** | Indicates advanced shock; requires urgent source control | | **Mortality** | Increases ~1% per hour of delay after perforation | | **Imaging** | Diagnosis already confirmed; further imaging delays definitive care | ## High-Yield: **Resuscitation + Antibiotics + Surgery** is the standard triad. Antibiotics must be started immediately (within 1 hour), but they do NOT replace surgery — they are adjunctive. ## Clinical Pearl: In a hemodynamically unstable patient with confirmed perforation, do not delay for additional imaging. The diagnosis is secure; the patient needs the operating room. 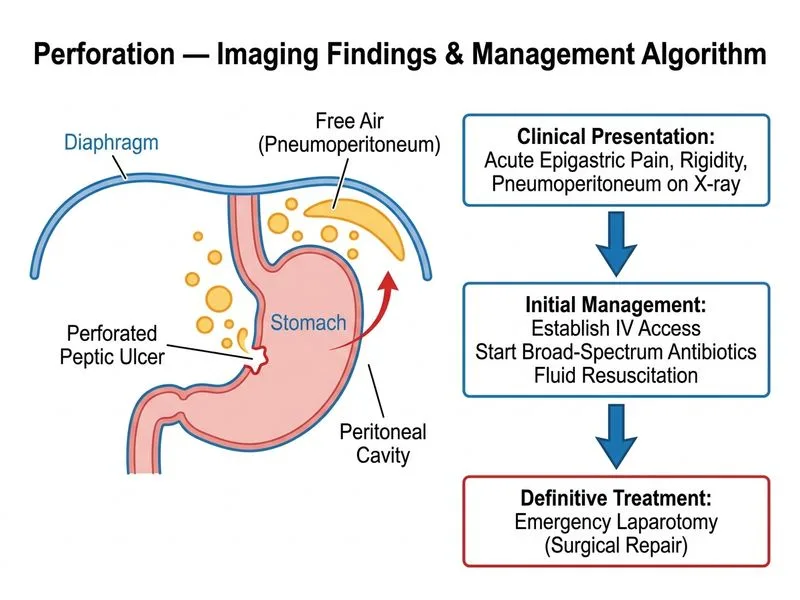
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.