## Clinical Scenario Analysis This patient presents with **perforated diverticulitis with a small localized abscess** — characterized by: - Contained perforation (localized abscess, not generalized peritonitis) - Hemodynamic stability (BP 118/76, HR 92, Temp 38.2°C) - **Small abscess (3 cm)** — below the 4–5 cm threshold for percutaneous drainage - Minimal free fluid, no generalized peritonitis → **Hinchey Stage I** ## Management Strategy for Perforated Diverticulitis ```mermaid flowchart TD A[Perforated diverticulitis]:::outcome --> B{Generalized peritonitis + unstable?}:::decision B -->|Yes| C[Emergency laparotomy]:::urgent B -->|No| D{Abscess size?}:::decision D -->|Small < 4-5 cm, stable| E[Antibiotics alone + serial observation]:::action D -->|Large ≥ 4-5 cm or not responding| F[Percutaneous drainage + antibiotics]:::action E --> G[Reassess; elective resection if recurrent]:::action F --> G C --> H[Primary resection or Hartmann]:::action ``` ## Key Point: **Hinchey Classification guides management:** | Hinchey Stage | Finding | Management | |---|---|---| | **I** | Pericolic/mesenteric abscess (small, < 4–5 cm) | **Antibiotics alone + observation** | | **II** | Pelvic/distant abscess (≥ 4–5 cm) | Percutaneous drainage + antibiotics | | **III** | Purulent peritonitis | Emergency surgery | | **IV** | Fecal peritonitis | Emergency surgery | ## Why Antibiotics Alone (Option C) is Correct Here? 1. **Abscess size is 3 cm** — below the 4–5 cm threshold that mandates percutaneous drainage per current guidelines (ASCRS 2020, WSES 2020) 2. **Hemodynamically stable** — no indication for emergency surgery 3. **Localized peritoneal signs** — no generalized peritonitis (Hinchey III/IV) 4. **Standard of care for Hinchey I**: Broad-spectrum antibiotics (e.g., piperacillin-tazobactam or metronidazole + ciprofloxacin) with serial clinical examinations; percutaneous drainage is reserved for abscesses ≥ 4–5 cm or those failing antibiotic therapy 5. **Evidence base**: Multiple RCTs and meta-analyses (including the AVOD trial) support non-operative management with antibiotics for small contained abscesses ## Why NOT Percutaneous Drainage (Option D)? Percutaneous drainage is indicated for **Hinchey II** (larger pelvic/distant abscesses ≥ 4–5 cm). A **3 cm abscess** is below this threshold and is typically managed conservatively with antibiotics alone. Drainage carries procedural risks (bleeding, bowel injury, tract infection) that are not justified for small abscesses amenable to antibiotic therapy. The original answer (Option D) incorrectly applied Hinchey II management to a Hinchey I scenario. ## Why NOT Emergency Laparotomy (Option B)? Emergency surgery is reserved for Hinchey III (purulent peritonitis) or Hinchey IV (fecal peritonitis), or hemodynamic instability — none of which are present here. ## Why NOT Diagnostic Laparoscopy (Option A)? Laparoscopy is not a standard step in the management algorithm for stable Hinchey I diverticulitis. CT imaging has already characterized the extent of disease adequately. ## High-Yield: **For Hinchey I diverticulitis (small localized abscess < 4–5 cm) in a hemodynamically stable patient, broad-spectrum antibiotics with serial clinical monitoring is the standard first-line management.** Percutaneous drainage is reserved for larger abscesses (≥ 4–5 cm, Hinchey II) or failure of antibiotic therapy. (ASCRS Clinical Practice Guidelines 2020; WSES Jerusalem Guidelines 2020) ## Clinical Pearl: The **4–5 cm abscess size threshold** is the critical discriminator: abscesses below this size are managed with antibiotics alone (Hinchey I), while larger abscesses require percutaneous drainage (Hinchey II). Emergency surgery is reserved for generalized peritonitis (Hinchey III/IV) or hemodynamic instability. 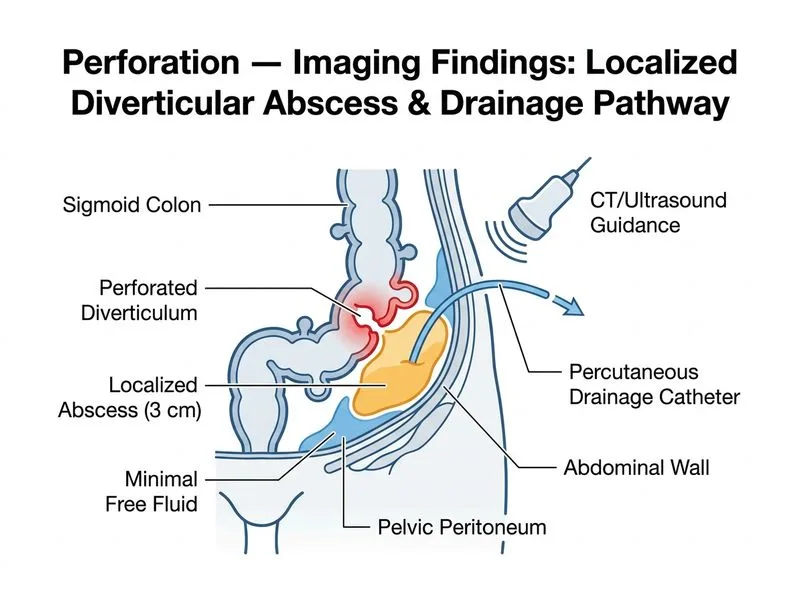
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.